The journalists at BuzzFeed News are proud to bring you trustworthy and relevant reporting about the coronavirus. To help keep this news free, become a member and sign up for our newsletter, Incoming.
As the US marched steadily toward 200,000 recorded deaths from COVID-19, President Donald Trump returned to a familiar line that he has pushed since the start of the pandemic: “It is going away.”
In reality, COVID-19 is not going away — certainly not before an election that for many will be a referendum on Trump’s handling of this crisis.
Over the past six months, the US has played a massive game of whack-a-mole with the coronavirus, temporarily taming its spread in one place only to have it flare up somewhere else where stringent controls on viral transmission were either never put in place, or were relaxed before it was safe to do so.
This patchwork spread of COVID-19 has kept the world’s most powerful nation in the coronavirus’s grip, as shown in these animations tracking its spread as it killed 200,000 Americans across the country since March.
Weekly coronavirus cases
This map shows the weekly rate of new confirmed COVID-19 cases per 100,000 people for what the US Census Bureau calls “core-based statistical areas.” These consist of a county or combination of counties containing at least one city with at least 10,000 people. While some rural areas that are grayed out in our map have also been hit hard by COVID-19, this geographical view clearly reveals the shifting patchwork of hot spots of viral transmission that has characterized the US epidemic so far.
As testing has expanded across the nation, the meaning of a “case” has changed: Those identified today include many people with mild or no symptoms who would not have been tested in the early days. (Read the methods to learn how we set the color scale so that the map still highlights the initial outbreak in and around New York City.)
The animation reveals the restless pattern of what the Atlantic’s Ed Yong in May dubbed America’s “patchwork pandemic.” Unlike countries in Europe, Asia, and Oceania that were able to enact nationwide measures to limit the spread of the virus, the US never took a coordinated national approach.
Instead, individual states, cities, and counties temporarily got things under control, only for the virus to find susceptible populations elsewhere, especially in places with limited restrictions on gatherings and no face mask requirements.
“This is just spreading from place to place to place, and it’s going to continue to do that,” Kate Grabowski, an epidemiologist at Johns Hopkins University, told BuzzFeed News.
In part, the patchwork pandemic in the US is a consequence of the US federal system, which gives autonomy to states. But epidemiologists and health policy experts fault the Trump administration for failing to develop a strong national infection-control strategy and to coordinate with state and county health departments to tackle the crisis head-on.
“One of my major concerns about the pandemic response is that we’ve never had a united plan for the United States,” Howard Koh of the Harvard T.H. Chan School of Public Health, formerly assistant secretary of health in the Obama administration, told BuzzFeed News.
Instead, individual state and local governments have taken the lead on when and how to lock down and reopen. Even after New York City and other parts of the Northeast were hit hard in April, lockdowns elsewhere were inconsistent and often short-lived.
Encouraged by Trump, states across the South and West rushed to open bars, restaurants, and other businesses in May, despite failing to meet White House and CDC guidelines for reopening.
“We didn’t have a consistent imposition of public health measures,” Ezekiel Emanuel, vice provost of global initiatives at the University of Pennsylvania and a former health policy adviser to the Obama administration, told BuzzFeed News. “And then we rushed to open up things like restaurants and bars.”
The result was the surge in cases across the Sun Belt states that took off from mid-June, clearly visible in the animation after early infection hot spots around New York City, New Orleans, and Detroit had calmed down.
New local outbreaks have continued to emerge. Right now, some of the worst affected areas are in Wisconsin — where cases have surged in 18- to 24-year-olds in recent weeks.
“We have this rolling thunder of waves of illness across the country,” Koh said.
A lack of leadership at the federal and state level also means that the nation has missed on opportunity to systematically gather information on which interventions are most effective in curbing viral transmission, according to Jessica Metcalf, a demographer at Princeton University who studies infectious disease dynamics.
“We still don't have a robust sense of what works to reduce transmission, and how this scales with the costs,” Metcalf told BuzzFeed News by email.
Weekly coronavirus deaths
This animation of COVID-19 deaths highlights the enormously high death tolls in April in New York City and the surrounding area in particular.
Death rates are now lower in part because doctors have gotten better at treating the people who are most seriously ill. We now know that putting people on ventilators is less helpful than was initially thought. Laying severely ill patients face down seems to help, as does treatment with steroids and the antiviral drug remdesivir, given emergency approval on May 1.
Still, the shifting hot spots highlight tragedies that have hit already disadvantaged local communities, including high death rates among Native Americans in counties including Navajo, Arizona, and McKinley, New Mexico — and more recently in the border communities of southeast Texas, where large numbers of people in the Latino community have died.
Across the nation, Black Americans have disproportionately been infected and died: The patchwork pandemic has underlined the nation’s stark racial and economic divides.
Daily coronavirus cases and deaths
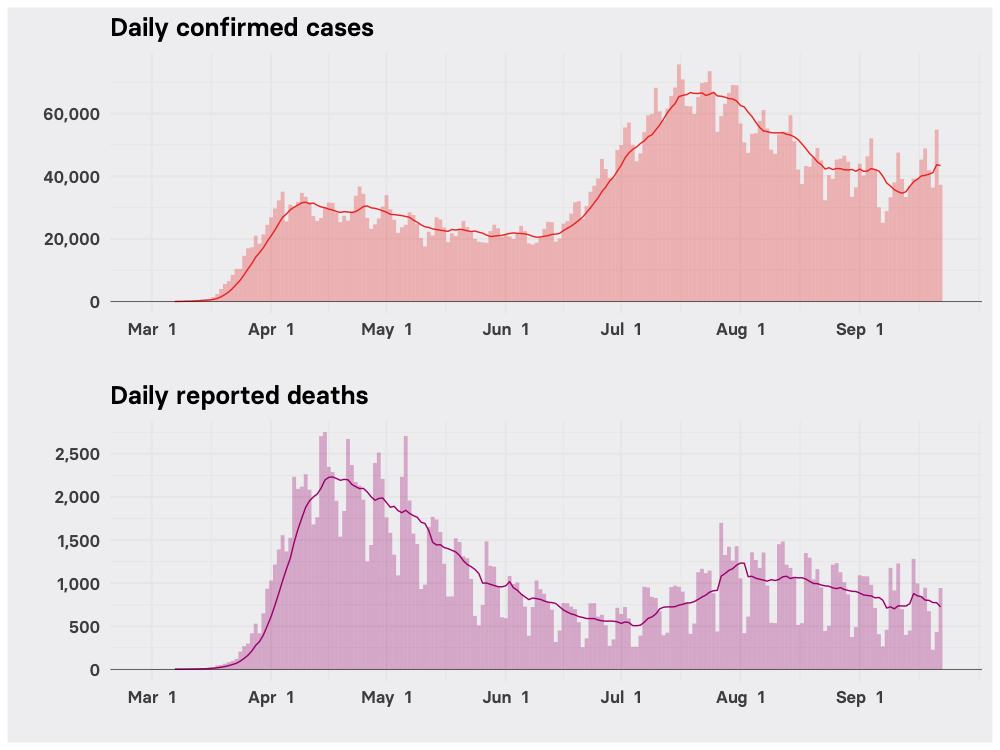
These charts show the daily counts of cases and deaths for the nation as a whole. While European countries including the UK, France, and Spain are now wrestling with a significant “second wave” of COVID-19 after months with relatively few cases, the US never had any respite over the summer months.
Instead, the patchwork pandemic has given the US an ongoing roller coaster of infections and deaths. And over the past couple of weeks, new confirmed cases have been trending up once again.
Experts warn that this roller coaster will continue, with outbreaks likely to return to places where the virus has already wrought havoc once before. “It’s everywhere. It’s an endemic disease at this point,” Grabowski said. “I think we’re certainly going to see increases in infections in New York City and Florida again.”
The big hope is that an effective vaccine can finally bring things under control — not eliminating the virus, but turning it into something we can live with.
“If we can eventually get a vaccine that is widely available and effective, there’s a chance that this ‘patchwork’ that you describe can be curbed; however, that’s a big ‘if,’” Maia Majumder, a computational epidemiologist at Harvard University, told BuzzFeed News by email.
Right now, Trump is butting heads with senior health officials in the administration over his desire to get a vaccine approved before the election, pushing back against safeguards to ensure that candidate vaccines are only approved for the public after rigorous processes to determine their safety and efficacy.
Few experts think a massive rollout across the majority of the population can happen before the third quarter of next year, even if things go well. “I keep saying November 2021,” Emanuel said.
Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, has said a vaccine that is 75% effective would be unlikely to achieve the herd immunity needed to finally stop rampant transmission of the coronavirus and allow us to resume something like our previous lives if only two-thirds of Americans take it.
And a growing worry is that many people won’t take a vaccine. According to a September poll from the Pew Research Center, just 51% of Americans said they would definitely or probably take a vaccine if it were available today. That level of hesitancy exceeds the hardcore of committed anti-vaxxers and seems to reflect wider concerns that approval may be rushed before safety has been fully established.
“I think the hesitancy reflects the politicization,” Emanuel said.
Jeremy Singer-Vine contributed reporting for this story.
