The journalists at BuzzFeed News are proud to bring you trustworthy and relevant reporting about the coronavirus. To help keep this news free, become a member and sign up for our newsletter, Outbreak Today.
The Food and Drug Administration authorized two malaria drugs boosted by President Donald Trump to treat COVID-19 in March based on threadbare evidence, according to an agency review obtained by BuzzFeed News through a Freedom of Information Act lawsuit.
The review also raised serious questions about shoddy practices at overseas factories that manufactured and donated the drugs for use in American hospitals, according to the documents.
The use of the drugs to treat COVID-19 has been politically charged from the start.
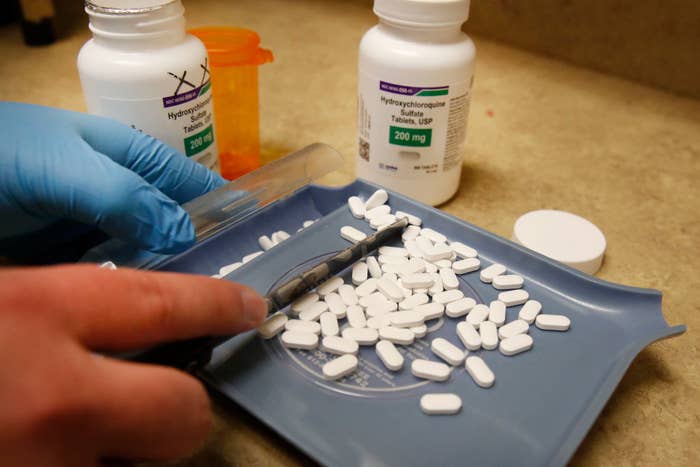
On March 19, as the number of coronavirus cases in the US started to surge, President Donald Trump called for widespread use of the two drugs, chloroquine phosphate and hydroxychloroquine sulfate, to treat the new disease, for which there is no known cure. Nine days later, the FDA issued an emergency use authorization (EUA), a special provision that allows the agency to quickly greenlight the widespread use of unapproved drugs during a public health emergency, allowing the malaria drugs to be used to treat hospitalized COVID-19 patients.
Medical experts, meanwhile, raised concerns about the drugs saying they could cause serious health issues and were not proven to work. Even the FDA issued a warning, four weeks after its authorization, cautioning that use of the drugs outside hospitals could cause “life-threatening” heart problems.
Then, a top science official in the Trump administration alleged that the emergency authorization was dangerous and came about as a result of political pressure. Rick Bright, director of the Biomedical Advanced Research and Development Authority, claimed he was pressured to sign off on the EUA, and was retaliated against after raising safety concerns about the malaria drugs and their importation from low-quality factories in India and Pakistan. “There wasn't sufficient data at the time to support the use of this drug without close physician supervision," Bright told Congress, after filing a whistleblower complaint in May.
Days after that, President Trump stunned the nation by announcing on live television that he was taking the drugs himself. “What do you have to lose?” he asked.
The FDA documents, released publicly now for the first time, outlined what data the agency used to make the hot-button decision to allow widespread use of the drugs.
The EUA review, conducted by six FDA officials, referred to only two studies of the malaria drugs, which either showed negligible results or have since been called into question altogether.
If you have any information to share about this story or anything else relating to the coronavirus, email dan.vergano@buzzfeed.com or reach out via one of our secure tipline channels.
At its center was a controversial French study that claimed that the malaria drug, combined with an antibiotic, was very effective at treating coronavirus infections. That study has since been criticized because of numerous problems, including failing to include the outcomes of patients on the drugs who died or were hospitalized. Two weeks after the study was published, the publisher issued a notice saying the study did not meet its "expected standard."
The FDA review also cited a small Chinese trial of 30 patients that showed the drugs had little to no effect on patient outcomes, and a letter from Chinese scientists that said it was effective — but was not backed up with any data. The review also included a reference to 16 clinical trials that were still underway and noted that many doctors had a “substantial interest” in trying the drugs.
According to the review document, officials briefly warned about the risks of giving the drugs to patients with heart problems as part of a longer section detailing warnings and precautions. “Chloroquine- or hydroxychloroquine-related cardiac conduction disorders (i.e. QT prolongation, ventricular arrhythmias) are rare but life-threatening adverse reactions and are usually associated with long-term use and high cumulative doses,” officials wrote.
The document also reviewed the risks posed by the millions of doses of the drugs that were donated for use in the US. Analyzing the 1 million chloroquine tablets donated to the US by Bayer Pharmaceuticals, the review noted they were made at never-inspected factories in India with “a low reputation for quality.” The pills were made by a manufacturer in India whose other factories had failed previous FDA inspections. That meant, “facilities used to manufacture this chloroquine are presumed to have even lower standards of quality.”
A chemical analysis of the chloroquine pills conducted on March 27, also among the public records, indicated the tablets contained small impurities but met standards.
“Based on the scientific evidence available to FDA, it is reasonable to believe that these products may be effective in treating the serious or life-threatening disease, COVID-19,” the FDA officials concluded.
“At least we have some hints now of what they were depending on" for the EUA, said Peter Lurie, a former FDA executive who now leads the advocacy group Center for Science in the Public Interest. "It still seems to me to be a thin read and one is left with the question of whether the approval had something to do with pressure from the White House."
Since the review was submitted, growing evidence has suggested that these drugs may do more harm than good. After a second clinical trial involving the drugs was recently halted, French, Italian, and Belgian officials last week all banned the use of the drug as a therapy for the novel coronavirus.
“I think it's fair to ask whether the FDA — expert in assessing drug data — should or could have spotted those issues,” Ohio State University law professor Patricia Zettler, former FDA associate chief counsel during the Obama administration, told BuzzFeed News by email. Zettler added, however, that the standard for an emergency use authorization is always low.
Here is a copy of the federal review of the EUA application for the malaria drugs as a possible COVID-19 treatment outside of clinical trials:
CORRECTION
This post has been updated to note the French study cited by the FDA review has been criticized by its publisher, not formally retracted.


