Gastroenterologist Colleen Kelly performed her first poop transplant eight years ago, on a young woman with a life-threatening gut infection who had run out of options. The bacterium Clostridium difficile had invaded the woman's gut, bringing her constant diarrhea and pain, and antibiotics weren’t working.
Kelly’s patient persuaded her to try a fecal transplant, in which poop from a healthy person is put into a sick person’s colon in the hope of resetting the mix of microbes there. At the time, it was considered a fringe therapy, but had seemed to cure many patients with C. diff infections, even though no one quite understood why.
The patient’s boyfriend provided fresh stool, and Kelly introduced half a cup of it into her patient via a colonoscopy. To Kelly’s surprise, it worked — by the next day, the woman’s symptoms began to wane.
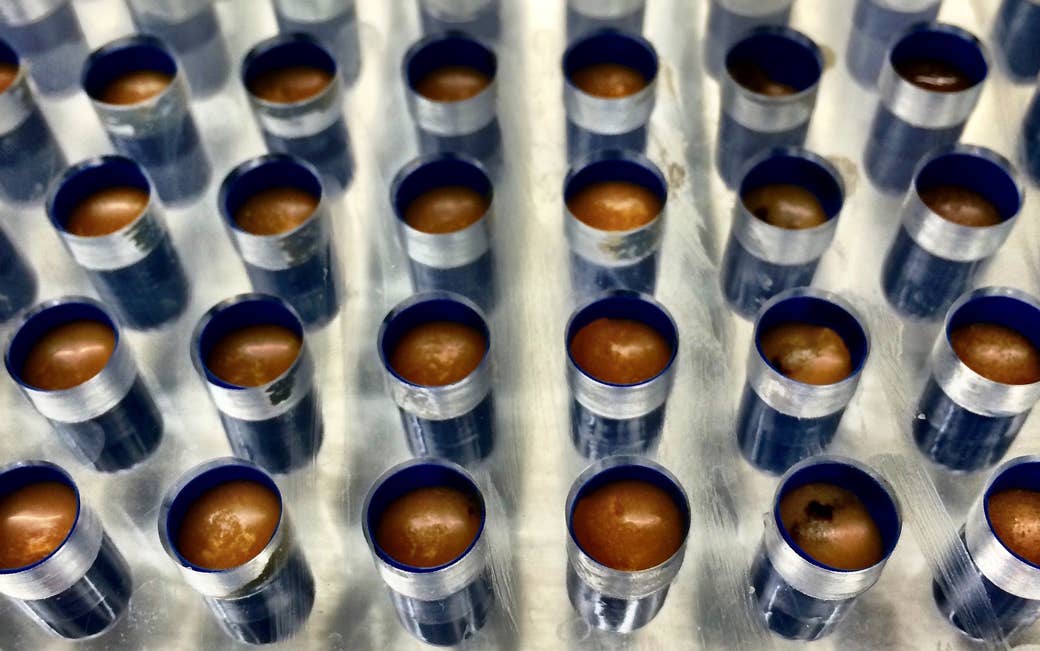
Kelly, an assistant professor of medicine at Brown University, has since performed some 300 fecal transplants for C. diff infections. These days, she usually buys healthy stool samples from OpenBiome, a nonprofit “stool bank” in Somerville, Massachusetts that launched in 2013. “It’s really unlike any therapy to date,” she told BuzzFeed News.
So this spring, when the FDA announced that it intended to tighten its rules on the procedure, known as fecal microbiota transplantation (FMT), making it harder for doctors to buy stool from banks, Kelly was among the commenters who wrote back, opposing the proposal.
The new rule could limit FMT to large hospitals, meaning that many fewer patients would have access to it, Kelly and a group of colleagues from the American Gastroenterological Association wrote. “Further, it may inadvertently encourage patients to perform ‘do-it-yourself’ FMT without medical supervision, using FMT material that has not been properly screened.”
Other doctors also chimed in, stressing that patient safety was at stake.
“If the FDA makes it prohibitively difficult for clinicians to work with stool banks, I believe this will actually make the procedure less safe, and of course, less accessible,” wrote Sarah McGill, a gastroenterologist at the University of North Carolina Medical School who has performed about 30 fecal transplants on C. diff patients in the last two years. Her freezer at work, she told BuzzFeed News, is full of poop samples bought from OpenBiome for $385 a pop.
Poop wasn’t on the FDA’s radar until about 2013, when a landmark study showed that a fecal transplant offered relief in 94% of extreme C. diff. cases. As more gastro docs started doing the procedure — not only for C. diff. infections, but Crohn’s disease and irritable bowel syndrome — OpenBiome arrived, suddenly offering a ready, frozen solution to clinics hunting for healthy donors.
In May 2013, citing concerns about safety and a lack of research, the FDA ruled that it would regulate poop (and the bacteria in it) not as a natural substance from the body, like blood or skin, but rather like a pharmaceutical drug, requiring rigorous safety testing before clinical use. After an uproar from gastroenterologists, the FDA granted an exemption to the new rule: Doctors could continue transplanting donated poop for extreme C. diff. infections.
But now the rules are changing again. The FDA’s new proposal would require that even for C. diff. treatments, doctors submit extensive paperwork for each patient needing a sample from a stool bank — treating the sample as an “investigational new drug.” (This rule would apply only to poop from stool banks, on the grounds that a tainted sample there could affect many others. But the additional red tape would not apply to C. diff. patients who get poop from a friend or relative, or from small stool collections stored in hospitals.)

The FDA has received more than 100 impassioned comments from doctors, scientists, and patients against the new rule. Because the treatment is not covered by insurance, patients and clinics in poorer states would be particularly hard hit, a doctor from Mississippi wrote. The procedure “saved my child's life,” one Virginia parent wrote, and a stool bank was critical in making it possible. An anonymous patient offered: “My colon. My choice.”
But one company, at least, welcomes more government regulation of stool. Rebiotix, a startup based in Minnesota that is developing an enema treatment of bacteria extracted from poop, told the FDA to shut down the stool banks and adopt the strictest regulation possible in dictating how samples are procured. The company contends that this is for the patients’ own good, as stool banks may not be fully screening their samples for diseases.
Rebiotix is also worried about its bottom line. If the company’s poop-like drug for C. diff makes it through the rigorous clinical trial process before anybody else, it would win the rights to be an exclusive seller of the product for seven years, gaining a huge lead in a market expected to be worth $1.5 billion by 2024. (The company declined to say how much its product would ultimately sell for, but a 2015 internal Rebiotix report obtained by BuzzFeed News forecasted a price range of $3,000 to $10,000.)
So far, results look good: In 2014, Rebiotix announced the results of a “Phase 2” trial that tested the product on 34 patients with C. diff, and found that it worked in 87% of them. A more rigorous trial, in which patients received either Rebiotix’s product or a placebo, was completed this year, and results are expected this fall.
From Rebiotix’s perspective, OpenBiome is selling a competing product — but gets to bypass the hassle and expense of clinical trials.
“We hope that the FDA comes back soon and makes those other companies go away, because it makes it hard for those of us that want to conduct good work [and] publish data,” Rebiotix founder Lee Jones told BuzzFeed News. The company told the FDA that it has had trouble enrolling patients in its clinical trials because they’d rather try the stool banks. “There’s no consistency and there’s no way for us to gather the data we need.”
The stakes are even higher now that Rebiotix’s chief competitor, a Massachusetts company called Seres Therapeutics, dropped out of the race last month after reporting dismal results for its lead product, a pill containing certain strains of bacteria extracted from stool.
Depending on how the approval is handed down, Rebiotix could very well put outfits like OpenBiome out of business, Rachel Sachs, a health and law professor at the Washington University at St. Louis, told BuzzFeed News.
“There is no room in this space for pettiness and competitive-ness.”
That’s an outcome that patient advocates are hoping against. “There is no room in this space for pettiness and competitiveness,” patient advocate Catherine Duff, who founded the Fecal Transplant Foundation, told BuzzFeed News.
It could be several years until Rebiotix is able to sell its product, and until then, Duff said, “OpenBiome is saving a lot of lives.”
Part of everybody’s worry is that if doctors aren’t able to perform the procedure with carefully chosen samples, patients will just do it at home under less safe conditions.
“Right now there’s nothing that prevents you from starting a stool bank in your garage,” Kelly, the gastroenterologist from Brown, said. “There needs to be some regulation here, the question is how best to do it.”
Following the FDA’s most recent guidelines, OpenBiome says it only sells to researchers, hospitals, and doctors. And even the stool bank acknowledges that some FDA standards regarding safety would help.
“There are 6,000 videos out there talking about: ‘This is how you should blend your poop,’” Carolyn Edelstein, director of policy and global partnerships at OpenBiome, told BuzzFeed News. “I think that should be pretty terrifying to regulators,” she said.
The FDA declined to comment on the status of proposal, and Kelly does not expect to hear a resolution any time soon. Edelstein, meanwhile, suspects that the FDA’s decision will coincide with an approval of a poop-derived drug like the one tested by Rebiotix. But OpenBiome is bracing for a verdict that could upend their entire business model. “That will definitely shift the way we work,” Edelstein said.
