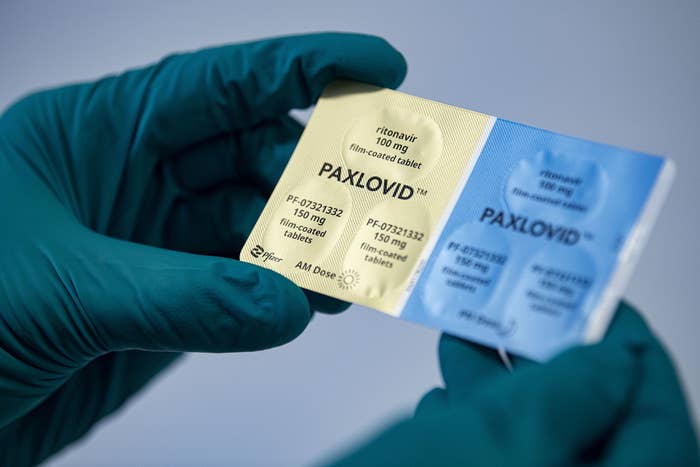
It seems the US has entered another phase in the pandemic where everyone around you is testing positive for COVID a first, second, or even third time. But this go-around is a little different. Now, we have powerful antiviral treatments that are actually pretty easy to access if you meet the criteria for use.
In December 2021, the FDA authorized the use of Paxlovid, the first oral medication that helps keep adults and children at risk of developing severe COVID alive and out of the hospital while also shortening recovery time and reducing coronavirus spread.
Just one day later, the FDA authorized a second oral drug called Lagevrio (molnupiravir), which has a similar benefit but is not nearly as protective as Paxlovid, which was 88% effective against COVID-related hospitalization and death among the vulnerable in a clinical trial.
“I think the number one thing to know is that Paxlovid is still proving to keep vulnerable and high-risk people and others out of the hospital,” Dr. Michael Mina, chief science officer at eMed, a digital platform that offers at-home testing and telemedicine services, told BuzzFeed News. “This drug is one of the pillars of getting us out of this pandemic — not because it makes the virus disappear, but because it changes the risk equation at a societal level.”
The use of Paxlovid and other treatments may help explain why hospitalizations and deaths have not mirrored the recent increase in COVID cases nationwide.
More than 22,000 people are hospitalized with COVID in the US, and about 250 are still dying every day as of June 3. These stats come more than two weeks after the US grimly surpassed the 1 million deaths mark.
Last week, there was a peak in the seven-day average with more than 110,000 new daily cases, although experts warn COVID’s true prevalence may be underestimated as more and more Americans rely on home tests.
Here’s everything to know about Paxlovid, including how it works, side effects, the risk of possible rebound infections, and where you can get a prescription.
When should you take Paxlovid and what are the side effects?
Paxlovid is used to treat mild-to-moderate COVID in adults and kids ages 12 and older who test positive for the coronavirus and face high risks for hospitalization and death. People at high risk include those who are unvaccinated or who have cancer, heart disease, high blood pressure, obesity, diabetes, neurodevelopmental disorders, asthma, and more.
The full treatment consists of three pills taken together twice a day for five days. You must start the treatment as soon after your COVID diagnosis as possible, and definitely within the five days since your symptoms started.
Waiting too long means you miss a window of opportunity and it may not work as well or at all.
To get Paxlovid, you’ll need a prescription from your doctor. You shouldn’t take the drug before a COVID exposure or after to prevent an infection (unless you are COVID positive), or if you are already hospitalized with severe illness.
Two of the three pills you take consist of nirmatrelvir, which blocks the coronavirus from making copies of itself. The third pill is ritonavir, which helps nirmatrelvir stay in your body for a longer period at high concentrations.
Like any drug, Paxlovid has side effects, one of the most common being a weird, metallic taste in your mouth. Others include diarrhea, high blood pressure, and muscle aches.
If you have either uncontrolled/undiagnosed HIV or liver or kidney disease, you should not take Paxlovid. Paxlovid can also have potentially harmful interactions when combined with other medications, including some blood thinning drugs, such as warfarin; antidepressants like bupropion and trazodone; herbal products like St. John’s wort; antibiotics like erythromycin; and others.
How effective is Paxlovid against severe COVID?

Mina called Paxlovid’s efficacy of 88% against COVID-related hospitalization and death “an astounding metric.”
In a study of 2,085 unvaccinated adults with a preexisting medical condition (or just older age), just 8, or 0.8%, were hospitalized with COVID or died from any cause compared with 66, or 6%, of those who took a placebo.
The good news is that it appears Paxlovid is holding up in real-world settings.
A non-peer-reviewed study of nearly 94,000 older or immunocompromised COVID patients in Hong Kong published May 17 found that people treated with Paxlovid had a 21% reduced risk of hospitalization.
Another non-peer-reviewed study published June 1 found Paxlovid was associated with a 67% and 81% drop in COVID hospitalizations and deaths, respectively, in people ages 65 and older. (But the benefits were not seen in younger adults.)
Although the drug has only been studied in unvaccinated people, there’s no reason to believe it won’t work as well in vaccinated people, Mina said.
“People who are vaccinated who are getting a breakthrough infection are just like anyone else who's getting a viral infection,” Mina said. “Having a drug that's going to massively reduce viral replication will, by all accounts, reduce hospitalization and mortality in anyone who gets infected, regardless of their vaccination status.”
Rebound infections can happen after Paxlovid
You may have heard that some people taking Paxlovid can have “rebound infections,” which is when people who finish their five-day Paxlovid treatment test positive again about two to eight days after testing negative.
Symptoms may not always reappear, but they certainly can, according to a CDC health advisory issued on May 24.
Case reports so far show rebound infections after taking Paxlovid are mild and tend to improve or resolve within about three days; none have been severe. The CDC said there’s no evidence to suggest more treatment is needed either with Paxlovid or other available therapies.
Still, rebound infections can contribute to further coronavirus spread, although how much is unknown. Plus, they are generally inconvenient, sending people back into isolation for a recommended additional five days plus 10 days of mask-wearing after rebound symptoms begin.
There’s still much to learn about why rebound infections are occurring, but Mina speculates that Paxlovid treatment isn't long enough to fully erase the virus from people’s systems.
“The drug could be serving as a crutch during your actual infection, so when you stop taking the drug, your immune system is taken by surprise as though it's a new infection all over,” Mina said. “If we just left the drug in for a few more days, it might actually give the body enough time to kill all the virus off.”
Dr. Albert Ko, the Raj and Indra Nooyi professor of public health at the Yale School of Public Health, told BuzzFeed News that it’s possible that a reservoir of virus somewhere in the body remains untouched by Paxlovid and causes the resurgence in symptoms and/or positive test results days after treatment ends. This theory may be extra likely in people who naturally have higher viral loads to begin with.
Mina said it’s likely health officials will consider extending Paxlovid treatment duration to 8 or 10 days.
The CDC said “a brief return of symptoms may be part of the natural history” of a coronavirus infection in some people, regardless of treatment with Paxlovid.
Omicron may be to blame, too, Mina said. Omicron is more infectious and immune evasive than Delta, so it’s possible your immune system is having a harder time working with Paxlovid to rid yourself of COVID.
People also experience Omicron symptoms earlier than past variants, Mina said, which means they also begin Paxlovid treatment earlier in their infection. So there’s a chance we’re not giving our immune systems enough time to develop a robust response to the treatment.
The CDC, as well as both Mina and Ko, still recommend Paxlovid for nonhospitalized people at high risk for severe COVID.
How does Paxlovid compare to other COVID treatments?
A number of treatments exist for COVID, but whether one is better than the other depends on the patient's medical needs and history, the availability of treatments, and the variants spreading in a given region.
What’s clear, however, is that Paxlovid has become the first-choice therapy for many people.
The National Institutes of Health’s COVID treatment guidelines state that Paxlovid is the preferred treatment for nonhospitalized patients. Next in line is remdesivir (brand name Veklury), which is given intravenously and has been shown to be 87% effective against COVID hospitalization and death among nonhospitalized patients at high risk for severe disease. Remdesivir also can be used in hospitalized patients.
Another treatment is bebtelovimab, a new monoclonal antibody, which can be given to nonhospitalized patients if Paxlovid or remdesivir aren’t available or are not safe for the patient. There isn’t any efficacy data for bebtelovimab yet, but the NIH said it’s “active” against all Omicron subvariants in laboratory settings.
While you could also take Lagevrio, the other new antiviral pill, studies show it’s only about 30% effective against COVID-related hospitalization and death, so it should be used as a last resort.
How to get Paxlovid
The Biden administration launched a “Test to Treat” initiative on March 8 that allows people to get tested for COVID at a pharmacy-based clinic, government health center, or long-term care facility and get antivirals like Paxlovid right away if the test is positive.
People are allowed to receive only Lagevrio and Paxlovid through the clinics participating in the initiative, which are free regardless if you have insurance or not.
Here you can find locations near you that are part of the Test to Treat initiative.
You can also visit your doctor (if you have one) who can prescribe Paxlovid, which you can pick up at a local pharmacy.
If you take a rapid COVID test at home and it comes out positive, you can get a free telemedicine visit via eMed, Mina said, during which a medical professional can prescribe the treatment. (You must first buy a rapid test from eMed, however — the rest is free.)
It wasn’t long ago that Paxlovid supplies couldn’t meet demand in the US, but Pfizer officials have increased production in recent weeks. The initial scarcity prevented many doctors from prescribing the medication, Mina said, because there was a lack of information on its use that came along with it. “It just led to this massive misunderstanding of this really powerful drug for months,” he said.
The number of prescriptions for Paxlovid has increased from about 64,000 each week at the end of April to about 184,000 a week by the end of May, a Health and Human Services spokesperson told BuzzFeed News via email.
About 300 Test to Treat sites have also been added since the beginning of May, with a total of about 2,600, which is expected to grow, the spokesperson said.
Can Paxlovid reduce the likelihood of developing long COVID?
Although no data has been collected on whether Palovid can lower your chances of developing long COVID, both Mina and Ko agree we should expect that it can and will.
“We should anticipate that early aggressive treatment to squash the viral load and kill the virus off before it really gets a big hold of you should absolutely reduce long COVID symptoms,” Mina said. “Just the mere fact of keeping the viral load to a very low number, that alone should really drive a better outcome in terms of a reduced likelihood of long COVID.”
Ko admits we don’t yet understand the mechanism behind why some people develop long COVID, but knowing the associations between the condition and viral load, “it’s highly plausible” Paxlovid can help on this front.
Does Paxlovid work against different COVID variants?
The clinical trial that determined Paxlovid’s efficacy was conducted between July and early December, before the more infectious Omicron variant dominated the pandemic in the US. This means what we know about Paxlovid’s virus-fighting abilities are based on infections with the now-defunct Delta variant.
But the fact is that all variants are and will be susceptible to the drug, Mina said. That’s because it targets a different part of the coronavirus that, at least where Omicron is concerned, isn’t being affected by mutations.
“It’s so easy to get caught up in the noise and hear all the negative stuff, but at the end of the day, the trial results weren't wrong,” Mina said. “People are still having their lives saved by Paxlovid.”
This does not mean, however, that future variants cannot develop a resistance to the drug, both Mina and Ko said, although the CDC noted that there is no evidence this is occurring.
