
No one was prepared for the coronavirus pandemic.
The public certainly wasn’t. The US government wasn’t. Even the public health experts who had spent their entire careers anxiously preparing for a pandemic weren’t, in part because the basic mechanics of the coronavirus now known as SARS-CoV-2 defied expectations. The virus didn’t spread the way experts thought it would. And COVID-19 looked wildly different in different people, making it difficult to spot.
"It’s an extraordinary virus, the likes of which I’ve never, ever seen, and I’ve been doing this now for almost 40 years,” Anthony Fauci, director of the National Institute of Allergy and Infectious Diseases, told BuzzFeed News. “I’ve never seen a virus that on the one hand has no symptoms in one person but on the other hand can be absolutely deadly for another person. That is really quite unprecedented."
Doctors and scientists raced to understand the basic nature of the coronavirus and how to treat severe infections. Meanwhile, the general public has craved answers, often turning to a panoply of imperfect sources: anecdotes, preliminary studies, officials, and the internet.
The swirl of misinformation, conspiracies, and conflicting official guidance, a problem exacerbated by President Donald Trump, made the situation even more confusing. Trump routinely dismissed and played down the threat; ignored, mocked, contradicted, and interfered with guidance from his own public health experts; and touted unproven treatments. The result was a deadlier pandemic, one that has already claimed more than 320,000 lives in the US.
But a year after the virus first appeared, there’s reason for hope: Two vaccines are already in distribution. An explosion of studies has deepened our understanding of the virus, and doctors and nurses, with months of experience under their belts, are better able to identify and treat infected patients.
Here’s a look at what we’ve learned:
1. The virus was circulating in China as early as November and in the rest of the world by January.
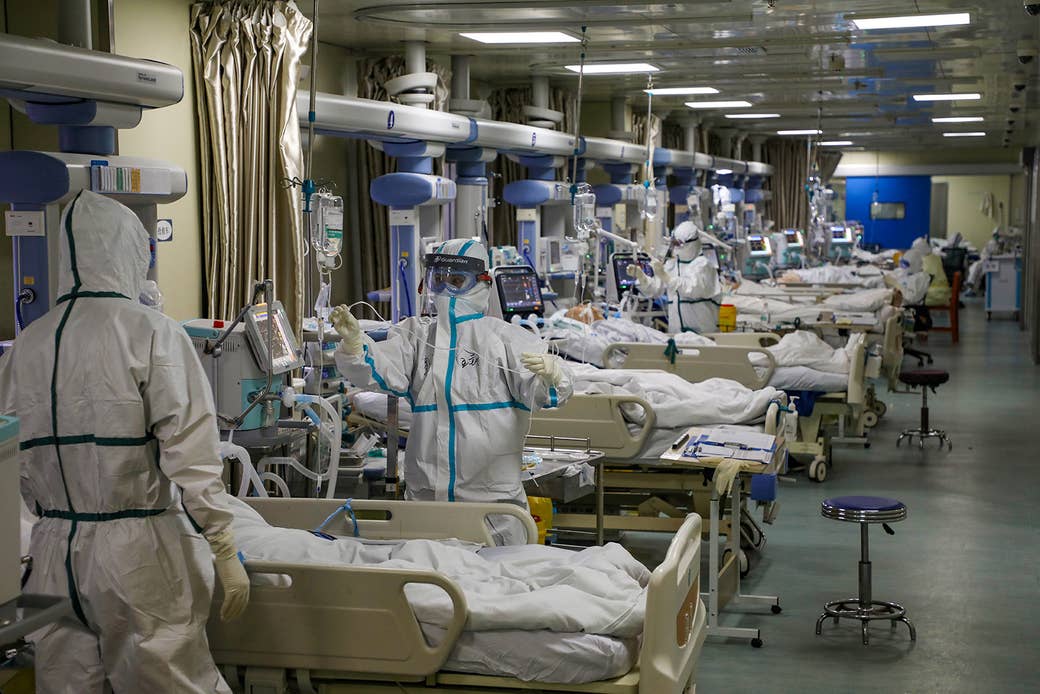
The earliest warning of the coronavirus’s threat hit the world on Dec. 30, 2019, with a report describing four cases “of pneumonia of unknown cause” in China.
“My initial gut response was ‘uh-oh,’” said Marjorie Pollack, an infectious disease expert who wrote the first alert for the ProMED early warning system. “Having lived through the SARS outbreak” that struck China in 2002, she recalled by phone, “there was just a feeling of déjà vu.”
Initially, the origin of the coronavirus was tied to an outbreak among people who had been at the Huanan Seafood Wholesale Market in Wuhan, China, in late December 2019. Coronaviruses are bat viruses, and rumors quickly swirled around bats sold for soup at the wet market.
However, even by the end of January, it was reported that cases were first diagnosed in China as early as Dec. 1, 2019, meaning the virus was spreading in November. Comparing the rates of mutation in genetic maps of the virus taken from people as the coronavirus spread worldwide, researchers at the Fred Hutchinson Cancer Research Center in Seattle pointed to a first “index” COVID-19 case in a person happening in China in November, when “hidden transmission of the virus was likely widespread.”
As far as the US, cases were likely already loose in January, according to a June CDC report. Some researchers have argued the first US cases could have been spreading as early as the third week of December, though this is disputed.
That is where the trail stops — and both China and the US have made it difficult to find out more.
From early on in the year, President Donald Trump and Secretary of State Mike Pompeo have pushed the idea, popular on right-wing outlets like Fox News, that the virus originated in a Wuhan lab that studied coronaviruses in bats. Scientists have vehemently argued that there is no evidence of this — and that the genetics of the virus point strongly against it being lab-made.
The political blame has added to tensions with China’s leaders, who have not revealed any more about the origins of the virus since March. After a long delay, a new World Health Organization team began investigating the virus’s origins in October in partnership with Chinese researchers. President-elect Joe Biden has indicated that he’ll cooperate more with international efforts — he has already committed to reversing Trump’s withdrawal from the WHO — and scientists are hopeful that will improve efforts to figure out how the virus came to infect humans. Discovering the answer is crucial not only for this pandemic, but for preventing the next one.
2. COVID-19 can look very different from person to person.

In the early months of the pandemic, doctors, and nurses looked for three key symptoms to best identify people potentially sick with COVID-19: fever, cough, and shortness of breath. But as more people got infected, it became clear the virus could attack different parts of the body, causing a wider range of symptoms.
Today, the CDC warns of 11 main symptoms to watch for: fever or chills, cough, shortness of breath or difficulty breathing, fatigue, muscle or body aches, headache, new loss of taste or smell, sore throat, congestion or runny nose, nausea or vomiting, and diarrhea. There’s no set order in which they appear. Moreover, there’s an ever-growing list of other potential impacts too, from swollen toes, dubbed “COVID toes,” to neurological injuries.
If a doctor checks a symptomatic patient in person for the virus, they aren’t just looking at the lungs anymore, according to Megan Ranney, an associate professor of emergency medicine at Brown University. “We know to also look for markers of inflammation, markers of blood clots,” she said, adding: “We look at the heart, the brain, the kidneys, liver function — those can all be signs of COVID 19.”
Another quirk of this disease is that it can severely impact some people while leaving others unscathed. An estimated 20% to 30% of people infected with the coronavirus develop no symptoms at all. Meanwhile, many people can recover, only to be left with symptoms that can last for weeks or months. A German study from July found that 78 out of 100 COVID-19 patients had heart complications two months later, while an Italian study the same month found that 87% of patients who were sick enough to be hospitalized still had symptoms after two months.
3. People can be infectious even if they don’t have symptoms.
One of the sneaky things about this disease is that people can have no symptoms but still spread the virus to others without even knowing it. The current evidence that we have, Ranney explains, suggests that someone can spread the virus in the two days or so before developing symptoms (called presymptomatic spread), while asymptomatic people who never develop symptoms can also still infect others. The CDC warns that more than 50% of transmission is occurring by people that are either presymptomatic or asymptomatic.
The public health community was slow to understand and accept this. Early on, the flawed assumption was that sick people were overwhelmingly spreading the disease within their homes and communities. This thinking was informed by experience with other respiratory viruses, such as the flu. Health screens popped up everywhere, from airports to hotels, checking people’s temperatures and surveying for other symptoms in search of the ill and infectious, without much benefit. The California Department of Public Health reported that travel screenings of 11,000 people in that state, from February to March, turned up only three sick people.
“The lack of those symptoms is not a guarantee you are not infected, nor is it a guarantee you are not passing it on to others,” Ranney said. “That’s something that took us all by surprise.”
4. Masks work.

The scientific consensus now is incredibly clear: Since so many people without symptoms are unknowingly spreading the disease, widespread mask-wearing is a simple and effective way of curbing transmission.
“Wearing face masks has turned out to be one of the most important control measures,” Joe Gerald, an associate professor of public health policy and management at the University of Arizona, told BuzzFeed News.
The more people wear masks, the less the virus spreads. The main benefit comes when sick or infected people wear masks, and thus don’t spread as many virus particles into the air when they breathe, cough, sneeze, and talk. There’s some emerging evidence that masks also offer protection to healthy people that wear them, providing a barrier against breathing in virus particles lingering in the air.
Studies in the lab show that the most effective masks at reducing the spread of the coronavirus and other respiratory viruses are medical-grade ones, such as N95 respirators and, to a lesser degree, surgical masks; but cloth masks also offer protection. Additionally, a mix of observational and modeling studies published this year suggest wearing masks can cut down COVID-19 transmission on planes and other indoor settings, such as homes and restaurants, especially when combined with social distancing and handwashing. One CDC study focused on Kansas found infections declined over the summer in counties that mandated mask-wearing but increased in those that did not.
But, early on, health officials added to confusion about masks: Both the WHO and CDC initially said face masks were only needed for healthcare professionals, partly in a bid to ensure sufficient supplies for those working on the front lines of the pandemic. Facing immense pressure from scientists during the first deadly surge of cases and deaths, the CDC finally changed its recommendations in April, but the WHO did not follow suit until June.
When local officials started implementing mask mandates, however, there was pushback. Some people, especially Republicans, saw the move as an infringement of their freedom and the mixed messaging left them skeptical that masks worked. Trump stoked these tensions, refusing to wear a mask himself and mocking those who wore them, including then–presidential candidate Joe Biden. Driven by the politicization, misinformation about masks has continued to spread.
5. The virus can spread in the air.
A key way the coronavirus spreads is through tiny particles in the air that may linger for minutes or hours, and may spread farther than 6 feet from an infected person. This is yet another reason mask-wearing is important and why improving ventilation indoors is an important mitigation strategy.
Public health leaders were also late to acknowledge the virus could spread this way, rather than only by close contact. In July, 239 scientists sent a letter to the WHO, imploring them to consider mounting evidence that these small water particles, also called aerosols, could spread the virus in the air. The WHO partially acknowledged the existence of airborne transmission shortly afterward, stating then that it posed a threat to healthcare workers. The CDC only updated its transmission guidance to detail this risk in October.
Rather than focusing on air transmission early on, experts warned of the risk of people getting sick by touching an infected surface or object and then touching their eyes, nose, or mouth. People then stockpiled cleaning supplies, microwaved their mail, and wiped down their groceries, prompting a CDC warning about how using disinfectants on food packaged in cardboard or plastic wrap is unsafe. Experts now acknowledge this is not the main way the virus is spread.
6. Superspreaders are driving infections.

A small percentage of people are responsible for most coronavirus infections, study after study has shown. This sharply contrasts with the initial thinking, based on China’s experience, that the virus was mainly spreading in households.
For example, one study using contract tracing data determined about 20% of cases in Hong Kong were responsible for 80% of total cases. Another one focused on India concluded about 5% of infected people in the Tamil Nadu and Andhra Pradesh regions drove 80% of cases.
Because indoor gatherings pose a higher risk of infection, so-called superspreader events ended up grabbing headlines throughout the year. Prominent examples include when one person with COVID-19 symptoms ended up spreading the virus to 87% of the people in attendance at an indoor choir practice in Washington state; when dozens of people got infected and sick at large indoor weddings in Ohio and Maine; and when the 11th floor of a South Korea call center became a coronavirus hot spot.
Researchers still don’t know why some people are superspreaders of the virus and others aren’t. And while this is not how the flu is usually spread, clustering or superspreader events were responsible for the spread of other infectious coronaviruses, such as SARS and MERS.
7. Not everyone who is hospitalized needs a ventilator.
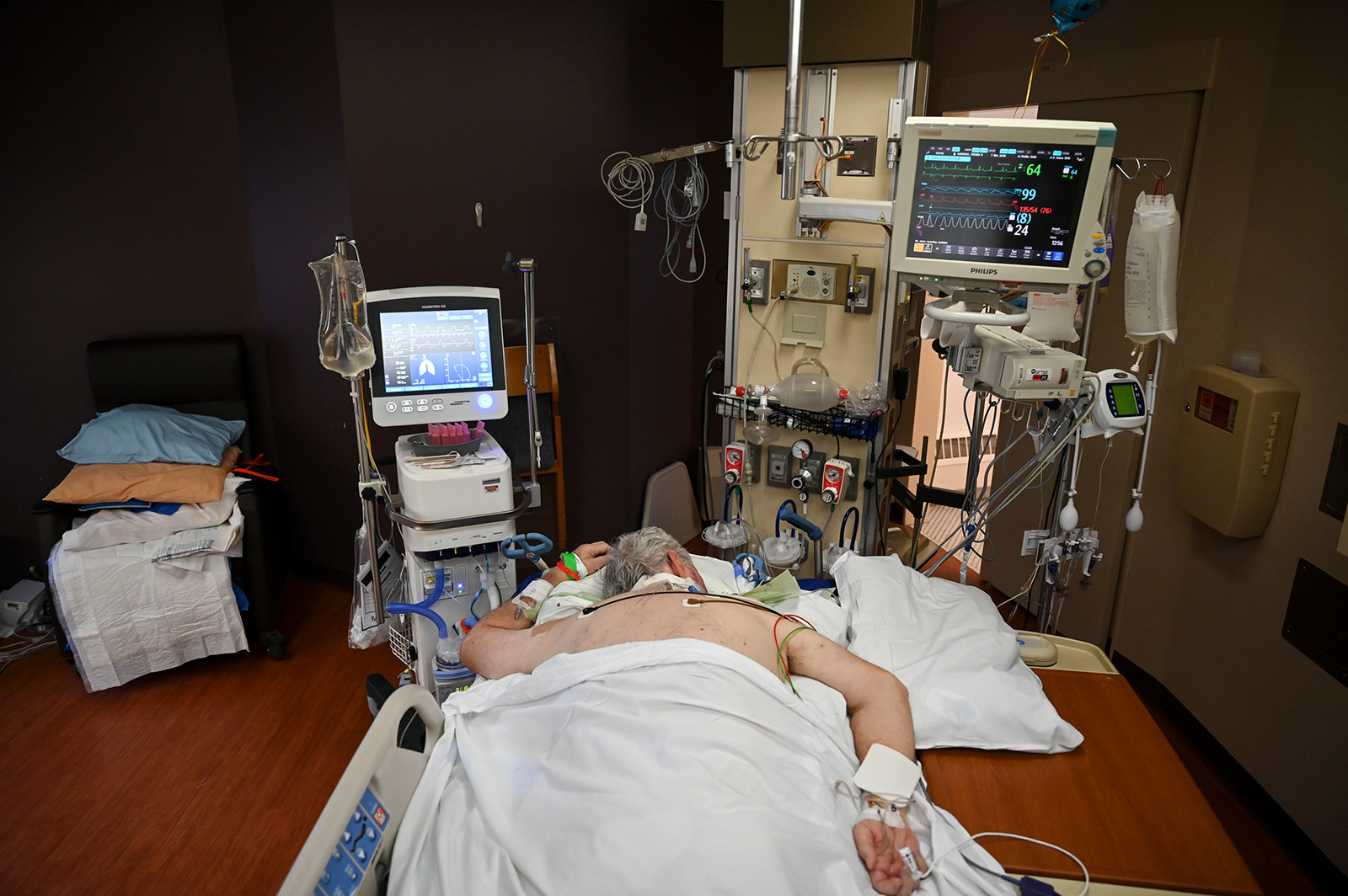
China’s crowded hospitals, filled with patients on ventilators, sent the early message that these breathing machines would be vital in treating people with the deadly disease, who in severe cases can struggle intensely to breathe on their own. Ventilators are still considered crucial, but better understanding of how COVID-19 kills many patients has lessened the crush for the machines.
Quickly putting coronavirus patients on ventilators was premised on two early ideas about SARS-CoV-2: One was that critical patients were going into “acute respiratory distress syndrome,” seen in pneumonia cases where a ventilator gives patients time for their immune systems to fight off an infection. The other was that patients were highly infectious late in their infections, like in the 2004 SARS outbreak, and that early intubation prevented patients from spreading germs by coughing on healthcare workers at the most transmissible moments of their case.
But it turned out that’s not how COVID-19 works. Instead, the patient's own immune system can turn out to be the most dangerous enemy, attacking the lungs in the late stages of the most serious infections. For this reason, the steroid dexamethasone, which tamps down the immune response, has become the go-to response for severe cases, shown to cut mortality by a third in patients on ventilators.
Likewise, we now understand that patients are most infectious around the time they first develop symptoms rather than days later when they are hospitalized. ICUs have turned to just supplying patients oxygen and “proning” them, or turning them onto their stomachs, which allows more air to enter their lungs, rather than sedating them and damaging their already-inflamed lungs with a ventilator.
The death rate for hospitalized COVID-19 patients seems to have declined since April, when many of these lessons about treating patients were first learned. An October Journal of Hospital Medicine study of more than 5,000 COVID-19 patients suggested that proning, less time on ventilators, and treatment starting sooner due to earlier testing, helped explain their death rate falling from 26% in April to 8% in August.
One interesting, but still unproven, theory is that more widespread wearing of masks means that people are now, more often, getting a lower initial dose of the virus. The immune system can battle fewer viruses more easily, leading to less severe cases and fewer deaths.
8. COVID-19 is worse if you have diabetes, heart disease, or cancer.
Old age appeared the key risk factor for dying from the novel coronavirus in the first reports of the outbreak from China. A February report on 72,000 Chinese patients for example found a death rate of 8% for patients in their seventies, and 15% for those older.
A more complicated picture emerged over the next few months, however, with illness that often came along with age — diabetes, heart disease, cancer — emerging as the crucial risk factor for patients. “Adults of any age with certain underlying medical conditions are at increased risk for severe illness,” said a November update on COVID-19 risks from the CDC.
That changed picture came from deeper looks at the critical cases in China, Europe, and New York as the pandemic spread. Since COVID-19 attacks many organs in the body, people with kidneys, hearts, or other organs already burdened by illness or obesity face higher risks of dying or of severe illness.
Because older adults have high-risk conditions at very high rates, the CDC’s advisory panel on vaccines has recommended those over 75 get shots ahead of others.
9. It’s also a bigger risk if you are pregnant.

The CDC’s early guidance suggested that pregnant people and fetuses didn’t have an elevated risk in response to COVID-19 infections.
Now we know that, if you are pregnant, COVID-19 poses a serious risk. “Based on what we know at this time, pregnant people are at an increased risk for severe illness from COVID-19 compared to non-pregnant people,” the CDC now warns. “Additionally, pregnant people with COVID-19 might be at increased risk for other adverse outcomes, such as preterm birth.”
Data collected over the last year showed that infected pregnant people are more likely to be admitted into an intensive care unit, need a ventilator, and die compared to people who are not pregnant. To date, more than 42,000 pregnant people in the US have tested positive for COVID-19, more than 8,000 of them have been hospitalized, and at least 55 have died, according to data collected by the CDC. Pregnant Latinx and Black people are more likely to get very sick from the virus.
There are still a lot of unknowns. “The majority of this data is from [people in their] third trimesters,” said Rahul Gupta, chief medical and health officer at March of Dimes, an advocacy and research group focused on maternal and baby health. It’s still unclear how infected people earlier in their pregnancies are faring, as well as their babies. And while limited studies suggest parents are not transmitting the virus to their children through the placenta or breast milk, March of Dimes is funding research to collect more data.
10. Kids are far less likely to get seriously sick.

The early observations out of China suggested kids only rarely got infected with COVID-19, and even then generally had mild cases. This initial picture wasn’t that far off: While it’s now clear children do get infected, and some seriously so, they are more often asymptomatic or mildly impacted. But it is still not well understood why this is the case.
Another open question is how much kids spread the disease. “The data right now strongly suggests that littler kids are less likely to spread the virus than older teens and young adults...and that young adults spread it at the same rate as full adults,” explained Ranney. But, she added, “there are a lot of contradictions in the data.”
An additional puzzle facing the medical community is why a small but growing number of kids of different ages, from toddlers up to teenagers, have been hospitalized for a coronavirus-linked syndrome, called multisystem inflammatory syndrome in children, or MIS-C. “Nobody read about this before. Nobody saw it coming. This is completely new,” Jane Burns, one of the researchers studying this syndrome, told BuzzFeed News in May.
The scientific questions around whether children faced risks from COVID-19 — and whether they were “silent carriers” — became deeply politicized amid fights about whether to reopen schools. While the Trump administration urged reopenings and threatened to withhold pandemic aid if states did not comply, Democrats raised concerns about schools turning into hot spots for infection. So far, research suggests that schools are not superspreading sites. Because of the consensus that opening schools is a priority and the risk of infection can be kept low through strict adherence to social distancing and other hygiene measures, the CDC this week prioritized teachers to be among the next group to receive COVID-19 vaccines.
11. We still don’t know how long immunity lasts, but there is reason to be hopeful.
An ongoing mystery surrounding the coronavirus is how long immunity to the bug lasts, either after recovering from an infection or getting a vaccine. Immunity to four other common coronaviruses that cause common colds wanes within a year or two. Since the coronavirus has been loose in humanity for only a year, we don’t know whether it lasts longer than that.
Reports of reinfections have shown that, for some people, immunity doesn’t last. But only a few hundred reinfections have been reported worldwide.
Because 95% of people produce antibodies to infection, some kind of long-lasting immunity is expected among the 17 million COVID-19 cases counted, so far, in the US. The two questions that have occupied scientists are: How long do antibodies last in the body? And do immune “memory” cells last for the years needed for long-term immunity to the virus?
The answer to the first question is that, for most people, the antibodies do seem to linger for five to seven months after an infection, leveling off but staying at a moderate level in the bloodstream, with higher levels seen after more severe cases. As for memory cells, their duration in numbers strong enough to deter an infection is more uncertain, again due to the length of time people have been getting sick with this virus. But there is reason to be hopeful: A study has shown that memory cells aimed against SARS, a closely related coronavirus, last for at least 17 years, while SARS antibodies seem to last for two. And studies have shown that SARS-CoV-2 infection does generate these memory cells, which rally antibodies when a virus tries to return.
This also has implications for COVID-19 vaccines, since it will be important to know how long immunity lasts after inoculation. Documents submitted by Moderna to the FDA for emergency authorization showed evidence that its vaccine led to a bounty of memory cells, seen at least two months after vaccination.
Moderna, Pfizer, and others are promising to track the antibody response generated by their shots for two years, gauging to see if they generate an immune response stronger or weaker than people who have recovered from an infection. That data could help us figure out how soon people may need booster shots for a COVID-19 vaccine.
12. The coronavirus will continue to steadily mutate.
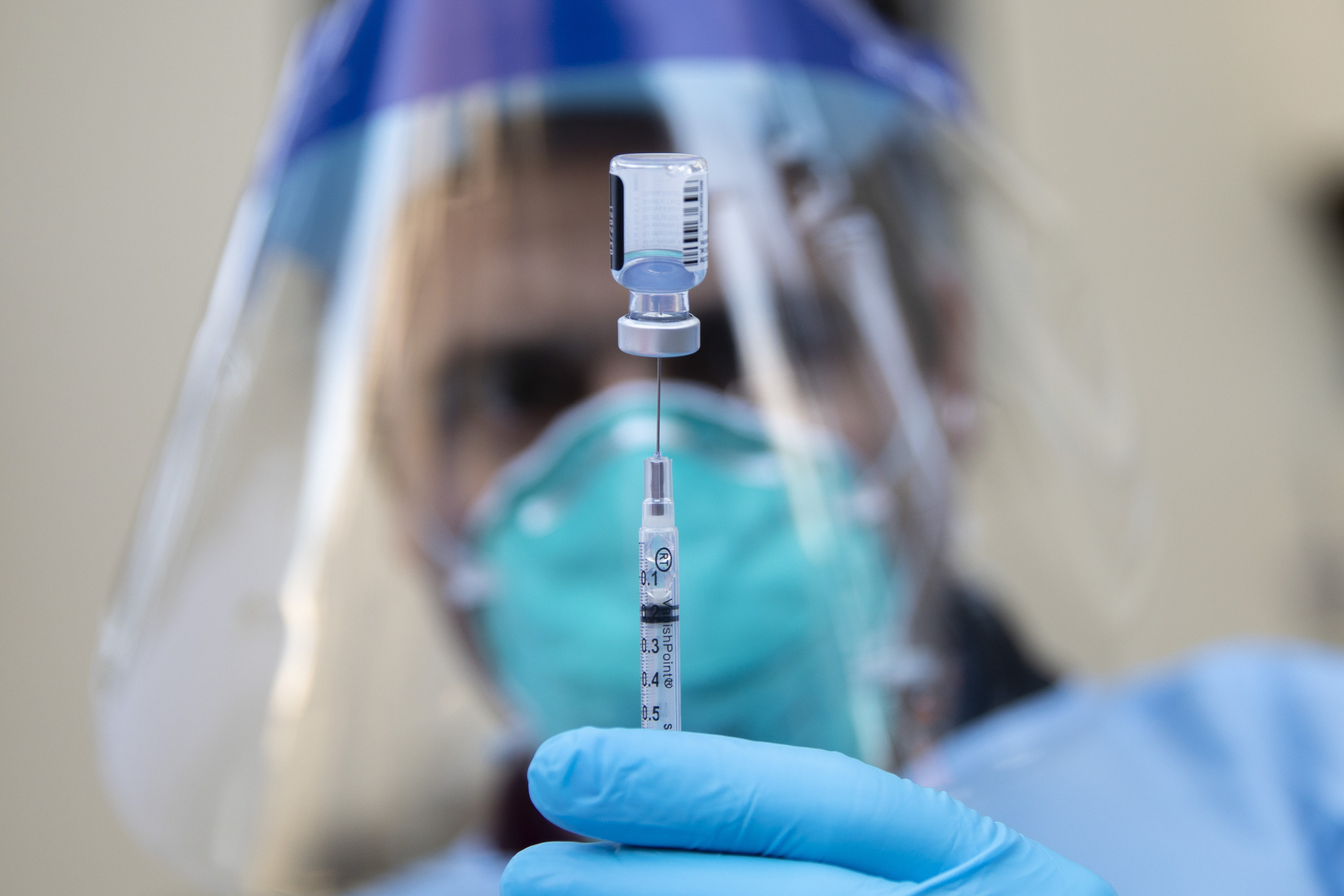
On Monday, Europe began banning travel from the United Kingdom, where a new, possibly more transmissible strain of the coronavirus has taken hold since September. This is not the first case of a new “variant” of the coronavirus emerging: As early as March, scientists observed that people in the US were infected with a virus that had mutations seen in cases in Europe, not China, suggesting that the virus had mutated at some point before taking hold in the US.
Whether these are truly new “strains” of the virus that are actually more dangerous or just ones that have taken over because of superspreader events — genetic lottery winners — is unclear. But it is known that the coronavirus steadily picks up small mutations as it infects people around the world. About one change in the virus’s genetic code crops up in a chain of infected people every 10 days, Trevor Bedford of the Fred Hutchinson Cancer Research Center estimated in March. And there have been a lot of chains of infection since then, with more than 75 million cases reported worldwide so far. Even by February, scientists reported more than 5,700 variants of the original Wuhan, China, virus were in circulation.
Prime Minister Boris Johnson described the virus as changing “its method of attack” to infect people even more readily, but whether this “B.1.1.7” variant of the coronavirus is truly more transmissible is hotly contested. The UK’s chief science adviser suggested on Saturday that the variant was 70% more transmissible than others. However, in response, virologist Christian Drosten of Berlin’s Charité University Hospital told Science magazine, “There are too many unknowns to say something like that.”
New influenza strains, functionally different versions of the same virus, do appear every year and necessitate seasonal changes in flu shots. The worry is that coronavirus will do the same thing, driving a need for changes in the COVID-19 vaccines just now becoming available. In particular, mutations to the “spike” protein of the coronavirus, the part that initiates infections of cells, are a concern, because COVID-19 vaccines by and large train the body to recognize and attack that part of the virus.
Coronaviruses actually mutate much more slowly than the notoriously sloppy flu, however, and with most of humanity still naive to the bug, there should be little evolutionary pressure to truly change its mode of attack. The B.1.1.7 variant, which has more than a dozen changes to its genetic code, is hypothesized to have emerged from a single, chronically infected patient who may have been treated with antibodies to the virus, encouraging it to develop more significant mutations.
Scientists are adding new variants to the list of things to watch carefully at this stage. Operation Warp Speed chief scientist Moncef Slaoui said on Monday that most likely the vaccines are just as effective against the UK variant as any other, but it will take weeks of studies to be certain. “There is no evidence this variant is more pathogenic,” he added.
13. Black, Latinx, and Native American people are dying at higher rates.

“We are all in this together,” President Trump and Vice President Mike Pence said in the March news conference unveiling the national response to the just-declared pandemic. But it hasn’t turned out that way. Black, Latinx, and Native American people have died in outsize numbers, at rates 2.6 to 2.8 times higher than white Americans.
In an October look at 114,000 deaths from COVID-19 this summer, CDC and New York City health officials found that 51% were white, 24% were Hispanic, and 19% were Black. Poverty, which can lead to living in multigenerational homes and doing essential work at higher risk for exposures, and higher frequency of diabetes, heart disease, and other health ailments, explains the increased susceptibility to dying from the coronavirus among minorities, that report concluded.
Perhaps the saddest finding is that minority children are likewise bearing a disproportionate burden as well. A September study of COVID-19 deaths in people 21 and younger nationwide found 75% of the deaths were among Black, Latinx, and Native Americans, even though they were just 41% of that population. Asthma and obesity were preexisting conditions most strongly tied to the deaths.
“COVID-19 has become the herald event that now fully exposes the deep and chronic social wounds in US communities,” Northwestern University’s Clyde Yancy wrote in a JAMA editorial in April. “This is a moment of ethical reckoning. The scourge of COVID-19 will end, but health care disparities will persist.” ●
Peter Aldhous contributed reporting to this story.

