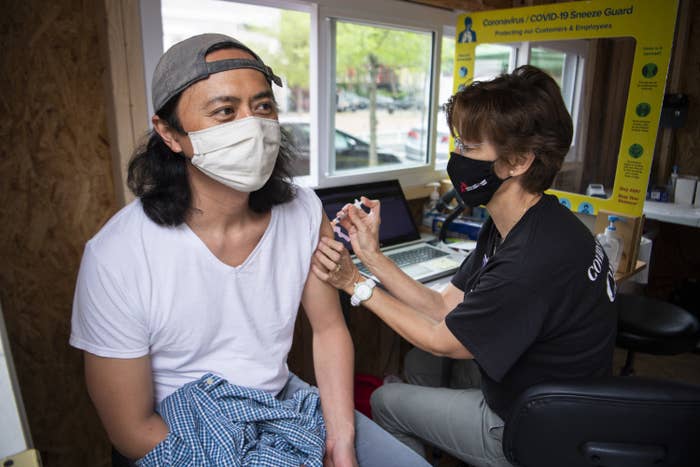
Federal regulators said Friday that distribution of Johnson & Johnson’s COVID-19 vaccine would begin again in the United States, following a vote from a CDC advisory panel.
The advisory panel’s 10–4 vote paved the way for the FDA and the CDC to lift a week-and-a-half-long pause on the single-shot vaccine after it became linked to a handful of highly unusual and severe blood clots.
The manufacturer and the FDA said that an updated warning about the risk of clots would be distributed to clinicians and patients via factsheets.
"We have concluded that the known and potential benefits of the [vaccine] outweigh its known and potential risks," said FDA acting commissioner Janet Woodcock in a statement. The two agencies will continue to monitor the vaccine.
To date, a total of 15 women have had the rare blood-clotting symptoms — including 3 who died — out of nearly 8 million vaccinated people, which amounts to 1.9 cases per 1 million doses.
That apparently very low risk for people in general — along with a slightly higher risk for women under 50 — instilled confidence in most of the members of the Advisory Committee on Immunization Practices, a group of independent vaccine experts who make recommendations to the CDC. Panelists said in a six-hour Friday session that in contrast to a week ago, they felt reassured that the vaccine could be safely given to the vast majority of people, given the remote odds of the clots and the lives that would be saved by the vaccine.
But the split vote reflected some members’ desire to explicitly warn women of the risk of clotting and to offer them an alternative vaccine. Others said that option would be confusing, impractical for many vaccination sites, and might needlessly discourage people from getting immunized.
“I acknowledge, as does everyone else, that these events are rare, but they are serious,” said José Romero, chair of the committee and secretary of the Arkansas health department, who voted yes. At the same time, he said, clinicians have an individual responsibility to inform the public about its risks.
Shots will restart as soon as Saturday morning, said Peter Marks, director of the FDA’s Center for Biologics Evaluation and Research, in a press conference on Friday night. Over 9 million of the shots made by Janssen Pharmaceuticals, a J&J subsidiary, are available for administration in the US, according to a recent White House briefing.
But its rollout has been delayed by the pause as well as high-profile manufacturing snags. Up to 15 million potential doses were ruined by contamination and other quality-control problems at a contractor’s plant in Baltimore, as detailed by a recent Food and Drug Administration inspection report, and new production remains paused at that facility per the FDA’s request.
At ACIP’s last emergency session, on April 14, the group declined to vote either way on what to do with J&J’s vaccine, saying that they wanted more time for any additional cases beyond the initial six to come to light. Earlier this week, European regulators recommended that both that vaccine and AstraZeneca’s COVID vaccine be restarted with a warning label. Both have been tied to similar blood-clotting syndromes, but the benefits of vaccination were found to outweigh the “extremely rare” risks.
On April 13, US regulators recommended the pause, which took effect in all 50 states, in order to buy time to investigate the cases and to advise doctors on how to treat them.
The 15 confirmed cases, including the 6 people who triggered the pause in the first place, developed an unusual combination of clots, most often and most dangerously in the brain, and low levels of clot-forming platelets within eight days of vaccination on average, CDC officials said.
It’s still unclear how the vaccine causes these seemingly contradictory symptoms to develop together. Michael Streiff, a hematologist at Johns Hopkins University, called them “extraordinarily rare.” “I’ve just never seen it,” he said, referring to his own experience treating patients. (In the general US population, blood clots and low platelets occur together naturally at an annual rate of 0.7 to 1.6 times out of every 1 million people.)
Most of the women affected — 13 of the 15 — were under age 50. That amounted to 7 cases per 1 million doses given to women of that age, according to the CDC’s analysis. Three have died, 7 have been hospitalized, and the rest were discharged.
Common symptoms at the beginning of these cases were headaches, chills, fever, nausea, lethargy, and abdominal pain. A typical medication for this type of clot — a blood thinner called heparin — may actually harm patients and should be avoided, regulators have told doctors. Heparin was not taken by any of the women who died. A key point made by some panelists was that the headaches marking the syndrome typically started six days after vaccination and initial symptoms worsened over the following days, which would give patients time to seek out treatment.
After the pause was lifted, CDC director Rochelle Walensky said that the agency had been communicating about these risks and warning signs with clinicians — “especially with providers of young women,” she said, singling out the American College of Obstetricians and Gynecologists — and would continue to do so.
During the advisory panel meeting, CDC staffer Sara Oliver presented a risk-to-benefit analysis, suggesting that resumption of the J&J vaccine would lead to 26 to 45 more clotting cases but prevent as many as 3,500 ICU admissions and 1,400 deaths over a six-month period.
Panelists debated a couple of options: recommending that the vaccine not be given to anyone, or only to adults over 50; recommending that everyone be eligible, with a warning label accompanying the vaccine; and recommending that everyone be eligible, while making women under 50 aware of the increased risk of blood clotting. In the end, the panel voted to reaffirm use of the vaccine after the FDA and manufacturer said that updated warnings for clinicians about the clots would be included with the shot once it resumes use and that patients would be told in fact sheets.
“I have no problem with the continued availability of this vaccine. I think if someone makes an informed consent after having and knowing the risks involved, I’m fine, let them get it,” said Pablo Sanchez, a member of the committee and professor of pediatrics at Ohio State University. But he voted no in opposition to “making a blanket recommendation,” saying, “I think we have to have stronger language and make sure people are informed appropriately.”
When the pause was initially announced, most medical and health experts praised it as an endorsement of the national vaccine surveillance system’s ability to quickly detect rare side effects and of regulatory agencies’ dedication to safety. “I think this pause was essential to our ability to inform the public, inform physicians, and to acquire more data for presentation and for analysis,” Romero said.
But public willingness to take the vaccine plunged, and after ACIP postponed voting last week, some observers were critical of the pause being indefinitely and universally extended. Taking J&J out of play for the entire US while new, transmissible variants are rapidly spreading, they argued, was a net negative for public health.
Compared to the Pfizer and Moderna vaccines, J&J doses made up less than 5% of the nation’s supply at the time of the pause. But this vaccine, authorized in late February, has advantages the others lack: It requires one shot, not two, and can be stored in refrigerators, not freezers. While it was available, it helped clinicians reach individuals who would have been hard to find for a second shot or who were vaccine hesitant, including rural residents, conservatives, people of color, and people experiencing homelessness. More than half of jurisdictions in a CDC survey said that they had been focused on administering it to people who were homeless, homebound, and incarcerated.
After months of constrained vaccine supply overall, the US is now approaching a turning point where its volume of doses outstrips demand, with 52% of adults having received at least one shot and everyone 16 or older eligible. Ensuring everyone is fully protected, not just the most eager and motivated, will be crucial to achieving herd immunity, experts say.
Clinicians serving people experiencing homelessness told BuzzFeed News that they were relieved at the vote.
“This was a major pathway to vaccination for a lot of the people we serve that was just closed off for a week and a half, and now it’s open,” said Van Yu, chief medical officer of Center for Urban Community Services, a New York City nonprofit. For some people, “this allows them to get vaccinated, and otherwise it wouldn’t have happened.”
Because most adults who are homeless are men, Yu doesn’t anticipate needing to discuss the possibility of blood clots with the majority of his clients. With young women, though, he said that he would be upfront about the 7-in-1 million risk and guide them to another site if they were uncomfortable with those odds. “All we have is the numbers,” he said.
In Chicago, Stephan Koruba, a senior nurse practitioner at the Night Ministry, will find out soon whether his clients will be receptive to J&J post-pause, as his organization is holding a vaccination event this weekend. Having fewer people to follow up with will allow his tired team to focus on reaching more people, he said.
“That’s going to help us and allow us to keep serving and doing what we need to do to get people off the street and off drugs,” he said.
UPDATE
This study has been updated with reaction from Van Yu of the Center for Urban Community Service and Stephan Koruba of Night Ministry.
UPDATE
This post has been updated with news of FDA and CDC reinstating administration of the vaccine.
