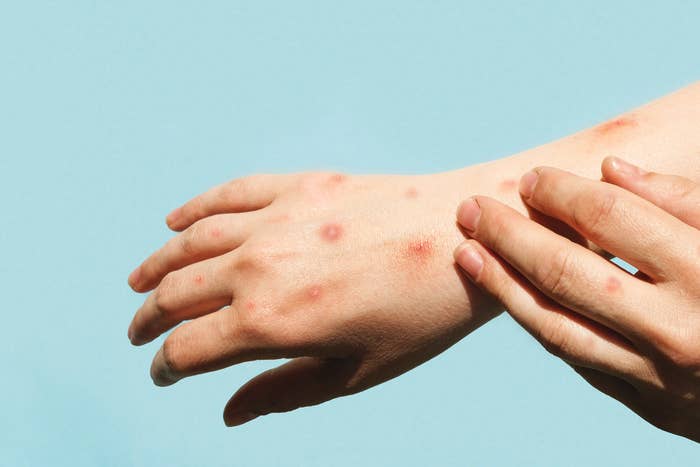
The World Health Organization declared monkeypox a public health emergency of international concern on July 23, voicing a specific concern for those who might be at high risk of getting severely ill from the virus, including children, pregnant people, and those who are immunosuppressed.
As of Aug. 18, there have been at least nine cases of monkeypox in children in the US. The first two were announced on July 22, one in California and another in Washington, DC. A few days later, there were two pediatric cases announced in Indiana, then another in California, then one in Maine. Most recently, three children tested positive in Florida, Texas, and Oregon, all within a two-day period.
Yet, even when making these seemingly game-changing announcements, public health experts continue emphasizing that the vast majority of cases they are seeing are still in men who have sex with men. Overall, 98% of cases in the US have been in men and 93% of cases have been in men who’ve reported recent sexual contact with other men, said CDC Director Dr. Rochelle Walensky at a White House press briefing on August 18th. At the moment, public health officials say that this is the community that needs more attention and access to vaccines and testing.
Of the two children with monkeypox reported by the CDC in July, one was a toddler in California, and the other, an infant who was an international visitor from the United Kingdom, was being treated in Washington, DC. Both were treated with the drug tecovirimat (Tpoxx), which is currently only available through an investigational new drug permit.
With summer nearly over and school starting for many, Monkeypox Twitter is concerned.
Parents and teachers are worried about how safe it is to go back to school. Others have unease that a large-scale pediatric outbreak could ignite a full-blown pandemic or could result in staffing shortages. And in one of the most widely shared sentiments, LGBTQ+ folks and allies fear that agencies’ continued focus on gay and bisexual men even as other people are contracting the virus puts LGBTQ+ people at risk for further societal ostracization, particularly those who work with kids.
Dr. Jennifer McQuiston, who is heading up the CDC’s monkeypox response, said they have experts looking into all potentials for how the virus could spread, including schools, daycares, and camps. But based on the data they’ve seen so far, McQuiston does not currently believe that schools have the potential to become monkeypox hot spots.
“It’s not something that we have a lot of concern about,” she said. “The occasional family transmission has been happening, but there is no evidence of spread within pediatric populations.”
In this current global outbreak of monkeypox, as of Aug.18, there have been 40,399 cases reported from 94 countries. That includes 14,115 in the US. The first pediatric cases announced in the US are not the first of this outbreak. According to the WHO, 107 children under 18, including 26 under age 5, have been affected around the world to date, including in the United Kingdom and Spain. There have been 12 deaths in adults, including four people in Nigeria, one in Ghana, one in India, two in the Central African Republic, two in Spain, one in Ecuador, and one in Brazil.
Here is a look into pediatric monkeypox, including information on how the disease is spread in the home, how to protect your family, and what is being done by schools to keep kids safe.
Is monkeypox dangerous to children?
While it’s thought that children could experience more severe illness with monkeypox than adults, that data is largely based on a more dangerous type of the virus than the one that is currently spreading in the US and other counties.
The CDC published clinical guidance for doctors on how to recognize and treat monkeypox in children that says children under 8 years old could have more severe symptoms, as can individuals who are immunocompromised or with certain skin conditions like eczema, burns, or severe acne. But again, that information is based on the more dangerous version of the virus. Data is limited from the one currently spreading around the world — although it is being compiled in real time. The CDC has said that the first children to test positive in the US have had relatively mild cases.
“While they became ill, they were not severely ill, and they appear to be doing well right now. I think, hopefully, the number of cases in kids is going to remain low,” McQuiston said.
For children, the most common symptoms of monkeypox are essentially the same as for adults — they include fever, headache, sore muscles, and malaise, followed by a rash that develops into pocklike lesions that can look like pimples or blisters. There can also be lesions inside the mouth, which could be mistaken for canker sores.
Are there treatments for monkeypox in children?
While there are therapeutics and vaccines available for children who contract or are exposed to monkeypox, they may be tricky to obtain.
Both the infant and the toddler who tested positive for the virus in the US have been taking the antiviral Tpoxx to help mitigate their chance of severe illness. The medication is currently only available through an investigational new drug permit, which requires patients to seek special approval and adhere to a series of doctor visits and health assessments.
Existing vaccines for smallpox (monkeypox is in the same family) have proven to be at least 85% effective at preventing transmission and can also help mitigate symptoms of the virus if administered after exposure, ideally within four days. Supplies of the preferred Jynneos vaccine remain limited, but appointments are being prioritized for recent exposures, including children.
in order to stretch this limited supply, the FDA announced an emergency use authorization on August 9 that would allow intradermal injections of the Jynneos vaccine for adults, which require only one-fifth the dose of the standard subcutaneous injections. The same authorization allows children at risk of monkeypox to get the vaccine, but only via the original subcutaneous delivery.
Some activists have said that this reactive approach to protecting children from monkeypox is not enough. Among them is Fatima Khan, cofounder of Protect Their Future, a grassroots organization working to ensure children are prioritized in public health policy; they led the fight to get COVID vaccines approved for children under 5. The organization released a statement on July 28 calling on officials to prioritize children and pregnant people in this monkeypox outbreak.
“We need to ensure that children are not left behind yet again,” Khan said. “Our government needs to lay out a plan immediately on how it will facilitate vaccinating children with the Jynneos vaccine.”
What do people who are pregnant need to know about monkeypox?
McQuiston said the CDC has “a lot of concerns” about monkeypox and pregnancy, particularly at the time of delivery. Pregnant people should take extra precautions to protect themselves from monkeypox, especially if they are close to their due date.
“We do have concerns that that could be quite a severe course,” she said.
The WHO has warned that monkeypox during pregnancy could result in the fetus being infected with the virus or, worst of all, a stillbirth. A 2017 study in the Journal of Infectious Diseases, which included four pregnant women with monkeypox, found that one had a healthy infant, two had early miscarriages, and one had a stillbirth. Thankfully, the infant recently born to a monkeypox-positive mother in the US seems to be doing well so far.
“Right now, the child appears to be healthy,” McQuiston said.
Can monkeypox spread in schools?
According to the WHO, none of the 107 children who have tested positive in this outbreak is believed to have contracted the virus in a school setting. Experts say monkeypox is more likely to spread at home than at school, and anyone who suspects the virus may be in their household should take precautions.
Examining possible means of transmission, the CDC remains focused on prolonged and personal contact, as is common with families living together. The CDC-confirmed pediatric cases announced in the US thus far are said to have been contracted from a family member living in the same household.
“We know monkeypox can spread through close contact, through cuddling, through kissing, through sharing utensils,” McQuiston said. “That’s why we recommend that if someone is diagnosed with monkeypox and they live with other people, that they isolate themselves.”
Anyone who believes they may have monkeypox is advised to avoid close contact with others, particularly children. If contact is unavoidable, as in the case of childcare, the CDC advises that caring family members wear gloves and masks. In any household with a presumed case of the virus, the agency recommends masking for everyone over the age of 2.
What are schools doing to prepare for monkeypox?
Even though health agencies are saying schools are not of primary concern for the spread of monkeypox, officials are preparing for the possibility.
As the summer heat begins to subside and schools start talking about reopening plans, Khan of Protect Their Future worries that children could become the primary drivers of this outbreak.
“Once monkeypox starts spreading in schools and daycares, the impact could be devastating,” she said.
There have already been a few such scares. The Illinois Department of Health announced on Aug. 5 that a daycare worker near Champaign-Urbana had tested positive for the virus. The news sparked concerns that the disease might spread to children at the center, but there has since been no known documented spread. On Aug. 12, Nevada’s Clark County School District said that an individual connected to Palo Verde High School in Las Vegas had tested positive for the virus, though there was no specification made as to whether the person was a student or staff member.
The New York City Department of Education represents the largest school district in the US with over 1 million attending 1,851 schools spread across New York’s five boroughs. The majority of these will reopen on Sept. 13.
Kaliris Salas-Ramirez sits on the department’s Panel for Educational Policy, which consists of 15 members appointed by the mayor and the city’s five elected borough presidents. She believes it is crucial for the panel to start talking about how to protect kids from monkeypox.
“We do need to have a plan, because we’re at a surge right now, and lord knows what that’s going to look like in the fall,” she said. “We need to start educating our children about monkeypox and what sorts of things they need to do to keep themselves safe.”
Salas-Ramirez, who is also a professor at the City University of New York’s medical school, said that COVID has presented a teachable moment for kids about how to protect themselves and their communities from viruses.
“Pedagogically, we try to remind the administration that this is a learning opportunity for children,” she said.
But she anticipates an uphill battle. Despite the fact that more than 40 children attending school in the New York City area have died of COVID, it has taken the panel more than four months to get a meeting with the city’s department of health about the upcoming academic year.
“A child cannot perform optimally if they don't feel well, if they don't have all of their needs met, but we keep having these conversations in isolation,” she said. “We don't talk about the intersection of these things. My concern is that we're going to make the same mistakes that we made with COVID, that we don't engage our communities.”
Mark Levine, the borough president for Manhattan who appointed Salas-Ramirez to the panel, agrees that the city needs to be prepared for all possibilities. Levine believes NYC’s first pediatric monkeypox case may be imminent.
“We have to prepare for the very real possibility that there will be a child or children in New York City who contract monkeypox,” he said.
When asked about potential monkeypox-related safety measures for public schools, Levine echoed the sentiments of public health agencies, that such a method of viral spread is unlikely.
“Health experts are saying that transmission to children is more possible in households and less likely in schools,” he said. “I talked to no experts who are calling for drastic measures in schools.”
So-called drastic measures aside, Levine would be in favor of a monkeypox educational campaign for everyone, including families with children. He would also support utilizing schools as possible locations for testing.
“I think we need to ramp up our education to the broader public about what monkeypox is and how it spreads,” he said. “I think the schools should be prepared first to be a source of clear information on this as it progresses.”
Public health messaging continues to focus on gay and bisexual men, even as cases are announced among children and pregnant people. Salas-Ramirez fears that many will use these words to justify their prejudices (one notable Republican politician has already leaped on the opportunity) or that some families without LGBTQ+ folks in their household may assume they aren’t susceptible.
“I am concerned that we are creating a stigma around monkeypox and implying that it’s just gay men who can get this virus,” she said. “That has been so compartmentalized for folks in a potentially dangerous way. They’re not really thinking about the public health repercussions this could have on our children.”
UPDATE
This story has been updated to reflect new confirmed cases of monkeypox in children.
