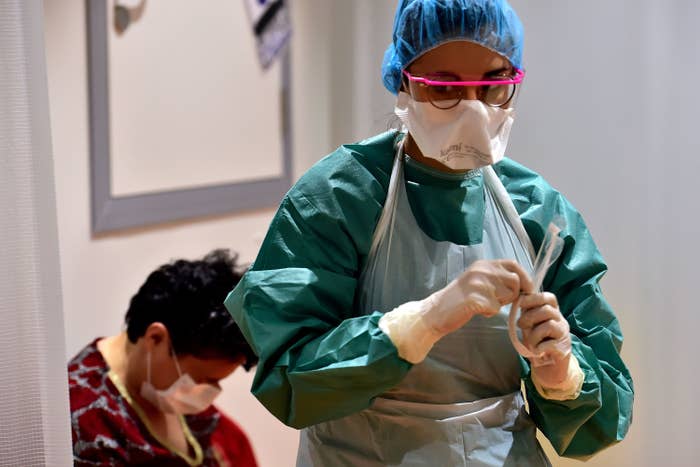
In 2018, a commonly used drug to treat irregular heartbeats was suddenly in short supply. “All of a sudden it gets taken away and I’m like, what is happening?” one New Hampshire cardiologist recalled to me recently. “I’m in the United States and I don’t have Cardizem right now?”
As the coronavirus sweeps across the globe, that experience is a preview of what’s to come: another round of what one trade publication called the “pharmaceutical version of The Hunger Games.”
China’s Hubei province is the epicenter of the global coronavirus outbreak. It’s also home to at least 12 drug plants supplying the US with everything from painkillers to antibiotics. And beyond Hubei, an estimated 80% of pharmaceutical ingredients are sourced from China and India (which, in turn, sources nearly 80% of its drug ingredients from China).
Our ability to make and distribute medicine here in the United States is falling apart, and it’s a direct result of the consolidation of the supply chains and factories that make it.
The Cardizem shortage of 2018 began when Hurricane Maria knocked out power to a handful of factories in Puerto Rico that produce saline bags used around the world for administering intravenous medications. Those few days of lost production in Puerto Rico caused Cardizem supplies to be backlogged for months. Pharmaceutical producers put most of their eggs in one basket, and the hurricane upset the basket.
The coronavirus could disturb a much bigger basket — the majority of pharmaceutical drugs globally.
Since at least 2005, hospital administrators and patients have experienced the fragility of the drug supply chain. Policymakers have failed to address the root cause. Why did we consolidate and thin out supply chains so aggressively?
The answer is found in the behavior of “power buyers,” corporations in the drug supply chain that buy a lot of product and subsequently have the power to set prices. Power buyers like CVS or the group purchasing organizations (GPOs), which hospitals use to buy everything from surgical gowns to generic drugs, have consolidated the drug supply chain, squeezing manufacturers to get rid of all their redundant sources of supply — or, even riskier, ship off their production to China.
Indeed, it’s consolidation all the way down: Many of these GPOs outsource even further, purchasing their generic drugs through separate power buyer entities. For example, Cardinal Health, the fifth-largest GPO in the country, runs a joint venture called Red Oak Sourcing with CVS Health, the largest pharmacy chain, to handle purchasing for Cardinal, CVS, Target, Omnicare (which sources for approximately 50% of all nursing homes), and OptumRx (the drug division of UnitedHealth Group). Other power buyers cover purchasing for Walmart, Walgreens, and Express Scripts. The market is so consolidated that just four of these power buyers control over 90% of generic drug purchasing for the entire country.
This consolidation might not seem like a bad thing. After all, generic drugs are cheap; a course of generic antibiotics may cost no more than $5 to the consumer. But power buyers have driven prices below a sustainable level for the producer. Their consolidated buying power — also called monopsony power — has lowered margins on generic drugs such that many manufacturers have consolidated to match their bargaining power or offshored their production lines to eke out whatever margin they can.
Drug shortages aren't the only consequence of this. Power buyers act similarly to the way Walmart handles purchasing for its more than 5,000 stores, demanding extremely low prices from suppliers and forcing them to either fold or move production to cheaper labor markets overseas. US factories close, production moves offshore, and the result is a loss of diversity and resiliency for the entire supply chain in return for slightly lower prices. Common goods, including garden hoses, TVs, air conditioner parts, and car parts are now all in shortage.
In the coming weeks and months, the coronavirus pandemic is likely to reveal the hidden risk embedded in the low consumer prices for medical supplies, just like the financial crisis forced hidden risks back on the balance sheet of major banks. Reports indicate the FDA is now carefully monitoring 150 drugs for anticipated shortages due to the outbreak.
As lawmakers and experts consider solutions to fix the fragile medical supply chain, many are focused on having the FDA gain visibility into our supply chain and relocating supply chains away from China. These approaches are a good start, but they also fail to address the root of the problem.
Rather than solely focusing on the country of origin of the supply chains, lawmakers and regulators should be focused on the market power issues that caused the problem. Regulatory solutions like breaking apart the power buyers of drugs and legislative solutions like banning contracts that guarantee massive purchasers the lowest possible price would allow the supply chain to rediversify. And diverse supply chains are better able to respond to a catastrophe.
We’re far beyond just manageable shortages. The coronavirus is forcing lawmakers to confront the weakness of US supply chains; the solutions should go beyond the short-term crisis and address the concentrated corporate power that’s at fault.
Olivia Webb is a policy analyst with the American Economic Liberties Project.
