The journalists at BuzzFeed News are proud to bring you trustworthy and relevant reporting about the coronavirus. To help keep this news free, become a member and sign up for our newsletter, Outbreak Today.
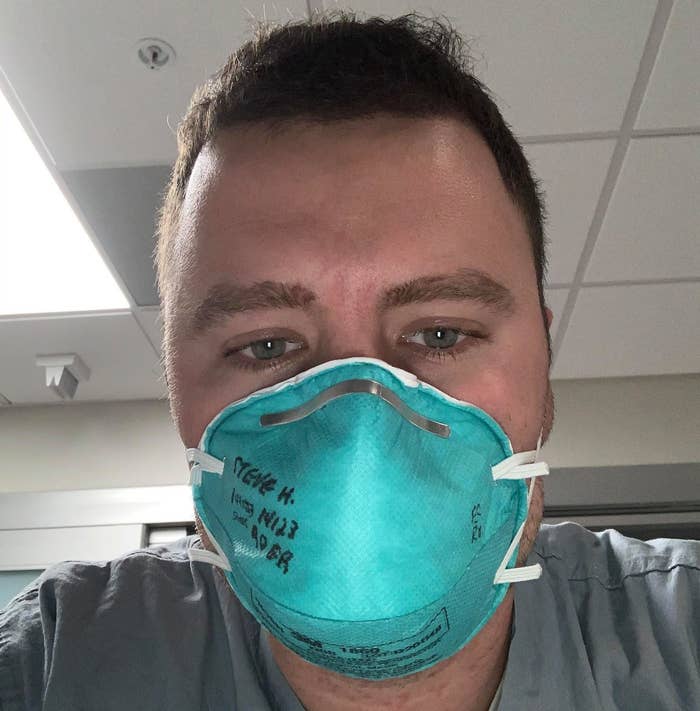
Two weeks ago, Steve Homick had “the worst night of work” he’s ever had in his four years of working as a nurse in Michigan.
Homick, a Canadian in his thirties, regularly crosses the border to work in one of the busiest emergency rooms in the US, at a hospital just outside Detroit. That night, he was assigned to work the hospital’s drive-through coronavirus testing site but things “got so bad” inside that he was pulled back in.
The ER had two rooms for patients with COVID-19, the disease caused by the new coronavirus, who needed ventilators. By the end of the night, the number of rooms had multiplied to 10, and they had been filled more than once. “I think our final intubation count for the night was 22 people, which is just absurd,” Homick said.
Before the coronavirus outbreak, the ER might have intubated a maximum of four people in one night if there were “several traumas,” he said. “None of these were traumas at all, it was all COVID-related.”
Homick, who works at Beaumont Hospital in Royal Oak, is one of thousands of Canadians who regularly crosses the border to work in Michigan’s sprawling health care sector. Now, like many other Canadians working in Detroit, he’s on the front lines of the area’s surging coronavirus outbreak. Experts have said Detroit could become the next hot spot in the crisis, following cities like New York, where the outbreak has been called “apocalyptic.”
Homick lives in Windsor, the small Canadian city just across the Detroit River, and others live in the surrounding area known as Essex County. Anywhere from 1,500 to 2,000 health care workers live in Windsor and commute to Detroit for work, according to the WindsorEssex Economic Development Corporation, a municipal non-profit.
Many of them work within the Henry Ford Health System, which runs six hospitals and employs 950 Canadian residents. More than 500 of them are nurses, the organization said. They’re able to work in the US thanks to the North American Free Trade Agreement, which created the TN visa for Canadians and Mexicans working in health care and other professions. Though Canada and the US recently banned non-essential travel between their borders, medical staff are considered essential and have been allowed to cross.
The fact that southeast Michigan’s health care sector depends on thousands of Canadians highlights the centuries-long economic and cultural relationship between Windsor and Detroit, which are less than three miles apart.
But now, as a global pandemic hits one side of the border harder than the other, the relationship is being tested. Windsor has seen a much smaller coronavirus outbreak so far, with only one death and 128 confirmed cases as of Thursday, while Michigan has 10,791 confirmed cases and 417 deaths, mostly in the Detroit area. One-third of Windsor’s cases are medical staff who work in Michigan, which has prompted some local leaders to call for restrictions on their travel.

Like their American colleagues, the Canadian health care employees are working to their limits. As they struggle to save lives, their own lives have never been at greater risk — and each day they drive to work, they make a decision to leave the relative safety of Windsor behind. BuzzFeed News spoke to a half-dozen Canadians from the region who work in Michigan’s health care sector, and several expressed fears about getting sick — one of them already has COVID-19 — and concerns about equipment shortages.
As he heads to work these days, Homick’s mind races. “The main thing that’s always in my head during this is, what can I do today to protect myself and not catch this?” He also wonders what has changed at the hospital since his last shift. Some of the COVID-19 floors are short on nurses because they’ve gotten sick, meaning he could get sent to cover for them. “I just think, what will today bring? I don’t want to have another night with 22 intubations.”
But for Homick and the other nurses, now is not the time to give up on their neighbors. Homick said supporting his colleagues is one of the reasons he keeps reporting to work.
“We’re all stressed out. We’re struggling right now; I know everyone is. You just don’t want to let them down,” he said. “We’ve got to put our heads together, chin up, we’ll get through this. It’ll be a while, but we’re going to get through this.”
Nurses like Homick often seek work in the Detroit area because there are more stable, full-time jobs. They’re also drawn to the US hospitals’ use of electronic health records, which makes their jobs easier — Windsor still uses paper.
“I have a passion for taking care of people, whether they’re people from Windsor or they’re people from the States.”
Such was the case for a nurse who lives in Canada and has worked at the Detroit Medical Center’s Harper University Hospital for several years. The nurse spoke on background as she did not have authorization from the hospital to speak to the media.
“I have a passion for taking care of people, whether they’re people from Windsor or they’re people from the States,” she said by phone this week. “It’s what I’ve wanted to do my entire life, so to help people — especially the ones that are as sick as they are — if we can help them from hopefully not passing during this time, it’s definitely something that I’ve always wanted to do.”
Now, when she prepares to cross the Detroit River to go to work, she’s afraid. “It’s definitely scary to think that the outbreak in Michigan or just in Detroit in general is — it’s huge,” she said. “Obviously all the hospitals are being extremely overwhelmed.”
She said her first day working with COVID-19 patients was “probably one of the worst experiences I’ve ever seen.” She realized how quickly the disease can affect patients’ health after several got intubated or sent to the Intensive Care Unit.
What made matters worse was a shortage of protective equipment for employees, she said — an issue hospitals across the country are facing. “It was a mess, because there’s never enough equipment in terms of N95 masks or even sometimes surgical masks are short, and the face shields, we have to share face shields,” she said.
She said there isn’t enough protective equipment for the doctors, either. “They always have to rely on us to give them stuff and there have been times where doctors have full-on yelled at us, because we didn’t have the equipment for them. But it’s not us that doesn’t have the equipment, it’s the whole hospital,” she said. “That gets really frustrating.”
Staff in her hospital are also having to reuse gowns, which she said raises the chances of contaminating patients who are being assessed for COVID-19 but might not actually have it. On top of that, the medical staff have taken on housekeeping’s role, since they can’t clean the floors anymore. “It’s just so much more additional work,” she said. “It’s hard for everybody.”
The Detroit Medical Center did not immediately reply to a request for comment.
Hospitals in the area have been working to expand their capacity and resources to respond to the growing outbreak. A spokesperson for the Henry Ford Health System said that like others in the area, it is “reaching capacity at several of [its] hospitals, including Henry Ford Hospital in Detroit.” The biggest part of the challenge is having enough employees to care for the surge of coronavirus patients, and Henry Ford is “working aggressively on a number of options to increase staff,” the spokesperson said. Those options include bringing in staff from other hospitals in Michigan that haven’t been hit as hard.
One of the people helping Henry Ford adapt to the crisis is Zain Ismail, a dual citizen who has lived in the Windsor area his whole life. Normally, Ismail works as a consultant to executives within the Henry Ford Health System and helps hospital leaders execute big projects, among other things. (Full disclosure: Ismail and this reporter are friends who have known each other for more than 15 years.)

That job has allowed him to make connections with people across the system and prepared his team for this moment. “At a time of crisis, a lot of us can jump in quickly and know who to call,” he said.
Most recently, he helped transform an outpatient clinic in Dearborn, Michigan, into a place for low-risk patients to free up more space for coronavirus patients in the main hospitals. He said he enjoyed the rush of having only a weekend to get it done. “I really like working quickly. I really like working with teams that can make decisions quickly and just move,” he said. “There’s no time to not take action.”
“During times of crisis, to add to this, people are just so willing to help,” he said. “So everyone is playing their role, playing their part, and moving towards executing on what we need to do, and that’s been fantastic.”
The seriousness of the situation is not lost on him, though. One day, as he was leaving, he found two housekeeping workers standing outside the new unit. “I just quickly perceived the fear of God all over them,” he said. As he spoke to them, they stared at him and asked, “are there patients in there?” Ismail reassured them that it was safe. “That was my first experience in realizing how this is affecting the clinical workforce around the world,” he said. “These people are petrified of catching this virus.”
Ismail, who previously worked at Leamington Hospital in Essex County, said he’s also been briefing a leader in Henry Ford’s human resources department on the fears spreading across Windsor and Essex County about health care workers bringing the virus home with them. He said health care systems in Michigan who rely on Canadian employees — not just Henry Ford — are worried about travel restrictions being applied to health care workers.
“This would be a — this might be hyperbole — but death sentence to Detroit and the surrounding region,” Ismail said. “We rely on Canadian nurses especially, heavily, heavily over here.”
Politicians in Windsor have recently raised the possibility of limiting health care workers’ trips across the border, while the local health unit has also said the government should restrict their travel. Suggestions have included making health care workers stay in Michigan throughout their workweek to reduce their chances of transmitting the virus in Canada.
“Probably the biggest thing that I think Windsor leaders are forgetting is that the city of Detroit, given its community profile, unfortunately will fare a lot worse than Windsor because of the structural inequities here, the abject poverty, the lack of public spending,” Ismail said.
He said any implications that Canadian medical staff are acting irresponsibly are wrong. “Health care workers are not your average citizen,” he said. “They know the risks, they know how to self-isolate, many of them are tested daily [for fevers].”
“People in Windsor need to know that these people are just going home, sleeping — in their garage some of them — they shower and then they come back to work,” he said. “So seeing them as a threat I think is an undue hardship in this time when they’re the ones that are really serving on the front lines.”
A young nurse who lives in Windsor and works at a Detroit hospital has been quarantined to her family’s basement since testing positive for the coronavirus. The nurse, who was tested at her hospital, also spoke on background because she did not have authorization to speak to the media. Luckily, her COVID-19 symptoms are relatively mild and she’s on the mend, she said.
Her parents leave her food on the stairs, and she puts on a surgical mask, grabs it, then returns to her room and shuts the door. “I don’t want them to get it, I’m so nervous,” she said. She keeps in touch with them by texting or calling every day.
“We have a lot of COVID patients,” she said of her hospital. “A lot. I’m going to say a majority of the patients in the hospital either have it or are being tested for it. It’s really bad there and [in] many of the Michigan hospitals, really.”
Her hospital has also experienced equipment shortages. Before the outbreak, she would use one N95 mask per patient. Now, she’s used one mask her entire shift, wearing surgical masks over it to help keep it clean.
“It’s scary,” she said. “It’s a totally different environment, we’re charting unknown waters. [...] We have no idea what it truly is. So that’s what stresses me out. Now look, I fricken’ got it!” she said with a laugh, followed by coughs.
For Nikki Hillis-Walters, a nurse in her thirties from Windsor who works in the ICU at Beaumont Hospital in Grosse Pointe — just outside Detroit’s city limits — the unknown is what sets this moment apart from any other in her more than 10-year career. “We have some good ideas about how to treat, but because everything is new, you do feel a little bit helpless,” she said. “You want to help people, but [you’re] not sure if the treatments are working or going to work.”

Hillis-Walters is in her thirties and has homes in both Windsor and Michigan, where her American husband and young son live. She also has a daughter in Windsor. She works full-time as a nurse in both places and runs her own yoga studio. Typically, she works in Windsor during the week, then three twelve-hour shifts at Beaumont on the weekends. But since the outbreak, she’s down to just the Michigan job to avoid infecting others, which has meant taking a significant pay cut. Her husband has also been laid off.
“There’s a big need for nurses where I am in Detroit and I knew that my job in Canada would be covered by somebody else easier,” she said. “There is some of that nurse-y camaraderie feeling, like I didn’t want to leave the girls in the trenches type of thing.” She said the hospital’s ICU is at least 90% full of patients confirmed to have the coronavirus.
The ICU has always been “a sadder place to work” than other areas of the hospital, she said, but it’s worse now because visitors aren’t allowed to visit their loved ones who are sick because of the risk of transmission. “That’s sad for us,” she said.
Homick, the other Beaumont nurse, feels similarly about families being banned from the hospital. They typically comfort patients and provide important information to staff about the individual, he said. The ban also means that once someone goes into the hospital, their loved ones might not ever see them again.
Homick, who also works occasionally at another hospital in Detroit too, said the age of some of the patients also worries him. “I think the biggest misconception about this from the beginning was we were told it only really affects the elder population or people with previous medical issues, and for the most part, that’s true. But I’m 30 years old and there’s people coming in that aren’t much older than me with no medical history, and they’re getting put on ventilators,” he said. “So that’s pretty difficult to see.”
Homick said he understands the concerns in Canada about his travel across the border. “I know for me, I get in my vehicle, I drive to work and when work’s done, I drive home and I don’t go anywhere else,” he said. His parents leave him supplies on his porch and he hasn’t seen his girlfriend in weeks. He said it’s been hard to change his lifestyle, but he knows it’s necessary.
The nurse from Harper University Hospital does the same. “I go to work and I come back home,” she said. “I don’t go anywhere else.” She said she uses online shopping to get groceries. “I feel bad for all the nurses, because we don’t just go over there just to work, we go over there to take care of patients,” she said. “It’s our passion to take care of patients.”
Hillis-Walters doesn’t go anywhere else, either. “I just go home, go to work, go to my husband’s home, go to work. I haven’t been getting groceries or going anywhere else,” she said.
Hillis-Walters worries about the border closing to her and other nurses, but what gets her through this all-around stressful time is focusing on the good that is happening around her. Beaumont is “working really hard” to get the medical staff the protective equipment they need and additional ventilators, she said, and the community in Michigan has rallied around frontline medical workers. Locals have sent letters thanking them for their work, while restaurants and the Wahlburgers food truck have brought them food, she said. Within the hospital, nurses who used to work in the ICU are returning to lend a hand.
“I always tell the girls at work: Do we want this to be the worst of times or do we want it to be like, ‘OK, we came through this and we came together, and we really showed up for people and the community supported us’? How do we want to write this story?”
She said she also wants the public to know that this virus is the “real deal.” She loves a good conspiracy theory as much as the next person, she said, but “people are definitely very, very sick from this.” Same goes for the need for more ventilators and protective equipment. “People are not lying to you,” she said. “That is the truth.”
The Harper University Hospital nurse has an even starker message to share. “What I want the public to know is that it is definitely so much worse than they think it is,” she said. “Every day we see younger and younger people coming into the hospital, and sometimes they’re OK and sometimes they’re really, really sick.
“We all want you guys to stay home, because no one can handle the spread, more and more people are going to die, and it’s just going to get worse.”