
Emily, a 32-year-old who lives in New England, had already been pushing for two hours when the OB-GYN came in and realized the baby was “sunny-side up” — in the occiput posterior position, meaning the baby’s body was facing Emily’s abdomen. It’s a more difficult birthing position because the baby’s head circumference measures larger from the back than the front. “Without giving me any warning, the doctor reached in and began turning my baby over in my body,” Emily, who declined to give her last name to protect her privacy, recalled in an email last week. “This was by far the most painful thing I’ve ever experienced in my life.” Emily said she looked over at her husband, who had tears running down his face as he watched. “I remember asking him a few days later if the doctor ever said anything to him or anyone in the room about making the decision to flip the baby,” she said. “He said no.”
Emily finally gave birth to a healthy baby girl about 36 hours after her water broke. Two hours later, her mother and sister rushed in to meet the baby. “They had been sitting for the whole day in the waiting room, watching other families come in and leave,” Emily remembered. “My mom and sister walked past the baby and came right over to me. I burst into tears at the sight of them and [said], ‘It was so hard,’ over and over. I felt ashamed that they weren’t having a Hallmark moment of joy with the new baby, but I needed them so badly. I couldn’t believe what I had just been through.”
Even now, when she gets texts from friends who are in labor, Emily spirals. “I stay anxious until I hear that it’s over, or sometimes with my closest friends, until I hear from them directly that they’re OK,” she admitted. “Sometimes even then I don’t believe them and it isn’t until I see them in person again that the anxiety fully leaves.”
Once she got home, it was hard for Emily not to feel resentment toward her baby. “I was breastfeeding,” she said. “I was getting up all night. I was sneaking in baths with Epsom salts in the evenings after the baby went to sleep, hoping desperately I wouldn’t wake the baby up and half not caring if I did. Fuck, we still had to take the dog out. Life continued to go on despite what I felt like I needed.” Emily, like so many other new parents, did not have the space to process or talk about the trauma she had experienced in the hospital. Friends thought she was a “chill parent,” but really she just felt like a zombie, “still in shock from everything that happened.”
Birth trauma, more acute than the “baby blues,” goes beyond hormonal fluctuations that arise from delivery and breastfeeding. It exists on a spectrum from full-blown post-traumatic stress disorder, which might look like flashbacks or hypervigilance, to symptoms that might not warrant a diagnosis but indicate difficulty coping after childbirth. It happens during hospital births and home births, with midwives and OB-GYNs, during medicated and unmedicated labors. Medical intervention can be traumatizing, but so can not having much-needed interventions when things go sideways.
The slippery nature of describing what happens in the delivery room makes it hard to identify and talk about afterward. “Trauma in and of itself relies on a person’s subjective experience of an event and to what extent they believe their life, bodily integrity, or psychological well-being was threatened,” writes Elyssa Barbash in Psychology Today. The stories of what can go wrong or how people can feel violated or scared for their own lives or their babies’ lives can make recounting birth stories a cloistered act, passed from mother to mother in private, the mundanity of early motherhood shrouding the commonplace danger and violence of delivering their children. But according to a 2018 study in the Journal of Perinatal Education, nearly half of the people who give birth experience trauma, caused by a range of experiences.
“But the doctor didn’t treat me like a person,” she said. “It was like a rape.”
Rachael Benjamin, director of Tribeca Maternity at Tribeca Therapy, said there are several reasons patients might experience birth trauma. “Birth trauma could be an emergency C-section, not feeling safe during labor or delivery, insufficient pain relief, the loss of a baby, or a long labor,” she said. “There could also be medical trauma.” This might look like what Emily experienced — the flipping of her baby without warning or consent — and can feel, to lots of birthing parents, like assault.
Ally, the owner of a bookstore in Alexandria, Virginia, felt violated during a prenatal appointment when a doctor inserted and opened a speculum for a routine check without warning Ally, and again after the delivery of her first child by the same doctor, when she experienced a retained placenta. The doctor reached inside to manually remove the placenta without explaining what was happening or why it was necessary. Ally described the experience as “being human-puppeted.”
“The nature of a retained placenta,” Ally, 37, said, means that to remove it, “someone is entering your body” — in Ally’s case, without her consent. “But the doctor didn’t treat me like a person,” she said. “It was like a rape.” Ally entered a five-week program at her local motherhood center to treat her postpartum depression and trauma, something she points out she had to pay for out of pocket, which excludes working-class mothers from being able to seek similar treatment.
Several of the women interviewed for this article mentioned their desire to be “good patients,” who accommodated the medical teams around them. “I’m too nice to everyone,” said Brittanny Travers, a 34-year-old stay-at-home mother in California who ended up with an unplanned C-section after an exhausting labor. “But now I wish I could’ve been like hell no! This is going to go this way. It’s my life, it’s my body. That doctor is working for me.”
These traumatic outcomes are far worse for Black people, who are at a higher risk of harm in hospitals. “Black maternal health care is in complete crisis,” Noelene Jeffers, head of the National Association to Advance Black Birth told me. “We know that most of the maternity care providers are white, and there’s just not enough Black midwives and Black OB-GYNs to provide racially and culturally congruent care. I think that that's part of the trauma that people are experiencing. They're not able to make autonomous decisions and are being treated poorly when they ask questions and demand that their rights are upheld.”
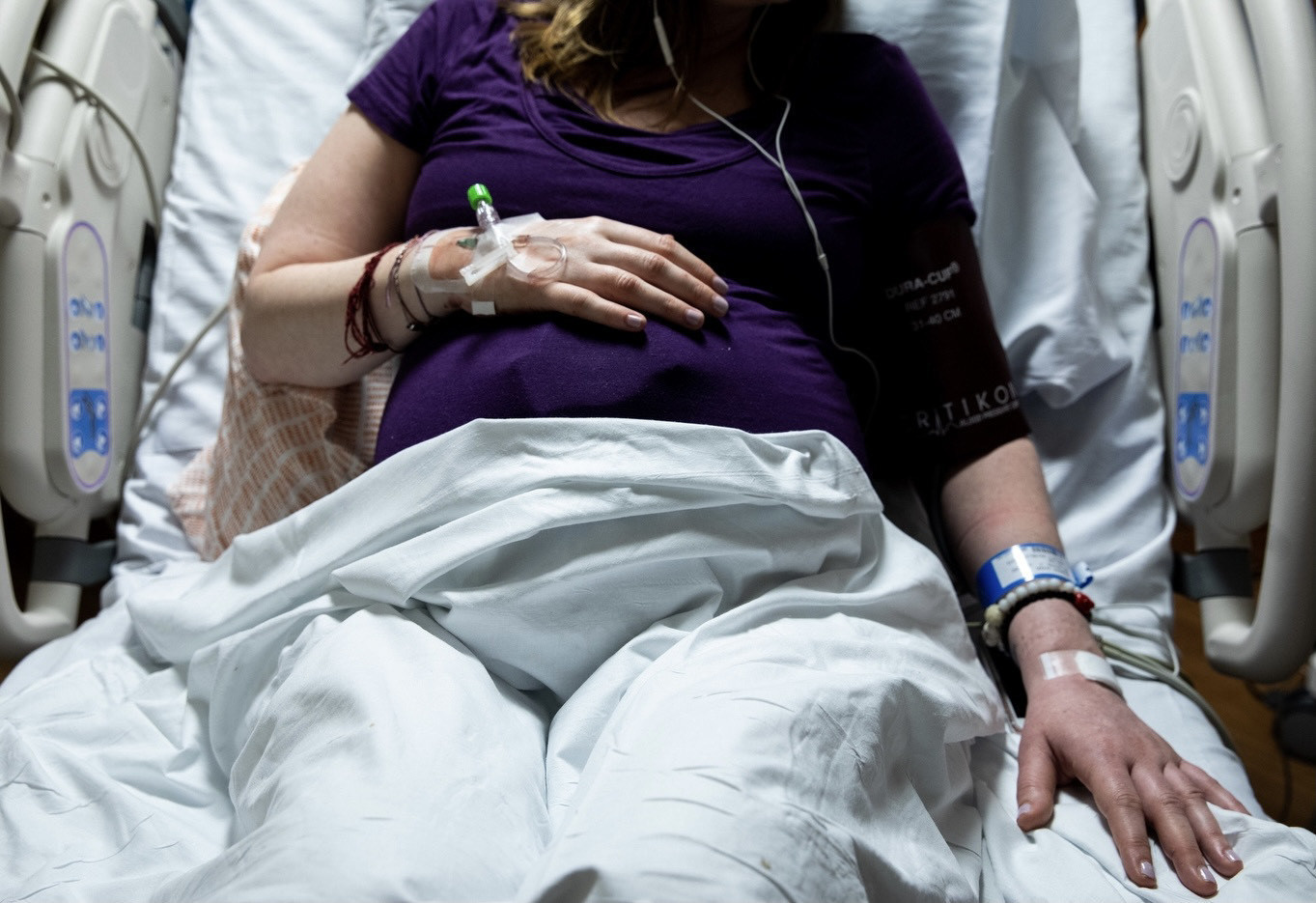
After her baby experienced a health emergency shortly after birth, it took Liba, a stay-at-home mom in Washington DC, six months to be able to talk about her experience without crying. “It’s fair to say that the unifying feeling for me is anger,” Liba wrote in an email. When her midwife checked her shortly before she delivered, Liba said, “they noted that they could not feel the baby’s skull sutures but did not suggest that might mean he was unfavorably positioned. A moment later, his entire body fell onto the bed below me in a single push, with the midwife sitting in a chair 10 feet away, totally unprepared. I’m angry that they refused to see what was right in front of them: a malpositioned baby.”
“I remember thinking he was so small, and then being terrified by the shape of his head, which looked like an anvil,” she wrote in an email. As Liba sang to her newborn, she could see “that he was not okay — he was spitting out large globs of mucus or fluid and his cry had a rattle to it.” They quickly cut the umbilical cord and rushed the baby to the other side of the room while Liba delivered her placenta and was sutured up. “I just wanted to know what was happening to my baby,” she said. “He needed mechanical suction and two sessions with a CPAP machine to finally get him breathing reliably.”
Her baby’s head was misshapen because of his brow presentation, but 12 hours later, its shape was round. “My son is six months old and I still ask the pediatrician to feel his skull sutures at every visit,” Liba added.
For Emily, the mom whose baby was “sunny-side up,” plans to grow her family have changed since the doctor tried to flip her baby without warning. “I have not yet decided if I want another baby,” she said. “I always thought I wanted two kids. I don’t think it’s a stretch to say it’s almost entirely due to the trauma I experienced with my first birth that now I can’t decide.” After Emily’s delivery she also had preeclampsia, a condition she’s at high risk of developing with a subsequent pregnancy, which adds another layer of fear. “Having a sister is one of the great joys in my life,” she added. “I have huge feelings about denying my baby that joy. I have huge feelings about giving birth again. I can’t tell you which side is winning right now.”
“I always thought I wanted two kids. I don’t think it’s a stretch to say it’s almost entirely due to the trauma I experienced with my first birth that now I can’t decide.”
Elizabeth, 38, an academic in the Midwest, hemorrhaged after giving birth to her first child six years ago and has been diagnosed with PTSD, which manifests when she feels like she’s not in control of her body. “When I’m a passenger in a car and someone takes a different route than I expected,” she said, “I remember how it felt for my life to be in danger.” She panicked recently when her husband braked without warning while they were driving. And she panicked when her children, feeling cooped up from quarantine, were playing rambunctiously on top of her. “I might have yelled, but I don’t remember,” she said. “Part of my post-traumatic stress is temporary amnesia.” She does remember a sense of fear, though. “I was like, whoa. That is a post-traumatic moment. It reminded me of the feeling of things happening to my body.”
The hemorrhage Elizabeth experienced after her first birth shaped the way she approached her second birth. “When the OB said she wanted it to be an atraumatic birth, I thought that word was significant. It wasn’t just not traumatic, it was actively part of the healing process for me to know that it was possible to have a birth that was pleasant.” Part of what made Elizabeth’s second birth so empowering was the way the OB informed Elizabeth of everything happening to her body, and the kinds of choices she could make. “Even with all the medical interventions, I felt very in control,” Elizabeth said. “I didn’t have any pain medication, but I sang, my husband and I sang duets. [The OB] talked me through the sutures, showed me the amount of blood I lost.” The OB also let Elizabeth lie on her side, an easier position to birth in, and let her hold own leg, which gave her “a sense of control too.”
Gretchen, a librarian in Phoenix, labored without anesthesia while delivering her second child until she was 8 centimeters dilated. At that point, she said, “I asked for the epidural three times, but my partner and my midwife [thought] I could push through. It’s upsetting when you’re so out of control of your body, and you say you’re done, and people ignore you and override your choice.” Her baby was in distress, and ended up being born via C-section. As Gretchen was being wheeled into the operating room, she heard the midwife say it would “affect their statistics” to have a C-section. “To have that be said on my way to meet my child... It’s not my job to not let the medical professionals down.”
“The current halo around natural childbirth is a dangerous overcorrection and doctors and hospitals are not doing enough to keep women psychologically safe and whole,” Lauren, a writer in Portland, Maine, said of her experience hemorrhaging during birth and receiving a blood transfusion. “Both are a problem. The only answer as I see it is greater research, regulation, and oversight of this whole process as a part of a public health campaign. It can't be on women alone to educate each other about our terrible experiences and then just play birth roulette with our choices.”
Hayley Oakes, a licensed midwife based in Los Angeles who does home births, believes most births are not medical emergencies, although they’re treated like one. But “it’s an inherent risk, choosing an out-of-hospital birth,” she said. “You might need more support and intervention than you can have at home.”
“Hospital births are a preference for a lot of people in this country, but that doesn’t mean those people can’t get a more holistic approach in their healthcare,” she added. The problem is, medical practitioners and natural birth advocates have radically different approaches to childbirth. “It’s always up to the doctors what they think is appropriate. It makes for a really hard relationship [between midwives and OBs], so midwives don’t always feel supported by physicians, and physicians end up feeling like the midwives’ practice is too risky.”
Oakes’ backup hospital — where she takes her patients on the rare occasion they do need to transfer to a hospital during labor — is Dignity Health California Hospital in downtown Los Angeles. “Labor and delivery is basically run by nurse midwives, and there are always doctors on the floor in case they’re needed. I’ve seen those midwives care for people in ways I’ve never seen anywhere else. They really push for a safe, vaginal birth that leaves you with your baby, trying to limit as many interventions as possible.” Collapsing the divide between medical and natural births seems to limit the trauma Oakes has witnessed when hospital births don’t go according to plan.
Giving new parents support while they heal and reflect on the life-rending experience of birth means a more robust network of care than we currently have in place under our standard medical model. After the baby arrives, most mothers get a 6-week checkup with their OB-GYNs. The doctor is looking for very specific things, according to Christine Pieton, who has a pelvic health practice in Santa Barbara, California. They might say, “From a vitals standpoint, you're stable,” Pieton said. “We've taken your blood pressure, your stitches — whether C-section or vaginal — aren’t infected, and there are no major red flags in terms of mental health popping up in your 10-minute postpartum appointment. We're going to clear you for exercise, and we're going to clear you for sex.” But how to ease back into life while getting used to a new body with different shapes, limitations, and scars most often falls to the mother, who may not know about or be able to afford pelvic floor physical therapy and mental health counseling.
Last year, the National Association to Advance Black Birth created the Black Birthing Bill of Rights, which can serve “as guidance for government programs, hospitals, maternity providers and others as they transform their policies, procedures, and practices to meet the needs of Black birthing people,” according to their website. These rights include being believed, respected, and having your humanity recognized, as well as not allowing obstetric violence to go unchecked, getting to decide how to nourish your baby, and being informed of all pain relief options.
Imagining birth without trauma, might look like “understanding that bodily autonomy and human rights in the birth world is necessary in order to send any pregnant person” into a delivery room.
Preventing birth trauma is the ultimate goal. Chanel Porchia-Albert is the founder and CEO of Ancient Song, a doula-certifying organization in Brooklyn whose goal is providing Black people and low-income families with doula support. Imagining birth without trauma, according to Porchia-Albert, might look like “understanding that bodily autonomy and human rights in the birth world is necessary in order to send any pregnant person” into a delivery room.
For a traumatic delivery, Porchia-Albert underscores the importance of “having accountability mechanisms in place” that allow this person to “speak their grievance and have it addressed. They should be heard by an independent body, she says, “completely separate from institutions, that does not put the hospital administration in charge” of reprisal and reconciliation, she added. She also makes sure her doulas notify patients on how to access resources to recoup costs associated with medical bills for unnecessary interventions, as well as pay for necessary therapies.
Addressing the needs of those most likely to experience trauma during birth means creating broad structural change to make everyone safer during the most vulnerable moments of their lives. Restorative justice work and education about rights before, during, and after the baby arrives can change how giving birth can look in a country that centers the health, dignity, and autonomy of the birthing parent as well as the baby.
“At first, I worried that I would always connect one of the best things that ever happened to me — my daughter coming into the world — with one of the worst things that ever happened to me,” Hannah, a Seattle-based writer, wrote in an email. But three and a half years after Hannah’s trauma, she said she can reflect on the support she received, friends and family “bringing sandwiches and suggesting high-iron foods to eat, just listening or sitting” with her if that was what she needed.”
“I had to rebuild myself somewhat in order to reemerge into the world,” she added. “When I hold [my daughter], I know that she’s here because she is strong, and I’m here because I am strong.” ●
Correction: Hayley Oakes only delivers babies at home. An earlier version of this story said she also delivered in hospitals.
Ellen O’Connell Whittet is the author of What You Become in Flight, a memoir about ballet and injury, and teaches at UC Santa Barbara.
