BuzzFeed News has reporters around the world bringing you trustworthy stories about the impact of the coronavirus. To help keep this news free, become a member.
Tanya Johnson wishes she never went to the cookout.
On Juneteenth, Johnson and a dozen or so friends gathered in a backyard in Atlanta, eating BBQ and sitting in chairs spaced out in a circle. Johnson, 27, accepted a ride to and from the party with her friend Jessica McCauley, 31. They drove with the windows rolled up and hugged each other goodbye.
Three days later, Johnson got a sore throat, then an earache, then a fever. The next day, McCauley’s 31-year-old boyfriend, Remey Williams, also came down with a fever. On June 24, a friend who had been at the BBQ called McCauley to let her know their brother-in-law had since tested positive for the coronavirus. He had attended the cookout and McCauley and Williams had interacted with him inside when they weren’t wearing masks.
The friends made plans to get tested. They went to a parking lot in Fulton County where nasal swabs were performed inside their cars at a state-run testing facility.
And then they waited.
And waited.
And waited.
It would be 16 days before McCauley was officially emailed results telling her she had tested positive for COVID-19.
Johnson’s mother, 59-year-old hospital secretary Margaret McNair, had accompanied her daughter to get tested too. While Johnson eventually tested positive and had to be hospitalized, McNair had to wait 19 days before an official email arrived in her inbox telling her she was negative. That’s five days longer than the quarantine period of two weeks recommended by the CDC.
“Every day I was checking and checking and checking. It kept saying no results,” McNair told BuzzFeed News. “I emailed. No results. I kept saying, ‘I’m a healthcare worker. I need the results. I have to go back to work.’”
“If they want to slow down the spread of this,” said McCauley, “I think they need to be a little more aware of what’s going on.”
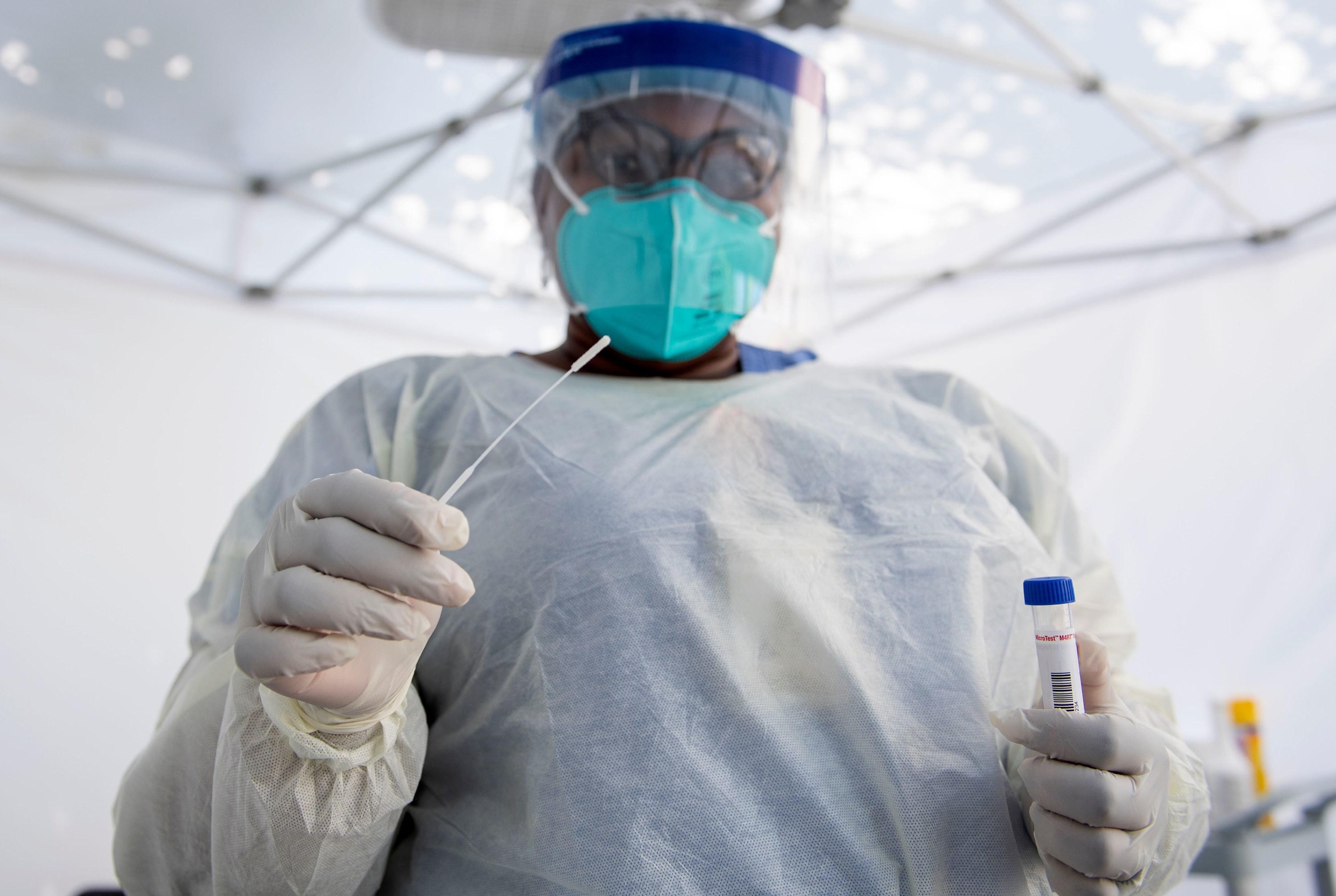
The backlog in testing across large parts of the US comes as both demand and infections soar. The country officially marked 4 million confirmed cases of the virus on Thursday, but experts caution there are many more that have gone undiagnosed.
President Donald Trump has held up the US as world leaders in testing, telling reporters at the White House on Thursday the country had now performed more than 51 million coronavirus tests. But with millions more Americans seeking tests — whether because they have fallen ill, have been exposed to an infected person, are trying to return to work, or are even looking for peace of mind before they take a vacation — private laboratories and health agencies are swamped, leading to communication and technical breakdowns, as well as extensive delays.
As health experts and officials note, the extended wait times for some results — exacerbated by a shortage of supplies — are also undermining the very purpose of testing.
“The average test delay is too long,” National Institutes of Health Director Francis Collins told NBC’s Meet the Press in an interview that aired Sunday. “That really undercuts the value of the testing, because you do the testing to find out who’s carrying the virus, and then quickly get them isolated so they don’t spread it around. And it’s very hard to make that work when there’s a long delay built in.”
Angela Rasmussen, a virologist and research scientist at the Center for Infection and Immunity at the Columbia University School of Public Health, told BuzzFeed News that stories of people waiting 17 days or more were evidence that “nearly eight months into the pandemic, our testing capacity is still woefully inadequate.”
“In the big picture, huge testing backlogs bode very poorly for the future, as robust capacity for rapid, easily accessible testing is essential to our ability to safely reopen the economy,” she said in an email. “Even 5 days is too long, much less 17 (17!!!!!!!!!!).”
Kevin McCauley, a 36-year-old graphic designer in Houston (not related to Jessica McCauley in Atlanta), was forced to wait 17 days for his results after he sought a test on June 26. Days earlier, he had driven his sister-in-law to a hospital in the middle of the night after she began experiencing COVID-19 symptoms. When she was officially diagnosed with the virus, a doctor told him to self-isolate and assume he had the virus, but he wanted to know for certain.

After waiting for more than two hours at a drive-thru testing site run by Harris County, he was given paperwork telling him to contact health officials if he didn’t get an email within five days. When that never arrived, he called the only number he could find: a health department line that would not accept incoming calls and has an automated message telling people to expect their results in three to five days. He made an online account with Quest Diagnostics, the private lab performing his test, but there was still nothing.
“I was checking every few days,” he told BuzzFeed News.
While he took quarantine seriously at first, his standards gradually slipped as he continued to wait amid silence but without any symptoms.
“For the first probably eight or nine days after taking the test, I was really strict about self-isolating,” he said. “Anything I needed I ordered online. I didn’t leave the house. I didn’t go anywhere. I had a friend pick me up a bottle of whiskey.
“And then at a certain point, I was like, This is unrealistic. I need to leave. I don’t have any symptoms.”
He finally received a call on July 13 from a county health representative informing him his test result was negative.
“I said, ‘Why did this take 17 days?’ He said, ‘Oh, well, you’re in Houston. It’s really swamped. They can’t handle it,’” Kevin recalled. “He was very sympathetic. He talked to me for a long time about the failures in the system. He was really frustrated.”
Kevin’s test result, which he provided to BuzzFeed News, showed it wasn’t received at Quest’s Dallas lab until July 2, six days after his nasal swab. It was officially reported into the Quest system on July 17.
A spokesperson for Quest told BuzzFeed News in a statement that they and others in the industry were struggling to keep up with the demand. The company said the average turnaround time for nonpriority patients is seven days, but noted “a small subset” were waiting up to two weeks for results.
“Demand for COVID-19 molecular testing continues to outpace Quest’s capacity and is highest in the South, Southwest and West regions of the country,” the Quest spokesperson said. “However, the inflow of specimens to our labs has stabilized, at a high level, compared to last week, due to our efforts to modulate orders for lower risk patients.”
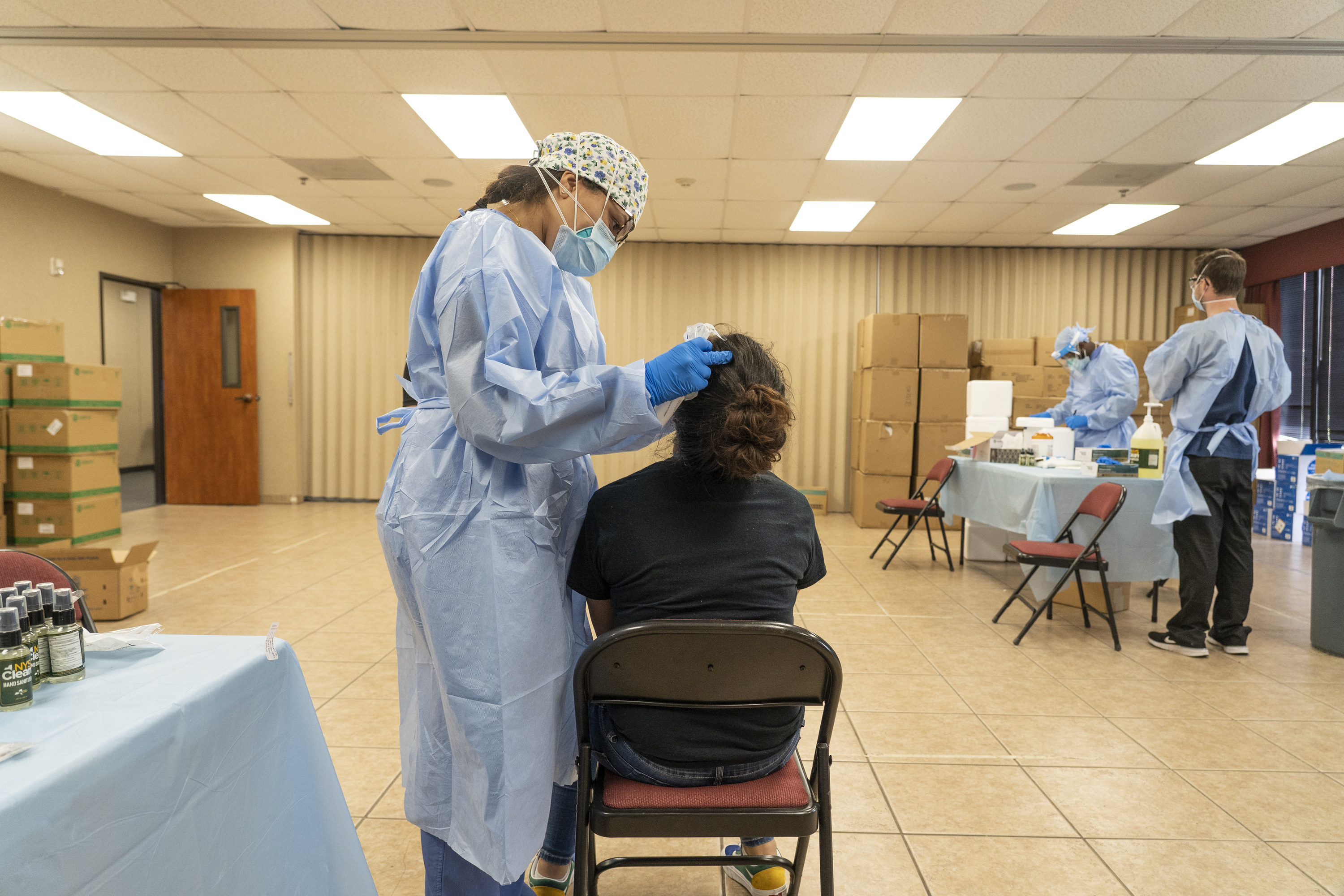
Dr. Umair Shah, executive director of the Harris County Public Health Department, told BuzzFeed News that Kevin’s experience was disheartening, but not surprising.
“Let’s not mince any words,” he said. “That’s awful. This is the problem with this entire system around the country relating to testing and lab turnaround: We don’t have a system.”
According to Shah, it is currently taking two weeks on average for results to be received from people who visit federally funded testing sites in Harris County, where some results are still being delivered to the health department via an outdated fax machine. The ideal turnaround is two to three days. Such delays only hamper public health workers trying to work against the clock to stop the spread of the virus. Shah worries, in particular, that asymptomatic patients who do not receive results in a timely manner may incorrectly assume it is because they are not infected.
“It’s nonsensical that in 2020 we, as Americans, do not have a public health system that coordinates with healthcare providers and lab reporting that is markedly better than what we have. This is because of this underinvestment in public health over the decades,” he said. “Well, the chickens are coming home to roost.”
Louise Serio, a spokesperson for the American Clinical Laboratory Association, a trade group representing Quest and LabCorp (which performed the tests in Atlanta on McNair, Johnson, and McCauley after their cookout), told BuzzFeed News that their members had quadrupled their testing capacity since April, but were struggling to keep up with demand, as well as a supply shortage of reagents, pipette tips, test kits, and platforms that allow for high-volume testing.
“We are building capacity every single week, but we have seen in the past several weeks that demand has skyrocketed,” she said. “We’ve made a lot of progress, but we don’t have control over demand. Labs don’t order tests.”
Asked whether her members were prepared for the need for testing to further increase if schools return in the fall, as Trump has pushed for, Serio responded, “Right now, when you think about the supplies that are in high demand, we expect that high demand to continue.”

Even after labs turn around results, technical or communication breakdowns are preventing people from learning of their diagnosis. The LabCorp results page for Jessica McCauley, the Atlanta woman who drove her friend to and from the ill-fated cookout, said her June 26 sample was received on June 27 and reported nine days later on July 6. She had created a LabCorp account, but the results never showed up online.
“I started to check. It wasn’t there. So then I was checking periodically and it just wasn’t coming up. It wasn’t showing up,” said McCauley, who works as a flight attendant. “I sent an email. I was calling. There were no responses.”
McCauley’s email from Fulton County’s public health department announcing her positive result wasn’t sent until July 12. Two days earlier, by chance, a health worker had called her boyfriend with whom she’d been quarantining to discuss the positive result he had received on July 7, when he inquired if the staffer could check for McCauley’s results. It was then that she first heard she, too, was infected.
“I’m blessed that my symptoms weren’t as bad as some people who have passed away from it, but the fact that people are waiting this long is not OK,” McCauley said, “because if I didn’t have it I would’ve just been sitting around, but if I did have it and was asymptomatic I’d just be passing it along to people.”

McNair, the Atlanta hospital secretary, first cared for her increasingly sick daughter at home, but then worried for her as she spent a week in hospital receiving treatment. She also feared for her 98-year-old father, who lives with the family.
For 19 days, McNair also couldn’t work until she knew for sure she was not infected and would not be a risk to her hospital colleagues. “It was driving me nuts,” she said. “It was really scary.”
“I’m annoyed at the system because I think they should get back to people in time,” McNair added. “It’s like a domino effect. I lost my money not working all those days. Had my results come back in a timely fashion, I could have gone back to work.”
Test results in Georgia have been taking 7 to 10 days on average, but even longer from some commercial labs like Quest and LabCorp, according to state health department spokesperson Nancy Nydam. “As you are aware, it is a nationwide problem,” she said, “not specific to Georgia.”
In a statement to BuzzFeed News, a LabCorp spokesperson said the company had experienced “additional delays” for some individuals who had been tested in Fulton County and had tried to use the company’s website to access their results. “Many of the test orders were not delivered to LabCorp electronically requiring additional manual steps, which contributed to the time to make results available,” the spokesperson said.
Sheena Haynes, a spokesperson for the Fulton County Board of Health, said the local system is struggling to keep up with demand.
“In the last several weeks, there has been an increase in the number of people getting tested, resulting in the labs being overwhelmed and results being delayed,” she said. “Our district health director and chief medical officer have worked with LabCorp to resolve the issue, and results are coming back sooner for testing being done now.”
McNair’s daughter, Johnson, is now out of the hospital and on the mend, but still has a lingering cough.
McNair, though, is still struggling to believe she had to wait 19 days for an answer.
“Guess what’s so funny? The day after I got my results, someone called from somewhere and they wanted to do a follow-up,” she said. “The lady was like, ‘Oh, actually, too much time has passed to do a follow-up.’”
