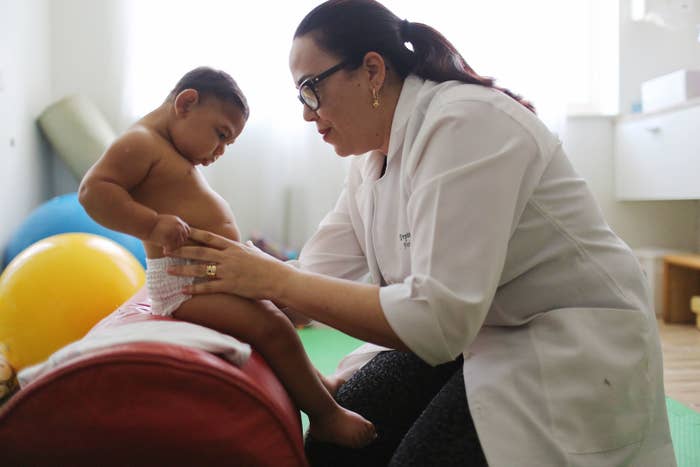
A simple mutation in one gene may have triggered the 2016 epidemic of infant brain damage tied to the once-innocuous Zika virus, Chinese researchers suggested on Thursday, based on a genetic comparison of old and new disease strains.
But outside experts expressed caution about the claim, reported in the journal Science, because it relies on just one ancestral strain of the virus to come to its conclusion.
Since an outbreak of the Zika virus began in Brazil in 2015, the tropical disease has spread to more than 40 nations, largely in the Americas, and also Puerto Rico.
Until that outbreak, the disease was regarded as a mild mosquito-borne virus marked by a purple rash, a less severe cousin to dengue and other tropical illnesses spreading worldwide in our era of cargo transport and jet travel. How the virus, spread by mosquito bites and sex, suddenly began causing severe brain damage — the abnormally small head size known as microcephaly — in thousands of newborns has puzzled public health experts throughout the epidemic.
“The most surprising result is only one mutation would have such a dramatic [effect],” study investigator Zhiheng Xu of the Chinese Academy of Science told BuzzFeed News by email. “We have expected that several more mutations are needed to have that kind of effect.”
In the study, the team compared a strain of the virus isolated from Cambodia in 2010 to three strains from the 2015 outbreak, finding that the earlier strain caused less damage to brain cells in baby mice and human cells. While the outbreak strains killed entire mouse litters and caused microcephaly, for example, the older strain only killed about 17% of them, and caused less severe and less frequent microcephaly.
To figure out why, the Chinese researchers generated seven different strains of the older virus type, each one adjusted to have just one genetic mutation seen in the more recent strains. The artificial strain carrying a single alteration to a gene called S139 (first noted by other researchers last year), which affects the coating of the virus, triggered the mortality and brain cell death seen in the outbreak strains. What’s more, when the researchers reversed the mutation in an outbreak strain isolated from Venezuela in 2016, it reduced the damage in mice and in human cells.
“This is very nice work to swap in and out viral [genetic] changes to see what happens,” infectious disease expert David O’Connor of the University of Wisconsin told BuzzFeed News.
“Having said that, we are still a long way from knowing the answer to the ‘Why Brazil, why now?’ question," he said.
That’s partly because the researchers have only shown the microcephaly effect in mice, not other lab animals more genetically similar to people. And they injected the virus into the mice, which doesn’t capture the whole route of transmission of the disease. Other scientists will also want to test more ancestral viruses than the 2010 Cambodian one.
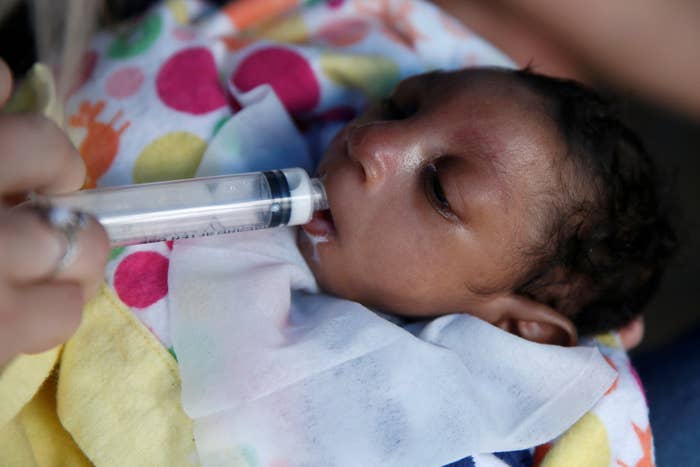
Viruses pick up genetic mutations all the time, but few have outsized effects. Statistically, the mutation in the more recent Zika virus strains appears most likely to have arisen in May 2013, the study concluded. That happened just ahead of a Zika virus outbreak in French Polynesia marked by increased cases of the paralytic Guillain-Barre syndrome, a rare side effect linked to infection with the virus in adults.
Some evidence suggests the S139 mutation makes Zika virus more infectious, which might help explain why the mutation survived in its viral genome. Although this year the number of confirmed Zika infections has steeply declined in most places, the disease is still causing infant birth defects in 27 countries, according to the Pan American Health Organization. Infections are linked to nearly 3,700 microcephaly cases worldwide, including 98 cases in the US.