
An Omicron-fueled coronavirus surge in places like New York and Miami have cities across the US scrambling to avoid similar fates as the federal government ramps up its own testing infrastructure. Experts, though, warn it could already be too late.
The Omicron variant now makes up an estimated 73% COVID-19 cases as of last Friday, according to data from the CDC released on Monday. That’s up from 12.6% the week before and just 0.7% two weeks ago.
Federal COVID-19 case data collected by University of South Florida epidemiologist Jason Salemi show the sharpest percentage increases in weekly cases were in Florida and Hawaii, two states that saw early Omicron outbreaks; Omicron caused 80% of the cases in Miami last week. Both the mayor-elect of Pittsburgh and the mayor-elect of Atlanta reported they tested positive for COVID-19 on Monday.
“This spreads so fast that if you look at what's going on today, it's actually already happened 10 to 14 days ago,” said epidemiologist Salim Abdool Karim of the Centre for the AIDS Program of Research in South Africa, who spoke at a Harvard Medical School briefing on Monday. “Time is not on your side.”
With the world already grappling with the delta variant, scientists are racing to understand how the rapid spread of Omicron could affect the global health crisis that the pandemic sparked in March.

The CDC is calling for people to get vaccinated or boosted, wear masks indoors, and test themselves before attending holiday gatherings. But the increased demand is posing challenges.
In New York City, where Omicron already accounts for 92% of cases and case numbers are breaking records every day, residents wait in line for hours and scour pharmacies for rapid tests. Denver and Miami also saw long lines for tests on Monday, and Daviess County in Indiana ran out of tests this weekend.
Other parts of the country are trying to avoid this disaster. Cities such as Baltimore and Washington, DC, are giving away free tests in libraries. Seattle has opened a testing site at City Hall, and Santa Clara County, California, nearly doubled appointments at its largest testing facility this week, to 3,500 a day, and anticipates going as high as 5,000 a day.
“A very common question I’ve been hearing is about family gatherings, especially in the weeks ahead,” said viral variants program coleader Jeremy Luban of the Massachusetts Consortium on Pathogen Readiness. Luban said testing is one of the most important ways to keep these gatherings safe, after vaccination. That makes testing centers and affordable at-home tests essential this holiday season.
President Joe Biden on Tuesday laid out a plan to contend with the highly contagious new variant, including opening federally run testing sites in New York City this week.
“I know you’re tired, and I know you’re frustrated," Biden said in his speech. "We all want this to be over. But we’re still in it. This is a critical moment."
The new push will include moves to make testing more accessible to Americans, providing supplies and military medical personnel to hospitals, and setting up federal vaccination clinics, senior administration officials told reporters on a call on Monday evening.

The federal government has 500 million at-home rapid tests, which people will be able to access for free via a website — but not until January, administration officials said. Those are in addition to 50 million tests the administration announced earlier this month as part of its winter COVID-19 plan, before the widespread emergence of the Omicron variant.
New federal testing sites will be opened in the coming weeks “based on where states and communities have pressing constraints and where the state and local public health officials request our assistance,” a senior administration official told reporters on Monday.
The White House’s approach is based on the expectation that hospitalizations of unvaccinated Americans will increase in the coming weeks, and that COVID-19 cases across the board will rise.
At the local level, public health officials are adding staff to testing centers and planning to open shuttered or new sites ahead of the wave. “Our work on Omicron is really kind of doubling down on the things we know work,” said Chris Hoff of the DuPage County Health Department in Illinois, speaking on a National Association of County and City Health Officials podcast. ICU capacity is already down to 20% in the county of 1 million people in the western suburbs of Chicago.

In Vernon, Connecticut, COVID-19 testing resumed in November, with steadily increasing demand since then, city communications specialist Dave Owens said. The city has also started giving booster shots, 446 last week, after pharmacies couldn’t keep up with demand.
Michael Purcaro, the town administrator and emergency management director, told BuzzFeed News that Vernon has seen a 200% increase in demand for testing within the past few days. Normally, one of the city’s testing centers sees about 50 to 60 cars in an afternoon, but a few days ago, it saw 375.
“The surge is here, and we expect it to continue for at least the next few weeks,” Purcaro said. “At least that’s what we’re planning for from an operational standpoint both in testing and vaccination efforts.”
Mike Estramonte of StarMed Healthcare in Charlotte, North Carolina, told BuzzFeed News that since June, his organization has planned to open dozens of winter testing sites able to see 800 to 900 people every hour and return results within two days. “It wasn’t until really the last three or four days that we’ve been staffed up to handle what we’re experiencing now and most people are getting in and out of our lines in less than an hour,” he said.
The test centers will be open on Christmas, Estramonte said, adding, “COVID doesn’t take a vacation.”
Nationwide demand for tests has steadily increased since early November, according to the US COVID-19 Trends and Impact Survey. “We also see more people reporting that they have COVID-like symptoms or that they know someone who does — those numbers are now about as high as they were during late August and September,” Carnegie Mellon University statistician Alex Reinhart said.
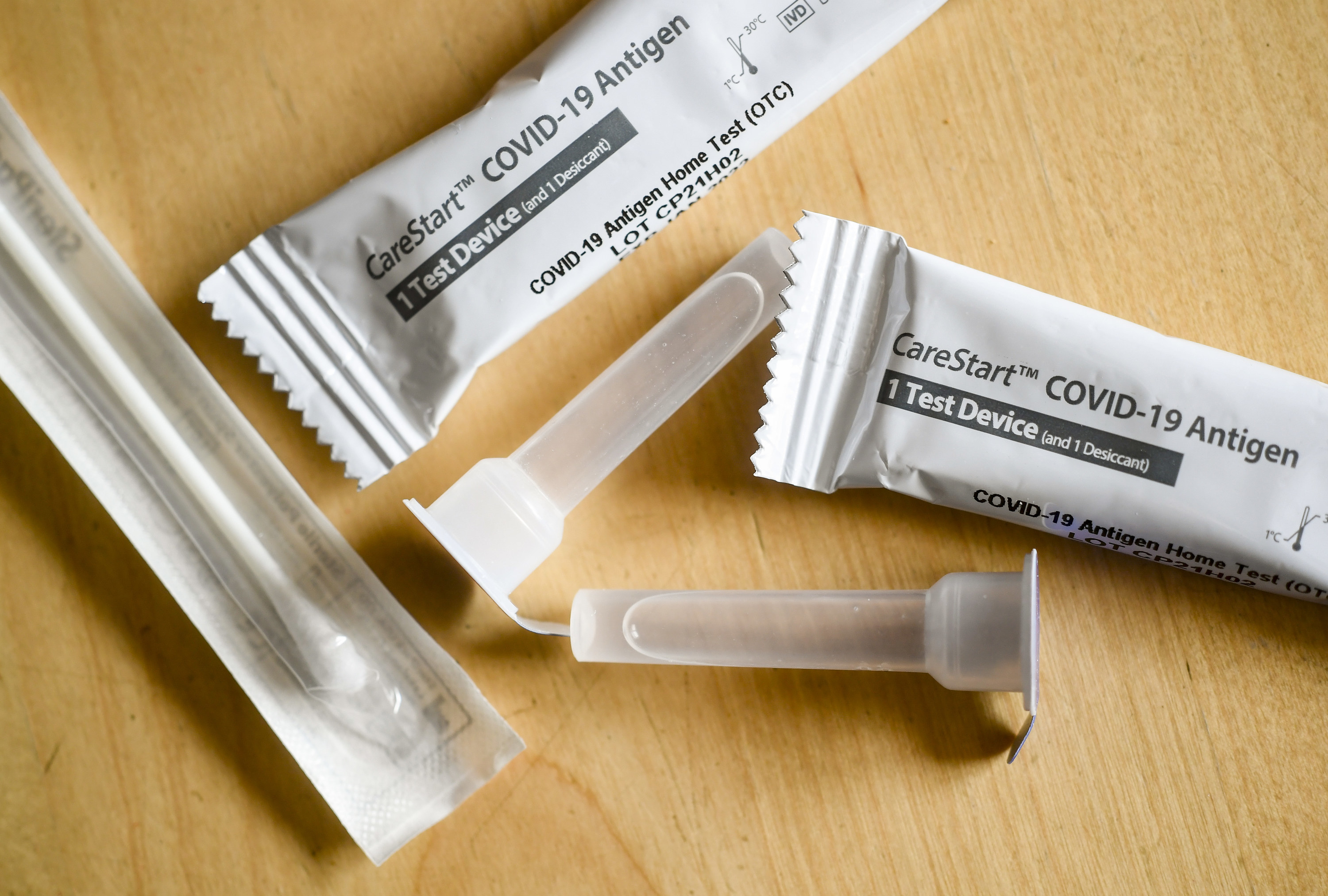
Broadly speaking, there are two kinds of COVID-19 tests: antigen tests, which look for molecules (called antigens) that are viral signatures, and more accurate PCR tests, which identify actual viral genes.
"The tests that are now available, the point-of-care antigen tests, are not as sensitive as the PCR test," National Institute of Allergy and Infectious Diseases chief Anthony Fauci said on NBC's Meet the Press. "But if you do them sequentially, one or two or more, you're going to get a result that would be an accurate result."
The arrival of Omicron also makes the availability of at-home tests more important than ever, experts said. “I wish everyone in the United States could be provided with a batch of free self-tests they could use at home,” Salemi said. “Things are changing very quickly with Omicron — it’s not really good enough to test 48 hours before travel — I’d test right before I walked out the door.”
However, at-home COVID-19 tests run about $10 a pop; reimbursement requires filing a claim for the 150 million Americans with insurance, under the current Biden plan.
“Unfortunately, these tests remain too costly and hard to find right now,” Stanford University School of Medicine’s Joshua Salomon said in an email, “so the extra layer of protection they provide remains the privilege of people, like me, who have been able to find and afford them.”


