The journalists at BuzzFeed News are proud to bring you trustworthy and relevant reporting about the coronavirus. To help keep this news free, become a member and sign up for our newsletter, Outbreak Today.
How long can a nation of 327 million people endure with work and schools closed, lost jobs, and people still dying from a pandemic with no proven treatment?
At least until April 30, President Donald Trump acknowledged on Sunday, backing down from earlier calls to end social distancing measures by Easter. Delaware has a stay-at-home order lasting until May 15. On Monday, Virginia issued one lasting until June 10. Meanwhile, the Imperial College London report from mid-March, which predicted 2.2 million deaths in the US without social distancing measures — a finding that triggered lockdowns on both sides of the Atlantic Ocean — projected a first round of shutdowns could last five months.
The university’s modelers suggested that, after a couple of months off, social distancing might then need to pick up again on Sept. 20.
“We are probably looking at five- to six-month phases, done in different ways and times in different places across the country,” pandemic expert Irwin Redlener of the Columbia University's Mailman School of Public Health told BuzzFeed News. “Putting people through that process will be extremely difficult.”
A recent spate of think tank reports and scientific presentations expand the Imperial College scientists’ vision, suggesting that cities, counties, and towns will need to enact public health lockdowns of varying lengths, with stops and starts based on if and when coronavirus cases hint at rising again.
This cyclical approach to social distancing in order to limit COVID-19 deaths depends on measures such as intensive care unit availability and cases dropping for two weeks or longer. To work — limiting the US death toll to hundreds of thousands of lives lost instead of millions — they demand widespread, fast, and accurate tests; a fortified health care system; and public health officials having the breathing room to track down and isolate new cases before they can spread. Most of all, they require endurance from people nationwide, along with the kind of financial assistance typically delivered to victims of natural disasters rather than economic downturns, noted Redlener, to help as unemployment surges to record heights.
“Once you are doing it, you have to have the patience to see it through,” University of Michigan pandemic historian Howard Markel, who's widely credited with coining the phrase “flatten the curve,” said at a National Academy of Medicine briefing on social distancing last week. “If you pull the trigger off too early, not only will the circulating virus do what it naturally does, but all the economic and social disruptions are for nothing.”
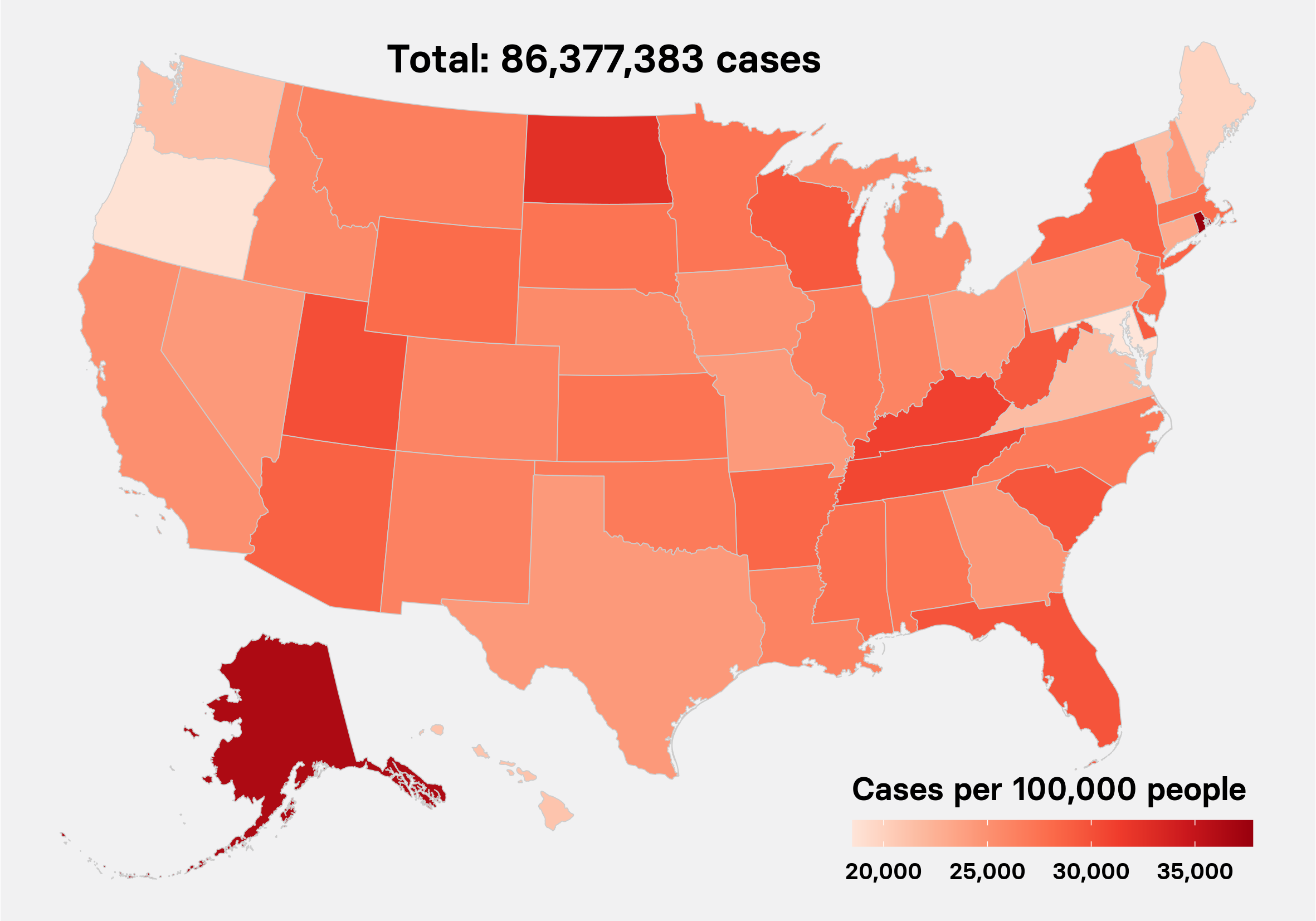
The US is just at the start of its first social distancing cycle, with upward of 186,000 coronavirus cases and at least 3,600 deaths as of Wednesday afternoon. Nationwide, all 50 states have issued emergency declarations, with at least 30 issuing stay-at-home orders, and another four ordering the lesser step of just business closures, according to the National Association of Counties.
Cities such as New York, New Orleans, and Detroit continue to see their case counts climb, while Washington state — where the US's community spread of the novel coronavirus was first spotted in late February — is watching to see if case numbers have perhaps started to flatten.
Even if social distancing measures that started in March in the US work to slow increases, the last half of April is expected to see peaks in cases in these first cities, with more places across the country reporting outbreaks thereafter. California Gov. Gavin Newsom said Tuesday that he expects his state’s cases to peak in May.
“We are not a small town. We are a big country, and it has allowed transmission to continue to a point where most cases are undetected, even now,” Harvard pandemic modeler Marc Lipsitch said at the National Academy of Medicine meeting. “So what we can do is social distancing.”
Without social distancing, the Imperial College London report foresaw 2.2 million US deaths from the coronavirus, a number that Trump referenced on Monday in explaining why he extended federal social distancing guidelines. He added that keeping US deaths an order of magnitude lower — still reaching an estimated 100,000 to 240,000 deaths — was the goal of the effort. “Every citizen, family, and business has a role to play in stopping this virus,” said Trump.
But while the president described 30 days as the end for social distancing, the models he referenced see it as only the beginning. In fact, several of these plans see social distancing as a necessary new normal.
Wuhan, China, which started a severe travel lockdown in late January, is why social distancing is happening in the US now, Lipsitch said. Deaths in the Chinese city of 11 million peaked four weeks after restrictions started — a widely disputed 2,500 people — and those limits are finally set to end on April 8, two months after the city was effectively cut off from the rest of the world. Daily new case counts in China have dropped to as low as 81 on Monday. All eyes will be on the city to see if cases continue to stay low even as it emerges from a lockdown.
One US plan for halting social distancing put forward by the University of Pennsylvania’s Ezekiel Emanuel, a former National Institutes of Health official in the Obama administration, calls for a nationwide shelter-in-place order. The plan includes exceptions for counties with low enough case counts to allow public health officials to trace every case, and would last until June 1, a shutdown of 8 to 10 weeks.
Such a long and severe shutdown would enable US hospitals currently facing unprecedented patient volumes and dangerously low supplies of PPE and ventilators to spread out their caseloads and more easily share resources. Rapid tests could roll out to identify new cases before they lead to further spread, and a certification system for people who already had the virus and were immune could be established in that time. “If these steps are taken, we should slowly open up parts of the economy in June, while requiring those 70 and older, or others at high risk, to continue to shelter in place, perhaps in isolation,” Emanuel wrote in the New York Times on March 28.
A different “road map,” pushed by former FDA commissioner Scott Gottlieb, envisions state-by-state endings to social distancing lockdowns. The loosening restrictions would be timed to hospitals having empty beds and a two-week drop in cases, as well as states having enough caseworkers to trace new infections. Looking past periods of sustained social distancing, teleworking should become the rule, not the exception, Gottlieb said. He has also stressed that more Americans should wear masks on a daily basis, and gatherings should be limited to 50 people, until a third phase of more loosened restrictions seems reasonable.
A 20% reduction in hospitalizations for people with coronavirus-like symptoms in Washington, once the epicenter of the U.S. coronavirus epidemic, offers a glimmer of hope for the region and nation. https://t.co/OgOp7gkEJT
The proposed road maps clearly describe the rules for stopping social distancing so that people will cooperate with the process, say experts. “We’re ringing a lot of bells in this country and we need to know how to unring them,” Michael Osterholm, an infectious disease outbreak researcher at the University of Minnesota, said at a Council of Foreign Relations briefing on Tuesday.
But he called the plans from Emanuel and Gottlieb more aspirational than practical right now. Alongside the massive backlogs of tests and medical equipment shortages, manufacturers are running out of the parts needed to build the massive numbers of ventilators that hospitals foresee needing.
One added unknown factor in the outbreak is the seasonality of the novel coronavirus, said Lipsitch, which changes the calculus of social distancing. If warmer temperatures and higher humidity cut the transmission rate of the virus, as some preliminary studies suggest, then a single longer period of social distancing that cuts into those summer months, when transmission is lower, might be a mistake. If you stop social distancing in June, then cases build until a peak in the warm month of August. If you stop social distancing in August, the next peak comes in October, when it would coincide with the flu season.
Such a rapid rise in illness could overwhelm hospitals in a second wave of outbreaks, like what happened during the 1918 flu pandemic, something to consider when weighing lifting restrictions in northern cities like Detroit as opposed to warmer ones like New Orleans.
“If we tried a policy of one-shot social distancing, it is treacherous,” Lipsitch said. “One-shot social distancing could make things worse.”

Seasonality remains a mystery, said Osterholm, suggesting that as long as 40% to 80% of the public still has no immunity to the new virus, it will likely readily spread regardless. “At this point, I don’t have a clue what is going to happen to the virus,” he said.
The alternative to one-shot social distancing, contemplated by the Imperial College London study and the plan from Gottlieb, is an alternating cycle of tighter and looser restrictions until we have treatment or vaccine options.
Vaccine trials are currently underway, but a usable vaccine is estimated to take at least 18 months to develop, and any vaccine would need to first be made available to health care workers and people most at risk, like the elderly and people who are already ill. Coronavirus vaccines have to be carefully evaluated for their safety because past studies have shown that a vaccine that targets the wrong part of the virus can produce one that's more dangerous, vaccinologist Peter Hotez of the Baylor College of Medicine told BuzzFeed News.
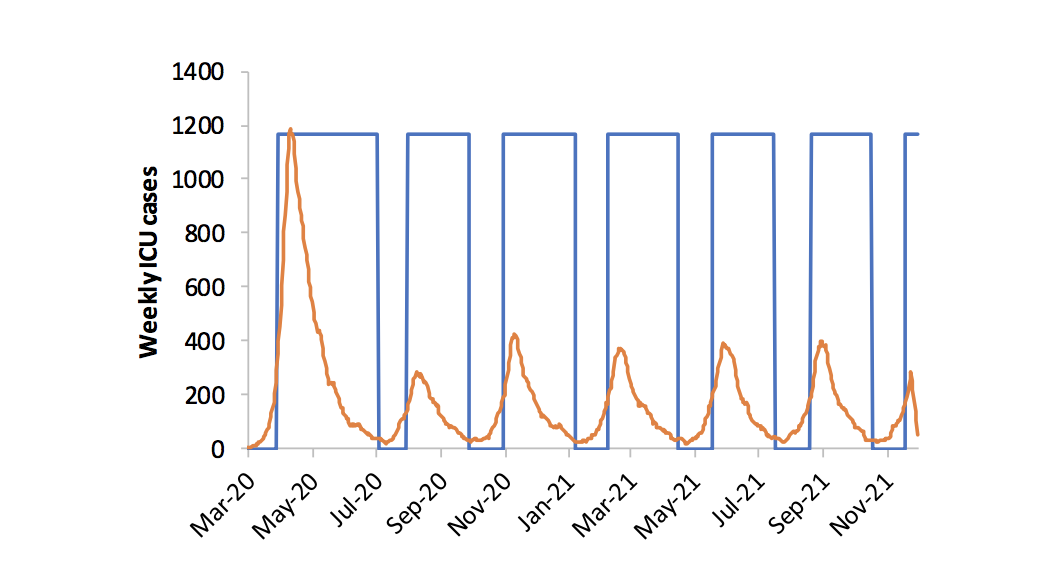
Lipsitch suggested that cycles of turning social distancing restrictions on and off could also be triggered by hospital capacity in a city or state, with loosening happening when hospitalizations fall to 0.2 per 10,000 people and turned back on again when they reach 0.75 per 10,000 people.
This threshold rests on the nationwide average of empty ICU beds, around 0.9 per 10,000 people, but that number varies widely across the country; some rural counties having zero critical care beds. Doubling ICU beds across the country is one measure that would allow for longer pauses between restarts of tighter restrictions.
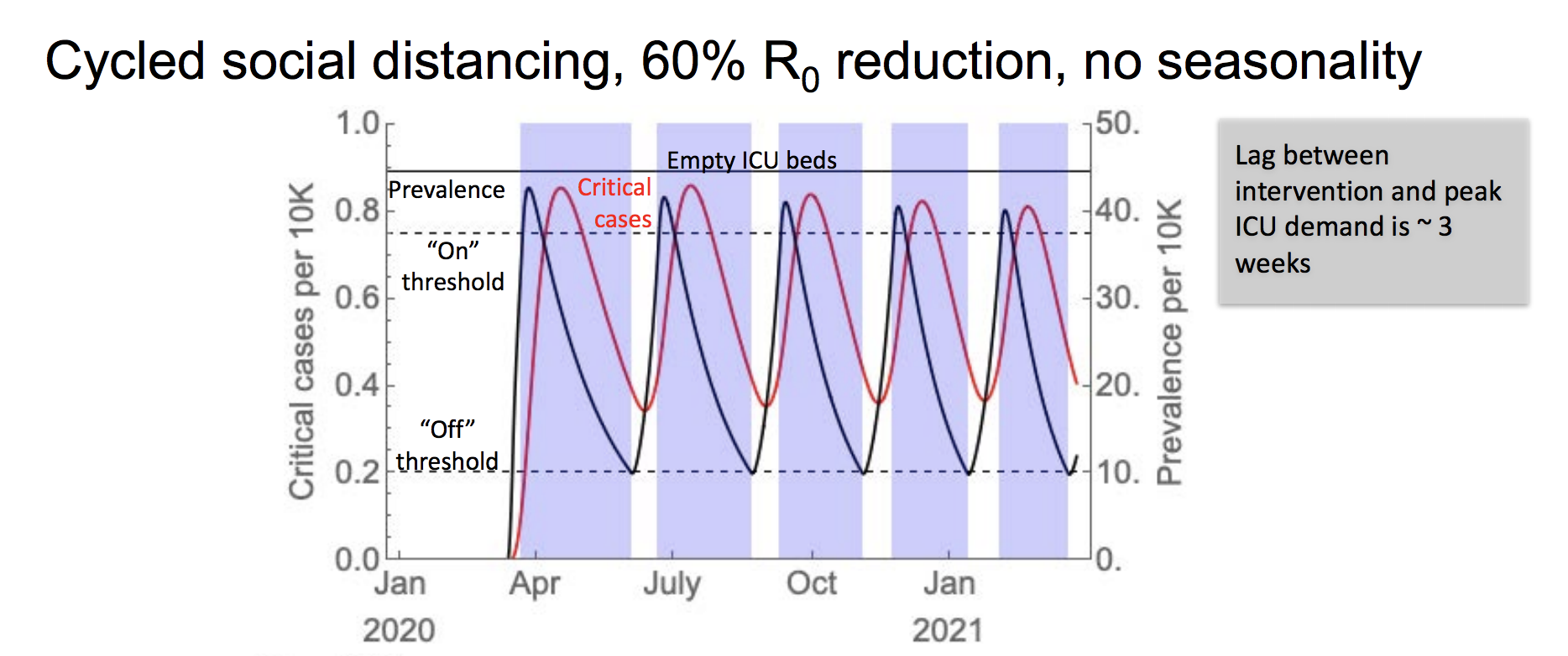
The goal of this is to allow infections to grow at a manageable rate that doesn’t lead to overwhelmed hospitals, while herd immunity to the virus slowly grows in the larger population. A wild card in this will be cases that are imported as travel restrictions ease up, something China is struggling with now.
To be clear we are well aware that extended intermittent distancing is not an attractive option - but are trying to lay out options & likely pub health consequences. Intermittent dist may be best of current bad choices @yhgrad @StephenKissler @ctedijanto https://t.co/pmkmF6CLcG
In all these visions, life would need to emerge changed by the pandemic. Rules about handwashing, keeping apart, and coughing into your elbow will need to become polite behavior. Contrary to the American work ethic, people will have to take sick days when they are sick.
Gottlieb’s road map also calls for erecting a system of recovered case certifications, the driver's license of the coronavirus era, which designates people who can safely go back to work. But questions remain about how people remain immune to the virus. It also requires the development of reliable widespread blood tests for antibodies, which so far has remained maddeningly disorganized, said Princeton epidemiologist Jessica Metcalf, who spoke at the Council of Foreign Relations event on Tuesday. “Where is the CDC in all of this?” she asked. Under those conditions, business and then schools might open on a voluntary basis.
Other experts have suggested we might see the establishment of a waiting room approach to daily life. Testing could be required before entering the grocery store or other essential businesses, especially if rapid tests become widespread, Baylor molecular virologist Joseph Petrosino told BuzzFeed News. “You pull into the parking lot, and a drive-through testing center takes a sample. And then you wait in the car with your phone until you are cleared to work,” he said.
Such testing would start with health care workers, and then expand as capacity increases. For this to work, we will need to develop a widely available, nationwide genetic test for the active presence of the virus, something still missing from the US response. South Korea has pioneered this sort of approach, with widespread testing allowing better control of its outbreak, at least so far.
All of that is far from the current reality in the US. Testing availability is still the bottleneck across the country, where some jurisdictions have been forced to restrict tests to the sickest patients; elsewhere, shortages of reagent and even cotton swabs have limited how many tests can be run. Private labs have also struggled with a backlog of tests. Like many scientists, Petrosino had transformed his lab, which normally investigates the genes of microbes turned up in the field, to create testing kits in order to help test Baylor’s doctors and nurses for infections.
The waiting room approach to managing the spread of the coronavirus could be helped by a small portable testing device by biotech company Abbott, which received FDA approval on March 27. Touted at a White House event on Monday and aimed first at urgent care centers, the machine takes just five minutes for a positive result and 13 minutes for a negative one. People will have to be more patient if such widespread testing is rolled out — making every day like a visit to the DMV, waiting for your number to be called to go to work or else test positive and face quarantine and interviews from health workers trying to trace the origin of the case.
“Just sheltering forever in our homes is not likely,” Nicholas Christakis of Yale’s Human Nature Lab, said on a JAMA podcast on Tuesday. Some states, like Kentucky, which instituted restrictions early, might end them sooner than states like next-door neighbor Tennessee, which waited until longer and has seen higher case counts. “We need to figure out how we are going to live in a time of plague.”
However these cycles of social restrictions play out, they will leave a changed nation, hopefully ending with herd immunity, better treatment, better testing, and a vaccine, Christakis said. Perhaps all of these would help stop the number of deaths currently seen across the world.
“The truth is that a lot of these decisions are going to have to be made by state and local leaders who won’t have perfect information about what to do, so the response is going to look different everywhere because every place is different,” said Redlener, the Columbia public health expert. He expects tighter restrictions to last longer in hard-hit locales, given a natural reluctance by political leaders to see fatalities rise again in their community.
“We are going to learn a lot of lessons here about ourselves,” he said. “I’m hoping we come out of this a stronger, more resilient people.”