There are only a few people left in the US still using the iron lung machine; 82-year-old Mona Randolph of Kansas City, Missouri, is one of them.
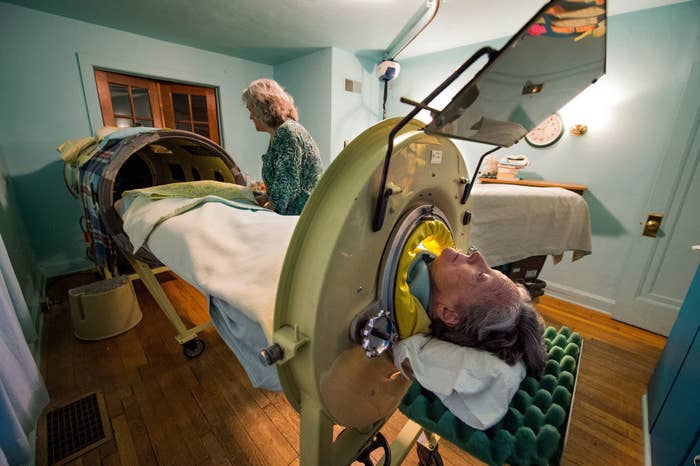
Randolph was 20 years old when she contracted polio, an infectious disease caused by a virus that attacks the spinal cord, which can cause paralysis and death. The polio vaccine had been approved the year before, in 1955, but Randolph didn’t get it in time because adults were considered lower risk than children.
Her polio symptoms started with a bad headache, fever, and a sensitivity to sound and light. “I couldn’t stand to hear people talking in the kitchen. They’d whisper and it would hurt my ears. I couldn’t stand any light,” Randolph told the Kansas City Star, which first reported the story.
Several days after getting sick, Randolph had trouble breathing and was taken to a hospital in Kansas City, Missouri. Doctors immediately put her on an iron lung, a mechanical respirator that uses negative air pressure to push air in and out of the lungs in patients who can’t breathe on their own. Iron lungs were commonplace at the time, but very few people rely on them today.
How many machines are still being used in the US? “No one knows for sure, but I would guess somewhere between three and five,” Brian Tiburzi, executive director of Post-Polio Health International, told BuzzFeed News.
Randolph survived polio, but her left arm was paralyzed and she depended on family and friends for help. According to the Star, she received rehabilitation at a clinic in Warm Springs, Georgia, where president Franklin Delano Roosevelt, who also had polio, was treated.
Although she eventually went off the iron lung, Randolph developed post-polio syndrome in the 1980s — a weakening of the muscles that can happen years after recovering from polio. It took such a concentrated effort to breathe, like lifting weights, that Randolph started using the iron lung again.
Randolph spends her nights in the 6-foot-long tank respirator, which helps move her lungs so she can breathe. During the day, she relies on a simpler machine.

Today, Randolph still sleeps in the nearly 75-year-old machine six nights a week — she calls it her “yellow submarine,” according to the Star. It takes about one hour to get situated inside the iron lung, and she is usually helped by her husband, Mark, or a caretaker.
The airtight, 6-foot-long metal tube covers her body up to her neck, so her head is exposed. The machine is very loud when it’s turned on, but it’s the only way Randolph is able to sleep — and breathe normally — through the night. She has been using the iron lung for the last 36 years.
The massive metal machines were developed in the 1920s to help polio patients breathe after the virus had weakened or paralyzed muscles in the chest — a stage that was often fatal. After widespread implementation of the polio vaccine during the 1950s, disease rates plummeted in the US and the machines became nearly obsolete.
During the day, Randolph can use a continuous positive airway pressure (CPAP) machine, which delivers a constant stream of air pressure through a mask worn over the face or nose. It’s a common treatment used for sleep apnea. The machine is more modern and portable, but is not without problems. Randolph told the Star that her CPAP machine is uncomfortable and prone to breaking.
Polio can be prevented with a vaccine. It has been eliminated in the US, but still infects people in other parts of the world.

Poliovirus, the cause of poliomyelitis, is highly contagious and spreads from person to person and through contaminated food or water. It mainly affects young children, and there is no cure.
In the US, polio was once a feared disease that caused massive outbreaks and paralyzed thousands of people each year, usually children. The first polio vaccine became available in 1955, and an oral version of the vaccine was developed in 1963, according to the Centers for Disease Control and Prevention (CDC). In 1979, polio was eliminated in the US, meaning no cases have originated in the country.
Despite a global effort to eradicate polio completely, cases still occur (there were 22 in 2017) in some parts of the world and could be brought into other countries by travelers. The best way to prevent polio is to get vaccinated, which also protects those who can’t get the vaccine by creating herd immunity.
Randolph told the Star that she believes “getting vaccinated is the thing to do” and that people should also act according to their faith. “It’s a personal decision. But something like vaccinations that you can see the proof of with epidemics just seems more logical,” she said.
