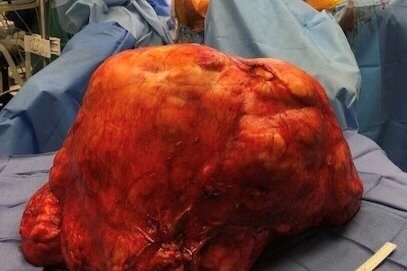
A 47-year-old man from California is on the mend after having surgery in July to remove a 77-pound tumor from his abdomen that he initially thought was just weight gain.
Hector Hernandez of Downey, California, was often teased by friends for his “beer belly,” even though he didn’t drink beer. “I just thought I was fat,” Hernandez told the Washington Post.
Exercise didn’t seem to affect his stomach — which became hard to the touch — but his arms were getting thinner. After his family convinced him to see a doctor, Hernandez learned that his so-called beer belly was not a result of weight gain but actually a giant cancerous tumor, according to a statement from the University of Southern California.
The diagnosis? Retroperitoneal liposarcoma, which is a rare form of cancer that begins in fat cells located toward the back of the abdomen, Hernandez’s surgeon, Dr. William Tseng, told BuzzFeed News. Tseng, who is a surgical oncologist at Keck Medicine of USC, explained that liposarcomas can develop in any part of the body, but they often occur in the abdomen or limbs. The exact cause is unknown.
Tseng specializes in treating sarcomas, so he typically removes abdominal tumors in the 20 to 30 pound range every few weeks — but other doctors may only see this rare cancer once in their lifetime, he said. However, Hernandez’s 77-pound liposarcoma was definitely the “biggest he’s ever taken care of.”
How did it get so big? This rare cancer sometimes isn’t that easy to notice, especially in the early stages. “We never really know exactly how long these tumors develop for but we think that they do grow slowly, over years,” Tseng said. Because the tumor starts in the back of the abdomen, it gradually displaces other organs as it grows, and the patient’s body basically “adapts” to it, he explained. So from the outside, the abdomen may just appear bloated or larger than usual — by contrast, a liposarcoma on an arm may look like a more obvious lump.
“That’s one reason it can get to such a huge size. ... [Another] is that patients often don’t have any pain with these tumors,” Tseng said. The other symptoms, like fullness or constipation, could be easily mistaken for another gastrointestinal problem. “A person who has this probably wouldn't think, ‘oh, I have something terribly wrong going on inside me,’” Tseng said.
Once a person is diagnosed with a liposarcoma, the most common treatment is surgery, Tseng said. Sometimes, radiation is also used to destroy cancer cells.
After a 6-hour operation, during which Tseng had to carefully navigate around important organs and major blood vessels in the abdomen, Hernandez’s tumor was successfully removed, in one giant piece. The cancer hadn’t spread to other organs, but Tseng said he did have to remove one of Hernandez’s kidneys that he could not separate from the tumor.

“To be able to take it out safely and see him enjoy a good quality of life after, that’s a big thing,” Tseng wrote in the statement from USC. Hernandez has made a full recovery, according to the latest update on a GoFundMe page his friends created to help him with his medical bills.
With the 77-pound mass in his abdomen gone, Hernandez feels much lighter and more energetic, he told the Washington Post.
Although he does not need to receive chemotherapy, Hernandez will need frequent checkups and CT scans, Tseng noted. Unfortunately, liposarcoma often returns, and patients like Hernandez have to be monitored closely even after their abdominal tumor is removed. “There’s a very good chance that it’ll come back in his lifetime. ... These patients sometimes have to get more than one surgery, or even many surgeries,” Tseng said.
“We’re still working on finding better ways to treat this rare disease. We need more than surgery ... and we need more research,” Tseng said.