
The journalists at BuzzFeed News are proud to bring you trustworthy and relevant reporting about the coronavirus. To help keep this news free, become a member and sign up for our newsletter, Outbreak Today.
Harvard. Apple. Biden’s campaign rallies. The list of organizations and events migrating to online platforms multiplies daily. Moving these hubs of in-person interaction to a virtual space is a critical part of flattening the curve of coronavirus spread — and although I’m sure these changes were not always simple to enact, the last few weeks have shown they are exceedingly possible. Seeing these dramatic changes implemented in a span of weeks has been heartening. It has also been deeply frustrating for those of us in the disability community, who've been asking for these accommodations — and been told they're simply not feasible — for our entire working lives.
Disability advocates like Karrie Higgins have been quick to point out that these same accommodations have long been requested by people in the disability community, and long been denied. Using the hashtags #AccessibilityforAbleds and #DisabledAndSaltyAF, the disability community is gathering stories and keeping receipts of accommodations that they have found extremely difficult to obtain, or flat-out been refused, but that are now being rapidly adopted. The perception is accommodations like online instruction, paying for sick leave, and single-use products have been deemed too difficult, or not worthwhile, to provide to the disability community — but organizations are willing and able to provide now that the health of able-bodied people is at stake. I understand we are in the middle of a terrible public health crisis, and I don’t mean to take away from the seriousness of this situation — instead, I want to encourage people to pay even closer attention to changes taking place now.
Disability is generally very misunderstood and very unacknowledged, even though approximately 25% of Americans live with a disability. The last few years have delivered important gains in representation along many axes of diversity, but representation of people with disabilities has lagged. As a result, the narratives about what a disabled person can look like, or what disability means, remains extremely limited. Embarrassingly, I was almost 30 before I learned that it was possible to have an invisible disability — and that I was someone who qualified as disabled.
When I was 20, I began to feel electric shocks in the right side of my face. I felt it first only when brushing my teeth. Then when chewing any kind of food. Eventually, even cold air over my face or lips set off blinding shocks. I saw half a dozen doctors and dentists, but no one could see anything wrong. The shocks got worse and worse: It felt like electrified barbed wire being continually flossed through my right jaw, eye, and cheek. Five months after the initial onset, I sent myself to NYU’s emergency room after almost blacking out in pain. There, a kind Texan dental resident diagnosed me with a chronic pain condition called trigeminal neuralgia (TN). TN is a rare condition that typically only impacts one side of the face (though some people have bilateral TN) and is widely regarded as one of the most painful known medical conditions. It is nicknamed “the suicide disease.”
Embarrassingly, I was almost 30 before I learned that it was possible to have an invisible disability — and that I was someone who qualified as disabled.
There is no surefire treatment for trigeminal neuralgia, and it generally doesn’t respond to pain medication. In fact, the pain increases in frequency and intensity over the course of one’s life. Over the years, I saw countless specialists and countless charlatans, took many cocktails of medication, and underwent dozens of medical procedures. Some of it helped a little; some of it helped a lot; none of it ever helped for long. As this happened, my life went on. I worked as an adjunct professor, writer, and office manager. I cultivated tricks that helped me get through speaking engagements: I only smiled with the left side of my face, and chewed on the left side of my mouth. I told jokes or asked students to read text out loud, which gave me a few seconds to stop talking. Throughout my twenties, I kept this equation running: Which hours of today can I least afford to be in pain? Which hours of today can I most afford to be in pain? How much pain do I think I can be in before I’m no longer effective at what I’m doing?
Sitting for long stretches of time and increases in air pressure would reliably flare up my neuralgia, so I generally turned down engagements that required extensive travel — but I was living on an adjunct professor’s salary and couldn’t afford to turn down all of them. I had one medication I took on an in-case-of-emergency basis (primarily because of the price tag: $200 for 60 pills). Prior to flights, I did what many poor Americans do and hoarded medicine to ensure I’d have enough to tide me through the post-flight pain spike, as well as the major speaking and networking obligations. As a trade-off, I spent the days before flights sequestered at home practicing disgusting personal hygiene, while speaking and eating as little as possible. For 10 years, this method of hoarding medicine and hoarding sick days worked well enough, until I was finally referred for a surgery that might give me a shot at being pain-free. A microvascular decompression craniotomy (MVD) is a three- to four-hour brain surgery that requires drilling a quarter-inch hole through the skull to wrap Teflon around the trigeminal nerve, insulating it from further compression. It’s a scary and serious surgery that isn’t guaranteed to work, but it was the first hope I had of truly alleviating my neuralgia. I said yes without hesitation.
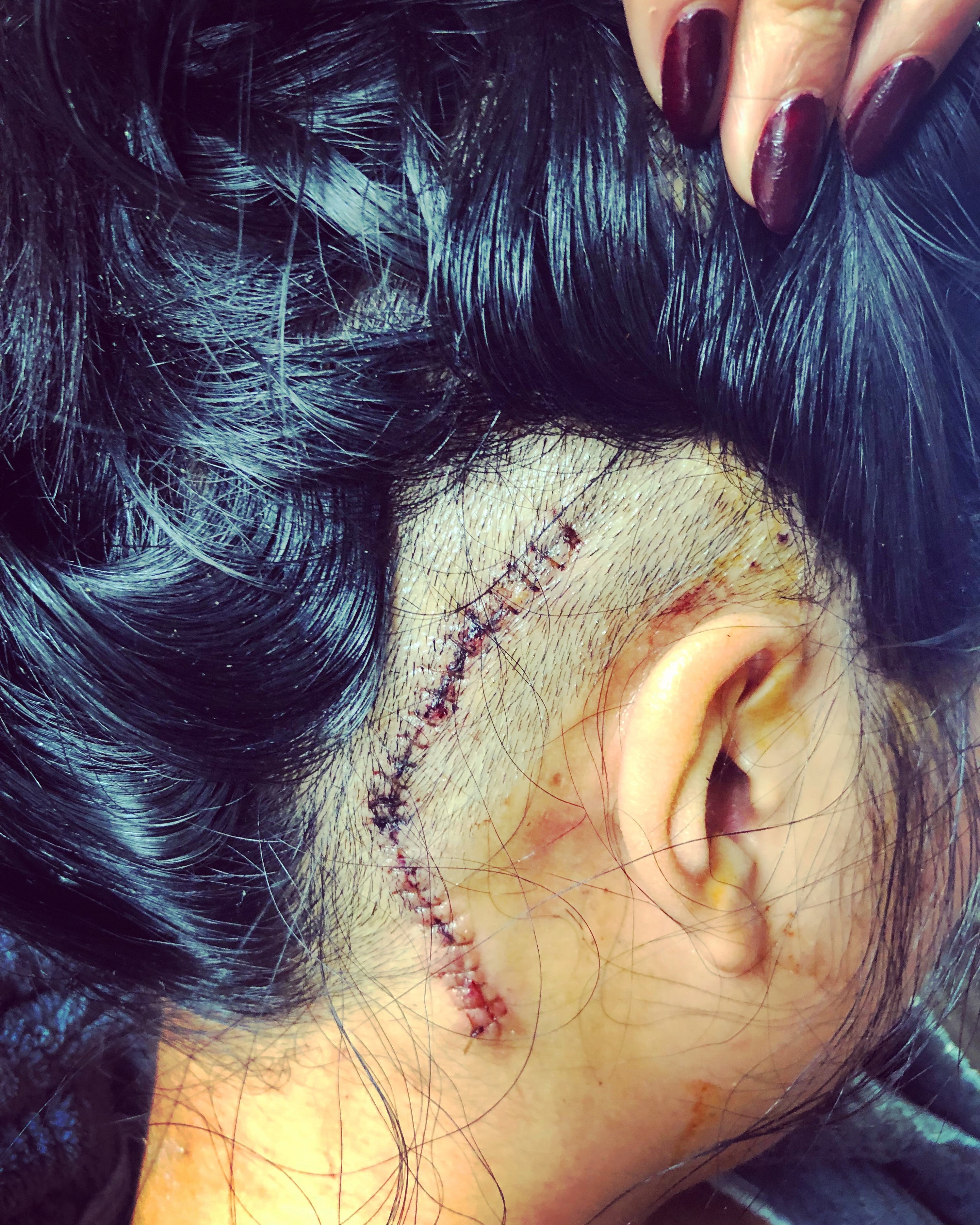
It was in the lead-up to my surgery that I was finally introduced to the disability community. When looking for people who had gone through an MVD, I began to find support groups online, many of which pointed me to chronic pain groups, and then wider disability networks. The more I read about the experiences of people with disabilities, the more I saw my own experience. The differences between myself and able-bodied people came into sudden, sharp focus. For the first time in 10 years, I realized an able-bodied person doesn’t experience pain so intense it hinders their swallowing or breathing reflex. An able-bodied person doesn’t get jolted awake by electric shocks every 20 minutes the entire night. An able-bodied person isn’t in constant negotiation with their body. For many in the disability community, this is just the reality of our bodies. And we figure it out. Even when we’ve been told telecommunication is not possible. Even when we’ve been told online instruction is not possible. Even when we’ve been told paid sick leave is not possible.
For many in the disability community, this is just the reality of our bodies. And we figure it out. Even when we’ve been told telecommunication is not possible.
America’s response to the coronavirus has exposed many, many systemic shortcomings — the vulnerability of tipped workers, the lack of standardized paid sick leave, and the tenuous capacity of the health care system, to start — but it’s also shown our capacity for positive change. The willingness to move classes, conferences, events, work, and interviews online for the sake of public health is a great indicator of what could happen in the future. Seeing this changing day by day, I can’t help but think: What about all the times the same organizations said no to these accommodations? And what happens to these new initiatives after the coronavirus becomes less of an imminent threat? Maybe this experience means all these organizations will see the benefits of remote work. Maybe a silver lining to COVID-19 is increased flexibility in these policies across the board. Having that option would be a boon to many in the disability community — and would have massive benefits beyond the disability community. But it’s hard to be hopeful.
One of the first things I learned when I started reading about the disability community was the spoon theory. Created by Christine Miserandino, the idea goes like this: Think about the energy you have every day represented in the form of spoons. Healthy, able-bodied people tend to have an unlimited number of spoons. Every action you take consumes one spoon, but because you are healthy and able-bodied, with unlimited spoons, it’s no big deal. You might go running in the morning, and then commute to work while reading the paper; you might grab lunch with a friend, and then go on a date; you might end the night at home, watching Netflix after picking up some ice cream from the bodega.
On the other hand, if you have a disability or a chronic illness, you have a limited number of spoons every day. Every action you take consumes one spoon, and after each step, you’re left to consider what you can do with the spoons you have left. Sometimes you finish getting ready for your day and you’ve already used half your spoons, so you have to be strategic about where the rest go. You might be able to borrow spoons from the next day, or save spoons — similar to how I used to hoard medication — but it means you borrow against yourself, and that is a debt you will always have to pay.
It can’t be solely the task of someone with a limited supply of spoons to fight for accommodations that have widespread benefit, especially when there are people with unlimited spoons sitting right next to them. During this coronavirus outbreak, healthy, able-bodied people have been important allies to more vulnerable populations and stood alongside members of these communities. Now that we’ve seen the kind of accommodations that are possible, we should work to formalize these into permanent policies. Allowing more flexible and standardized teleconferencing policies across the board is not just helpful for the disability community: It can be helpful for people who are immunosuppressed; for new parents; for the environment; for people who can’t afford the plane ticket; for people who are caretakers; for people with social anxiety — the list goes on.
Allowing more flexible and standardized teleconferencing policies across the board is not just helpful for the disability community.
I have been extraordinarily lucky. I underwent my MVD surgery in April 2019, and since that time I have had no more pain from trigeminal neuralgia. For the first time in a decade, I do not need to take any daily medication. I can eat and breathe and move without constantly monitoring my body. Some things do remain: I have a permanent wad of Teflon in my brain, which protects my trigeminal nerve; I have a titanium plate covering the borehole in my skull; I have a 5-inch scar under my hair; and if you touch the right side of my skull, you can feel a permanent dent at the incision site. Although my neurosurgeon has a great track record, the trigeminal neuralgia could return anytime. Every few months, I run the equations again: How old might I be when this happens? What other medical conditions might I have at that point? Should I undergo brain surgery again? What if I continue to relapse? Out of curiosity, how much more can my skull sink in? What if next time there are no more options?
It is easy to forget physical pain. Once recovered, it is easy to forget what illness felt like — as the saying goes, “health is a crown only the sick can see.” I lived with neuralgia for so long it will always be part of me. And for all us, in this moment of pandemic, we are learning about ourselves as individuals, as members of a community, and as people capable of compelling change in institutions and organizations that would otherwise resist change indefinitely. Even when the pandemic is over; even when the vaccines have been distributed; even when we trickle back into schools and offices; remember this time when you fought to help people, to be a good citizen and an inclusive neighbor. Then do it again. ●
