Ernestine Coon reclined in her hospital bed at The Connecticut Hospice with a colorful blanket covering her legs, watching seagulls soar over the water from her second-floor room. Longtime friends chatted with Coon as the slender, silver-haired grandmother prepared to do something she’d never done in her 70 years: Try marijuana.
One year ago, Coon visited the doctor and left with a diagnosis of ovarian and uterine cancer. Now, with doctors giving her about six months to live, she has constant pain in her abdomen and back, and has signed on as patient number five in the nation’s first federally approved trial to see if medical cannabis can sufficiently reduce pain in dying patients so that they can reduce their use of opioids. The study, which was announced in December and began in May, could change how millions of dying Americans treat severe pain, and open the door to alternatives to prescription painkillers blamed for a nationwide epidemic of addiction and overdose deaths. It’s expected to run for at least a year, and the goal is to enroll 66 on-site patients who are well enough to swallow capsules filled with cannabis extract, but whose pain is so bad that they require prescription medication to manage it — patients like Coon, one of the 1.3 million US hospice patients facing certain death and hoping to make it as pain-free as possible.
“You’re talking to someone who never did drugs,” Coon said, her voice scratchy. “It wasn’t my thing.”
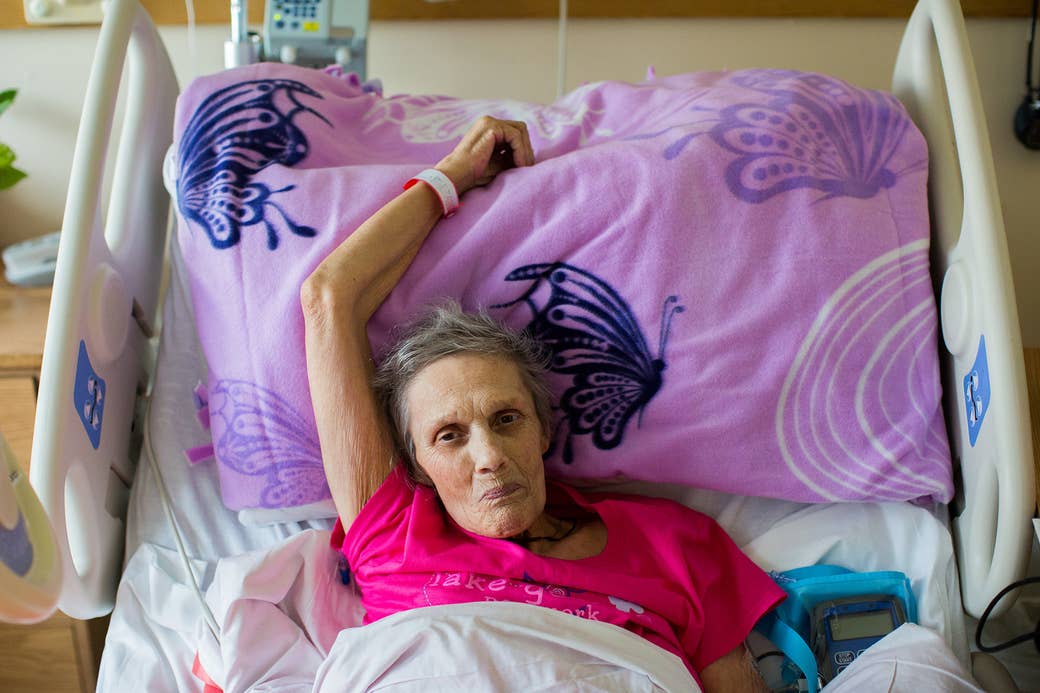
That has changed as her disease has progressed and her pain has worsened. Coon — an energetic woman who brags that she rarely was ill and was never hospitalized except when she gave birth — now has trouble walking, sitting up straight, or playing with her grandchildren. “Since I was diagnosed with this, I’ve probably taken medicines that in my wildest dreams I never even thought I would be taking,” Coon said, craning her neck to see her two friends, Fran and Ann, who were sitting nearby. Ann held Coon’s hand. Fran grabbed a photo from the windowsill that showed Coon at her happiest, healthiest self — grinning in the midst of a pile of grandkids.
“In fact, I’m going to give myself a dose,” Coon said as she pressed a button that looked like a buzzer. It pushed a small dose of Dilaudid, a powerful opiate, into her body through a pump.

A “tree of life” is etched on the glass at the entrance to The Connecticut Hospice, which sits on the shore of Long Island Sound and serves 3,000 people each year. The nation’s first hospice, founded in 1974, treats pain in a variety of ways, from a visit with Lizzie, an eager golden retriever therapy dog, to some of the strongest painkillers available. But the drugs’ side effects — drowsiness, confusion, and nausea, among others — add to the agony of gravely ill patients and their relatives, who want their loved ones to be alert in their final days.
The cannabis study was designed in part by Wen-Jen Hwu, a Yale School of Medicine graduate and former fellow at the hospice, who watched families endure the misery that often accompanies conventional drug care, and who concluded that, sometimes, it’s more humane to address the symptoms rather than continue treating the disease.
“The tradition is narcotics, and more and more narcotics. But, that makes patients more lethargic, more confused, and have nausea, vomiting, and poor appetite and depression,” said Hwu, now an oncologist at MD Anderson Cancer Center in Texas and a board member at The Connecticut Hospice. “I do believe that the marijuana can definitely reduce the amount of the opiates that we need for our patients. More importantly, it can help them to feel better than they actually are.”
“The tradition is narcotics, and more and more narcotics."
Rosemary Hurzeler, CEO of The Connecticut Hospice, urged staff to take on the trial. She anticipates that the ripple effect could be “enormous.” “I think there’s going to be a big chance for other hospices to take a swing at this in their own state,” Hurzeler said. “But, it has to be standardized and that’s what the feds are doing in giving us this opportunity to demonstrate this.”
From start to finish, it took three years for Jim Prota, the hospice’s pharmacy director, and his colleagues to bushwhack through red tape to get the clinical trial off the ground. The idea of using marijuana for medical reasons isn’t new — the movement was born out of the AIDS crisis in the ‘90s, and 29 states and Washington, DC, now allow medical marijuana in some capacity. But in the eyes of the federal government, cannabis is an illegal drug, so the hospice had to gain approval from the Food and Drug Administration. It also needed the Drug Enforcement Administration to give its permission for the hospice to distribute a Schedule 1 drug, the category the federal government reserves for drugs it considers to have a high potential for abuse and no medical value.
“Maybe there is a drug beyond the opioids that can influence, a little bit, their quality of life.”
Decades of research support marijuana’s efficacy in treating pain. A RAND Corporation study found a link between legal cannabis dispensaries and a reduction in opiate-related deaths, which reached 33,000 in 2015. Sen. Elizabeth Warren has asked the Centers for Disease Control and Prevention to examine “the impact of the legalization of medical and recreational marijuana on opioid overdose deaths.” Nora Volkow, director of the National Institute on Drug Abuse, coauthored an article in July that said there is “strong evidence of the efficacy of cannabinoids” in pain treatment. The article said that medical cannabis could “provide a powerful new tool” in the fight against opiates.
Hurzeler agrees and hopes that the hospice staff’s research leads to broader use of marijuana as a “beautiful new drug” that lessens anguish for people suffering terminal illnesses.
“Maybe there is a drug beyond the opioids that can influence, a little bit, their quality of life,” she said. “And we always say that we want to add days to life and life to days.”

Hospice care providers across the country have said the same thing: Patients are talking about pot even in states — like Kentucky — that have highly restrictive medical cannabis laws. Brian Jones, director of Hospice and Palliative Care Programs at St. Elizabeth Healthcare in Edgewood, Kentucky, said more and more patients want to know if cannabis is available and legal, and how much might be enough to help with their symptoms.
Jones has noted an increased interest in cannabis and palliative care in the years since he gave a talk in 2014 on medical cannabis to a national group of hospice providers at the National Hospice and Palliative Care Organization. He’s hopeful about The Connecticut Hospice study. “If it’s shown to be effective in Connecticut and perhaps some other studies as well, you’ll see a greater interest. There’s no doubt,” he said.
“I truly believe that the cannabis is our solution."
But the law and science haven't caught up with public opinion about medical marijuana, and national hospice organizations haven’t come around to the idea either. NHPCO, the country’s largest organization representing hospice and palliative care programs and professionals, hasn’t taken a position on the use of medical cannabis, and “currently does not comment on the issue,” said Jon Radulovic, vice president of communications for the organization.
This is due in part to federal drug laws that make it nearly impossible for hospices to advocate for pot as a pain reliever. In 2011, a study in the Journal of Palliative Medicine found that health care workers in hospices “are generally in favor of legalization of marijuana and, if legalized, would support its use in symptom management for their terminally ill patients.” But hospices risk losing federal reimbursements and other funding if staff provide marijuana to patients as long as the government classifies it a Schedule 1 drug.

The feds’ rules limit research on medical marijuana, which Hwu says makes some doctors uncomfortable with it, further hampering attempts to make it part of accepted palliative care. The Connecticut trial could help remove that stigma, she said.
“I truly believe that the cannabis is our solution. But I can’t say that to you, and convince anybody, until we have the clear evidence to show the facts, to tell people that it improves their quality of life in the end stage of their disease,” Hwu said.
With medical cannabis legal in Connecticut, the clinical trial has strong support from state elected officials. Gov. Dannel Malloy and Sen. Richard Blumenthal attended the news conference at which the trial was announced last December.
“There is a need for pain management, but there are better alternatives. And that’s why the research to be done here is so critically important. It is really groundbreaking. It can help save lives,” Blumenthal said, offering a challenge to any federal attempts to quash the medical marijuana movement. “And if any attorney general thinks he is going to turn back the clock, or roll back the progress we have made, he is in for a fight,” he said to loud applause.

Whole-plant marijuana and its products are already used during palliative care outside of the traditional hospice and hospital settings. Santa Cruz, California, is home to the Wo/Men’s Alliance for Medical Marijuana, a cannabis collective that has been compared to a traditional hospice. Director Valerie Corral helped pass the country’s first medical cannabis law in part to help people die more peacefully.
WAMM members grow marijuana for themselves and one another to treat symptoms related to a variety of serious and terminal illnesses. Since a local ordinance approved the use of marijuana for medicinal purposes in 1993, WAMM volunteers have helped more than 500 people die using whole-plant marijuana. That’s a different form than the capsules being used in the Connecticut study, but the goal is the same: to make people more comfortable in their final days. Pot cannot replace drugs like morphine, said Corral, herself a medical cannabis patient, but it can help to distract a dying patient from the pain.
“Pain can trap one in the body. It can make it nearly impossible to get away from that deep suffering. So, cannabis can be helpful to amplify the usefulness of opiates,” she said.
Corral recalls one of the first members of WAMM, a man with cancer in his mid-forties who was hours from death in the early '90s and in a coma-like state. She shotgunned a joint, meaning she lit it and blew cannabis smoke into his nostrils as he inhaled. Corral recalled that, after the third time he breathed in marijuana, the man smiled, gave a thumbs up, opened his eyes, and talked to his family — before he died an hour later.
One challenge facing The Connecticut Hospice trial is that some patients still see marijuana as a street drug, unlike traditional therapies. And even though most of them are suffering from advanced cancer, end-stage Lou Gehrig's disease, and other painful illnesses, if they or their families have struggled with past drug or alcohol abuse, they’re hesitant to join because of concerns about relapse. “I’ve had problems with alcohol in the past. I guess once an alcoholic, always an alcoholic,” said Rick Wright, a thin 61-year-old who sat in a wheelchair puffing on a cigarette. Wright suffers from bowel and liver cancer and would have been a good candidate for the trial, which has so far enrolled patients aged 59 to 70, but he chose not to participate.
“I think maybe if I had seen a lot of other patients using it, I might have,” he said as a harpist plucked away nearby and other patients sat in their wheelchairs outside, taking in the ocean breeze.
Coon’s daughter, Tanya, helped her mother make the decision to take part in the study. She knew more about the possible benefits of medical marijuana than her mother, and discussed the trial with Prota. “I think the impression was that it would make her high,” Prota said of his conversations with Coon. “She didn’t know how she would feel since she never used it recreationally.”
"And toward the end of my life, maybe I can go out with my grandkids to the park and watch them run around.”
In fact, the medical cannabis pills don’t get people stoned. The clear capsules given to patients contain a dark, tar-like cannabis extract high in cannabidiol (CBD), known for its medicinal benefits. They are low in tetrahydrocannabinol, or THC, the ingredient in marijuana that gets people high.
Coon’s decision to participate had as much to do with managing her pain as trying to enjoy life as much as possible, given how little time she has left. Three times a day, she swallows a dose under the watchful eye of medical staff, who monitor her vital statistics and quiz her on her pain. Coon is still also taking opiates, and it’s too early to tell if the cannabis will enable her to taper her Dilaudid doses.
But Coon feels more in control of her treatment now that she’s working with the doctors on a scientific study. And she’s more hopeful than before — thinking that maybe in addition to relieving pain, medical marijuana will prove to have curative effects.
“I know my life expectancy, what they say, is not good. But if I could postpone it a month, a day, 10 months, three months, it will all be worth it if they can manage my pain,” Coon said. “And toward the end of my life, maybe I can go out with my grandkids to the park and watch them run around.” ●
UPDATE
Ernestine Coon died Aug. 23, with family and friends at her side. "She is no longer in pain and is watching us all, including her beloved grandchildren," her son, Thomas Coon, wrote in an email to BuzzFeed News.
The data that staff at The Connecticut Hospice collected while Coon participated in the medical cannabis clinical trial will be incorporated into its research. No other patients have yet been enrolled in the trial.