BuzzFeed News has reporters around the world bringing you trustworthy stories about the impact of the coronavirus. To help keep this news free, become a member.
After months of stress, Americans have been looking forward to the pre–COVID-19 pleasures of a (socially distanced) 4th of July. How about a cookout? It's a traditional, low-key summer celebration — but amid the nation's growing outbreak, even a simple home-cooked meal comes at an exorbitant price.
A BuzzFeed News investigation reveals the extent to which the virus — and the nation’s inadequate response to it — has infected, sickened, and even killed workers up and down the nation's food supply chains as they work to keep our refrigerators full.
Take a typical summer feast: tangy ribs, a side of creamy pasta salad, and a slice of freshly baked apple pie. If you shop at a Walmart Supercenter, in, say, Massachusetts, the apples you’d buy would have been picked by workers in Washington state’s Yakima Valley, who live in a crowded labor camp with few protections in place. The fruit would then be sorted into boxes in an Allan Bros. packhouse, which for weeks failed to follow federal COVID-19 safety guidelines — even after employees started falling ill.
The ribs would have been sliced and packed by employees at a pork processing plant — like the Tyson Foods facility in Indiana that stayed open for weeks, even as the virus spread through its staff.
The pasta would have been stacked by grocery clerks whose employer was slow to close down for a deep cleaning after workers got sick, and to inform the local health department and customers of the growing outbreak.
From those three workplaces alone — the Allan Bros. packhouse in Yakima Valley, the Tyson plant in Indiana, and the Walmart in Massachusetts — around 1,100 employees have tested positive for COVID-19, and at least four have died, according to a BuzzFeed News investigation based on government documents, company memos, and interviews with around 50 workers, managers, local officials, and labor advocates.
Worried about putting themselves and restaurant staffers at risk, many Americans have turned to home cooking as a safer, more ethical option. But what may seem safer for consumers can still be deadly for the low-paid, often immigrant workers who make up America’s sprawling food supply chains. Across the country, from fields to packhouses to slaughterhouses to grocery stores, companies failed to require masks, build protective barriers, or arrange testing until after outbreaks had spread through the workforce. Some workers in the chain still do not get sick pay, forcing them to choose between spreading the virus or missing out on paychecks — between feeding your family or protecting their own.
“I'd just like to see them keep us safe,” Dennis Medbourn, a worker at the Tyson plant in Logansport, Indiana, where three coworkers he knew have died from COVID-19 complications, told BuzzFeed News. “We’re working a lot of hours, too, to try to make up for the meat shortage.”

One grocery worker, Yok Yen Lee, a door greeter at the Walmart in Quincy, Massachusetts, continued to report to work up until days before she died from COVID-19.
“She was really hardworking,” her daughter, Elaine Eklund, told BuzzFeed News. “She absolutely loved that job. She wanted to do that job for her whole life.”
The paths through which food reaches Americans’ plates originate on farms and in factories in small cities and rural towns before making their way across the 50 states. The networks are intricately interrelated, which means that the people who live in those areas and work in those jobs, along with the friends and relatives they come into contact with, shoulder a disproportionate share of the risk to keep the nation fed. An apple picker at a FirstFruits Farms orchard in Yakima Valley appears to have caught the virus from her husband who worked at a Tyson beef plant in the area, according to Erik Nicholson, vice president of United Farm Workers. FirstFruits didn’t respond to a detailed request for comment.
Are you still working during the coronavirus pandemic? We'd love to hear your story. Reach out at albert.samaha@buzzfeed.com or via one of our tip line channels.
Since the start of the pandemic, around 29,000 workers at grocery stores, meatpacking plants, and other food processing facilities have been infected nationwide, and at least 225 have died, according to the United Food and Commercial Workers International Union. This is almost certainly an undercount: Many companies have declined to order widespread testing, even at workplaces where employees are falling ill. As a result, the full scope of infections among frontline food workers may never be known.
“What this pandemic is making very clear is that some of our most underpaid, marginalized, and exploited workers are, in fact, our most essential,” said Vermont Sen. Bernie Sanders, who co-sponsored a bill with other Senate colleagues in June to provide protections for the country’s agricultural workers. “Every plate of food reflects a disturbing reality: Food-supply workers — from farmworkers to grocery store clerks — are risking their lives every day to keep us fed, often in unsafe conditions, and far too often making starvation wages.”

“If they don’t work, they don’t get paid — and if they don’t get paid, they don’t eat.”
On April 30, Angelina Lara felt an itch in her throat.
For seven months, she’d worked as a fruit packer for Allan Bros., one of at least 18 produce companies in Yakima Valley, a fertile agricultural zone that rolls east across central Washington from the mighty Cascade mountain range. Lara, 48, grew up in Southern California but moved to the city of Yakima in 2005, following relatives who had come for the jobs at the valley’s plentiful packhouses. Around a third of the local jobs there are in agriculture, more than the next two industries combined. Apples are one of the main businesses in town, and the fruit is at the center of the Yakima city seal. Central Washington accounts for 60% of the nation’s apple production.
Over the years, Lara worked at numerous packhouses, including a previous stint at Allan Bros. She returned to the company last year for a job that paid $13.50 an hour, more than the $12 minimum wage she made previously. Inside a squat warehouse on Highway 12 in the foothills of Mount Rainier, Lara and her fellow day shift employees washed and sorted apples, which are packed and shipped year-round in the region. Around 300 workers clock in for the day shift, standing along a brisk conveyor belt about 2 feet apart, sorting apples, like the organic Fuji variety sold at Walmarts across the country, and separating out fruit that’s been spoiled or infested with worms. (The night shift handles seasonal fruit, such as cherries.)
It’s hard, tiring work, Lara said, and “it’s impossible to be 6 feet apart because at times the line moves so fast that you need somebody to help you with all the apples.”

As COVID-19 was spreading across the state and the country in March and April, Allan Bros. added plexiglass barriers to the office area where management and administrators worked. “But the same was not put in the warehouse,” said Shauri Tello, who moved from Mexico to Yakima when she was 15 and began working in the fruit industry shortly after she graduated high school at age 18, two years ago.
The company hadn’t yet begun providing workers with masks, so some workers brought their own from home, according to four employees and a memo from health officials who inspected the site on May 8.
Lara didn’t immediately assume the itch in her throat meant she’d caught the coronavirus. At the time, she didn’t know if anyone at work had been infected, she said. Still, she stayed home from work the next day as a precaution. Within 24 hours, she had developed a fever. Then she began to have trouble breathing. Lara has asthma, but this was worse than any asthma attack she had ever had. “I was home alone, so I started panicking,” she said. At the hospital, she said, she paid for the COVID-19 test herself — $152 — and it came back positive.
Lara informed Allan Bros. that, under doctor’s orders, she would stay home and quarantine for two weeks. She and another worker who tested positive said that company officials told them that their leave would be unpaid.
She asked her supervisor to “let [her] coworkers know so they can take precautions,” Lara said. “They never did it. Nobody even knew I was sick.”
Three of her coworkers corroborated that claim, saying that management didn’t tell them about any cases at the plant in April and early May. In an emailed statement in response to questions, Allan Bros. denied failing to inform employees about cases until May but declined to specify when it began doing so.
Today, Yakima County has the highest rate of per capita COVID-19 cases in the Pacific Northwest — about 1 for every 34 people. In central Washington — as in other areas such as California’s Imperial and San Joaquin valleys — the agricultural industry is experiencing a reckoning; the methods for packing produce and housing migrant workers that have been maximized for efficiency have created the ideal conditions for the spread of a devastating virus.

“When farmers were designing farmworker housing and warehouses in which fruit is sorted, they were in no way considering pandemics,” said Dr. Malcolm Butler, the officer for the combined health district of Chelan and Douglas counties, which lie north of Yakima and are home to some 20 agriculture companies. “They built an industry and fed the world, and unfortunately social distancing is not possible. It’s very challenging and extensive to retool an entire industry at the drop of a hat.”
By late April, the virus had been quietly spreading among apple pickers and packers in central Washington for weeks. The scope of the outbreak remained unknown, in part because many companies were reluctant to arrange comprehensive testing. But even the available case numbers at the time revealed that the region’s fruit workers were facing a mounting threat.
Two weeks before Lara got sick, on April 13, three apple pickers at the Stemilt Growers farm in Douglas County, 70 miles north of the Allan Bros. facilities, developed coughs, according to a court statement from Stemilt’s human resources director, Zach Williams. These three were among the thousands who entered the country on temporary work visas, known as H-2A, for jobs at the region’s farms. While packhouses are largely staffed with local residents who have lived in Washington for years, fieldwork is mostly done by seasonal laborers who ride buses up from Mexico for gigs that can last upward of six months.

Sixty-nine of those workers were housed at Stemilt’s “North District” housing facility, Williams stated. They slept on bunk beds in rooms shared with as many as three others. They also shared a kitchen, a laundry room, and several bathrooms. In the mornings, they piled into vans that carried 14 of them at a time to the orchards.
The company began implementing new procedures to protect workers from COVID-19 as early as March 13, after a worker at a different Stemilt housing facility tested positive. In a memo to employees, Stemilt said that vans and common areas across the company would be sanitized every night and throughout the day.
Those measures weren’t enough.
While the three North District workers were awaiting their test results in mid April, three others at the camp began showing similar symptoms. Ultimately, all six tested positive, according to Williams’ statement. Over the next few days, Stemilt coordinated with local health officials to begin testing all the workers from the North District camp, as well as the eight local crew leaders who worked with them. All the crew leaders tested negative, but 44 of the 69 guest workers tested positive. When Stemilt conducted another round of testing on April 22, nine more workers tested positive. Most of the cases were asymptomatic. No one was hospitalized.
The state’s Employment Security Department said it expects 27,000 H-2A jobs in 2020. Stemilt declined to comment for this story.
Stemilt was the exception — not in terms of its explosion of cases, but because it looked for them at all. Though local officials in nearby Yakima County offered to organize free testing at all produce industry workplaces, only one fruit company, Columbia Reach Pack, had taken them up on it by late May, according to local health department documents. At most fruit companies in the region, workers only got tested if they showed symptoms or were exposed to a confirmed case, and then called health authorities. Still, by the third week of May, more than 300 fruit workers in the region had tested positive, and health officials identified outbreaks — a workplace infection rate of at least 5% — at seven of the county’s 18 produce companies.
Allan Bros., where Lara worked, was one of the companies that declined to test its workers. Danielle Vincent, a spokesperson for Allan Bros., denied that the county offered to test all its workers — though other companies confirmed the offer, and government documents show that local health officials were “Awaiting Response” from Allan Bros. on an inquiry about whether the company “Want[s] Employee Testing.”
Though 19 of 515 employees at its packhouse had been diagnosed by May 21, the company did not schedule widespread testing, according to local health department records. Workers had to decide whether to risk going to work and getting sick, or staying home and not getting paid.
“The fear of every worker that I know is that they may come down with the virus. And if they don’t work, they don’t get paid — and if they don’t get paid, they don’t eat,” said Erik Nicholson, national vice president of United Farm Workers.

COVID-19 exacerbates long-standing power disparities between farmworkers, some of whom are undocumented, and their employers, noted Beth Lyon, a law professor and founder of Cornell University's Farmworker Legal Assistance Clinic.
And while the country has deemed them “essential” during a pandemic, most farmworkers can be fired at will, making many hesitant to advocate for safety measures.
This is particularly true of guest workers, whose visas are directly tied to their employer. “If they speak up for health protections like masks or social distancing, they are likely to lose not only their livelihood but also their housing” and their permission to be in the United States, Lyon told BuzzFeed News.
Local officials and farm owners attribute some of their slow reactions to the pandemic to the lack of direction at the federal level. That’s led the industry to “take care of itself” said Butler, the Chelan–Douglas Health District officer.
“The difficulty we’ve had was that there was absolutely no guidance on what was the right way to house H-2A workers,” he said.
Sean Gilbert, who leads Gilbert Orchards, said the Centers for Disease Control and Prevention's changing position on masks left his company in a conundrum. In March — as the country’s top public health agency told citizens not to use masks and to save them for healthcare professionals — orchard and packhouse operators donated a few thousand N95 masks they had gathered for fire season to local hospitals. Weeks later, when the CDC changed its guidance, those businesses were left scrambling, facing stiff competition and spiking prices for face coverings as the rest of the world competed for mask shipments.
Gilbert, whose operation includes 4,000 acres of orchards and 1,200 workers during peak season, noted that apples are a “labor-intensive business” with small margins. As a result of social distancing measures, the packhouse could only prepare 10,000 boxes of apples per shift from late March to the end of May, rather than the typical 12,000.
“Keeping people apart means that people can’t hand off things in a process,” he told BuzzFeed News, “and it slows the process down.” He added that protective equipment and hazard pay add a further squeeze on Gilbert Orchards’ economics. “COVID has fundamentally changed how we do business.”
Yet he didn’t see the need to allow health officials to test all his employees. Gilbert Orchards — where at least 26 of the 350 or so employees in the packhouse, shipping, and administrative departments have been diagnosed — declined Yakima County’s offer to arrange testing at the facility and instead suggested its workers take advantage of the free testing sites local officials had set up around the valley.
Gilbert said part of his reasoning was fear of upsetting his employees. “I turned down their offer to bring in a National Guard unit to quarantine our facility while they escorted people to and from testing tents,” he told BuzzFeed News. “I felt that requiring that of all employees would have been potentially traumatic.”
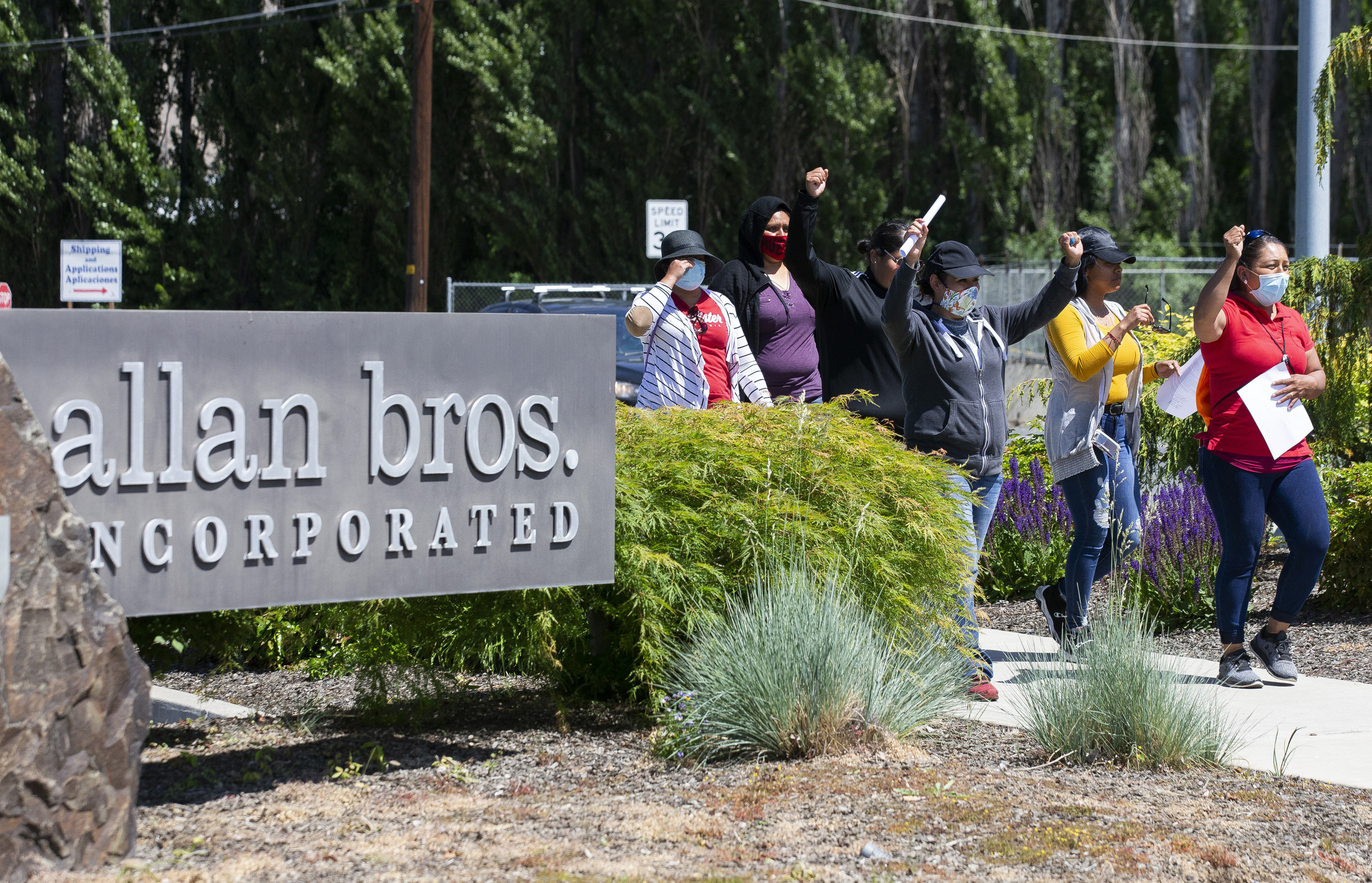
If guest workers are among the most vulnerable employees in the produce industry, workers who live year-round in central Washington are only slightly more secure.
Lara’s diagnosis, she said, threw her family into a precarious financial position. Her husband, who works at the same warehouse, and her two sons, who work as nursing assistants, tested negative but stayed home as a precaution in case they subsequently caught the virus from her. The household of four went without a paycheck for two weeks. Lara qualified for unemployment insurance because she’d been diagnosed, and her husband and sons may be eligible for family leave benefits — but whatever government money they’d receive wouldn’t come soon enough to meet the bills coming due. The family burned through years’ worth of savings in a matter of days, she said.
Back at Allan Bros., meanwhile, workers in the packhouse said the company still hadn’t distributed masks, and as the cases mounted, many were growing angry.
On May 7, dozens of Allan Bros. workers went on strike over conditions they said were unsafe; in the days that followed, around 500 workers from six other fruit companies joined them. When Lara’s quarantine ended, she took a spot in the line of workers holding signs by the road, chanting through colorful cloth masks. Local lawyers and union representatives estimated that the labor action was one of the largest they’d seen among agriculture workers in Yakima, reminiscent of the marches César Chávez attended in the county in the 1980s.
Nearly every day, at each of the seven strike locations, the workers encountered local white residents driving by, shouting at them to get back to work, said Cristina Ortega, an activist who participated in the strikes. She recalled those drivers saying things like “If you don’t like it, get out.” On another occasion, a man shouted out his car window that he was going to “come back and shoot you all,” according to a Yakima County Sheriff’s Office incident report and written witness statements. When deputies later caught him returning to the scene, he told them that Allan Bros. “treats those people very well and they should not be protesting,” according to the incident report. The man was arrested and charged with malicious harassment.
The backlash against the striking workers reflected a long-standing resistance to Yakima’s growing Latinx population for some. Latinx residents accounted for 15% of the city’s population in 1980, 30% in 2000, and 50% in 2018. Still, no Latinx candidate had been elected to office in the city until 2015, after a federal judge ruled that the city’s previous system of at-large council seats violated the Voting Rights Act. In 2016, a majority of the county’s residents cast their ballots for Donald Trump.
Three weeks into the strike, Lara finally went back to work. Allan Bros. had installed protective barriers in the packhouse, offered a $1-an-hour pay raise, and started providing masks, according to Lara and three coworkers. Though she has been cleared of infection, she still has trouble breathing and sleeps sitting up most nights. She said her doctor told her it might be months before she feels normal again.
She considers herself fortunate, she said. One of her coworkers, 60-year-old David Cruz, got sick a few days after she did. His wife and daughter tested positive too, Lara said. He had worked at the plant for 12 years, most recently putting together boxes on the upper level of the warehouse. When Lara saw him on breaks, he was “always positive, getting along with everybody,” she said. On one of the last days of work before the pandemic hit, Cruz told Lara about his plans to visit his mother in Mexico for the first time in years. “He was very happy he was going to see her,” Lara recalled. “He was planning for June or July.”
He died on May 31. His coworkers collected $4,000 to give to his wife. The mood at the packhouse has been somber since.

“Wow. It spread out really, really quick.”
Every morning at the Tyson pork plant in Logansport, Indiana, a low-slung town of 18,000 that’s located at the intersection of three highways and surrounded by livestock ranches, farmers deliver the hogs to the kill floor, known colloquially as the “hot side.”
There, the pigs move through pens, into a machine that stuns them, and then onto a conveyor belt that carries them to the knife that slits their throats. On a normal day, Tyson’s kill floor processes five hogs every 16 seconds, according to Dennis Medbourn, a 52-year-old worker who sets the speed on the machines. Workers stand elbow to elbow along the production line, peel the hog’s skin off, cut through its center, remove its guts, and hang its carcass on a hook that takes it to the plant’s refrigerated “cold side.” The movements are strenuous and repetitive; to try to prevent injuries, ergonomic monitors — their official job title — walk up and down the line checking on the welfare of workers.
An ergonomic monitor on the hot side, a 16-year Tyson veteran who requested anonymity out of fear of losing his job, began seeing some of his coworkers wearing cloth masks they brought from home in early April.

Outbreaks were beginning to pop up at meatpacking plants around the country. Tyson had instituted temperature checks at Logansport but hadn’t yet installed plexiglass barriers or distributed any protective equipment — even though another Tyson pork plant, in Columbus Junction, Iowa, had closed on April 6, leaving the company all the more reliant on its other five hog slaughterhouses.
“That’s when everybody was thinking, Man, why don’t they close our plant?” said Medbourn. “You’d hear people coughing and stuff. People weren’t showing up for work more than usual.”
Tyson declined to comment on whether its Logansport plant increased production during that period, but a spokesperson, Liz Cronston, said, “The level of production at which we determine to operate in our facilities is dependent on ensuring team member safety.”
The company has maintained that its response to the pandemic was swifter than most. Cronston noted that Tyson began seeking masks for workers even before the CDC recommended their use, and it was one of the first companies to proactively test all employees for COVID-19. “If we learned a team member had tested positive for the virus, we notified co-workers who had been in close contact,” she said. “Our priority and focus have been the protection of our team members and their communities.”
The ergonomic monitor tried to maintain a few feet of distance when he checked on workers — but the long, open-tiered plant was loud with the whirring of electric saws, the rumble of conveyor belts, and the echoing clangs of metal. He sometimes had to lean in close to talk and hear, he said. He interacted with around 200 workers each day. Tyson began requiring employees to wear masks in mid-April.
On April 23, with rising case numbers at several facilities, Tyson organized COVID-19 testing for all 2,200 of its workers in Logansport.
The monitor and others on his shift filed into a big white tent in the parking lot, “all pushed together to get out from the rain” as nurses swabbed their noses, he said.
A few days later, he got a call informing him of his result: He had COVID-19 — one of 890 Tyson workers to test positive by the end of April in Logansport, a staggering 40% of the plant’s workforce. Like most of them, the monitor showed no symptoms at the time of diagnosis, although he did recall feeling unusually tired the previous week. He shuddered at the thought that he may have infected the people he saw every day.
“I wouldn’t have suspected if I didn’t get tested,” he said. “I was really freaked out. Just, like, wow. It spread out really, really quick.”
Tyson closed its Logansport plant for two weeks starting on April 25. All six of its pork plants have had outbreaks of at least 200 cases, and five have temporarily closed. At one point, four of the country’s five largest known outbreaks in meatpacking plants were at Tyson sites. To date, around 8,500 Tyson workers have tested positive, more than the company’s three biggest industry competitors combined, according to data compiled by the Midwest Center for Investigative Reporting.
But Tyson’s standing at the top of this list isn’t necessarily because its plants are more dangerous than those of its rivals, but because the company has been more committed to determining how many of its employees have been infected, even though revealing those numbers almost guarantees a plant’s closure. The other big meat companies — JBS, Smithfield Foods, and Cargill — haven’t conducted comprehensive testing at most facilities, even as meat processing plants became widely known as incubators for the virus.
“We believe it’s imperative that we share our experience addressing this pandemic because safety is not a point of competitive advantage,” said Cronston, Tyson’s spokesperson. “Results from these tests have allowed us to find team members who have the virus but don’t have symptoms and would not otherwise have been identified.”
For Tyson, JBS, Smithfield, and Cargill, closing a plant sends a ripple effect across both ends of the supply line. The four companies produce around 85% of the meat sold in the US, churning out pork, beef, and poultry in massive facilities staffed by the thousands of employees needed to reach output goals. The concentration of meat production into a few dozen mega-plants has led to lower prices but has also left the system vulnerable to major disruption, adding further pressure on workers to help keep the plants going.
Tyson is the largest buyer for many farmers around the country and one of the largest suppliers for many groceries, including Walmart. A plant closure can lead to lost wages for livestock sellers at the start of the chain and barren meat shelves for consumers at the end. “Our plants must remain operational,” CEO John Tyson wrote in a full-page ad in the Washington Post and New York Times in late April, noting the company’s “responsibility to feed our country.” The Trump administration codified that idea into law with its April 28 executive order granting meatpacking corporations immunity from legal liability for sick workers.
As Tyson got ready to reopen the Logansport plant, it notified employees through an automated text service that starting May 6, “If eligible to work, you will be required to work all scheduled hours in order to receive the guarantee pay.” Workers would receive a $30 “daily show up bonus” for all shifts through the end of May, another text stated. A May 8 text told employees that if they had been “symptom free for the last 72 hours without the use of any medication you can report to Tyson” — though the message didn’t include CDC’s additional recommendation that those diagnosed should only stop isolating at least 10 days from the onset of symptoms. One worker, a loin cutter in the cold side, told BuzzFeed News that he didn’t feel symptoms until 12 days after he tested positive, just as his two weeks of paid quarantine time was ending, leaving him temporarily without a paycheck as he applied for short-term disability to cover additional time off.

Tyson maintains that its policy has been clear: “Any team member who has tested positive will remain on sick leave until they’ve satisfied official health requirements for return to work,” Cronston said.
But some Logansport workers vented their frustrations on a private Facebook group called “Tyson Talk,” expressing dismay at the company’s plan to reopen even while nearly half of its workforce was under quarantine. They also shared health updates; on May 5, a group member wrote in both English and Spanish that someone from the slaughter side had died from the virus.
In fact, at least three workers at the Logansport plant have died of the coronavirus, according to local health officials and a union steward at the plant.
Tyson officials refused to confirm the number of workers who died. “We’re deeply saddened by the loss of any team member,” Cronston said. “We don’t have a number to share.”
Tyson also declined to provide an update on the number of confirmed cases at the plant since the 890 reported in April, but local health officials estimated that “over 1,000” of the plant’s workers have tested positive.
Cass County, where Logansport is located, has nearly triple the rate of COVID-19 cases per 100,000 people compared to the rate of the next highest Indiana county, and Tyson’s pork processing facility is one of the area’s largest employers. Tyson was “absolutely the hot spot” for COVID-19 in the county, said Serenity Alter, the administrator for the Cass County Health Department.
The Tyson plant reopened on May 6. The company ramped up production as quickly as its workers could return, accelerating from half-capacity to nearly full capacity within two weeks. It provided face shields, built plexiglass barriers in the cafeteria, and expanded its cleaning staff.
“All you can do is wear one of these masks and wash your hands,” a Tyson senior manager in Texas said of the risk that meatpacking workers face during the pandemic. “I gotta assume most of the people in our facility have been around or interacted with someone who was positive.”

Two months removed from the Logansport plant’s mass testing, some workers are still infected with the virus, though Tyson won’t say how many are now out sick.
“We currently have very few cases,” Cronston said. "We are aware of no positive cases of any team member currently working in our facility."
When he returned from his quarantine, the ergonomic monitor wore a mask and kept several feet of distance from the coworkers he checked on. At the facility last month, he and others walked past a daily reminder of the cost of producing pork through the pandemic: A memorial of wreaths and photos in the common area honored the three workers who have died from the virus. It stayed up until the middle of June.

“We weren’t prepared to lose her this suddenly.”
While fruit pickers and meat-packers labor out of view of consumers, grocery clerks serve at the public-facing end point of the supply chain, the final set of hands to touch your food before you do. As grocery stores became all the more critical to keeping people fed during lockdown, their safety protocols soon concerned not just the workers who spend their days there but the customers passing through.
In March, as the US declared a state of emergency, panicked shoppers flocked to supermarkets to hoard toilet paper, flour, and pasta; in stores around the country, shelves began to empty. Some lined up in the early morning for a first crack at the inventory. Many didn’t wear masks.
It didn’t take long for the virus to reach the Walmart Supercenter in Worcester, Massachusetts, which has an online inventory that includes Tyson pork ribs and Fuji apples from Rainier Fruit, Allan Bros.’ distributor. (A spokesperson for Walmart said that Tyson pork ribs are not on the store’s shelves at this time.) On April 27, the store posted on Facebook that it would close on April 30 for a single “day of deep cleaning and sanitizing” before reopening early the next morning. Some shoppers from the postindustrial city around 50 miles from Boston were horrified.

“How do you ‘deep clean’ in one day??" a commenter wrote.
But while shoppers had the option of staying away from the store, some of Walmart’s workers felt they did not. Despite the widespread testing shortages at the time, the company’s COVID-19 emergency leave policy didn’t offer additional paid time off to staffers unless they tested positive or were subject to mandatory quarantine — a policy that advocates said is too narrow as it doesn't clearly cover workers who feel ill, are immunocompromised, or need to care for a sick relative.
By the end of April, Walmart knew that a growing number of employees in Worcester — as well as in another store in Quincy, an hour’s drive away — had contracted the virus, which was quickly spreading through the state. Although the company had released a plan detailing how they’d keep workers safe a month prior, the stores weren’t providing staffers or local public health departments with enough information about sick workers, records show.
“We have had consistent problems with Walmart,” Quincy’s health commissioner, Ruth Jones, wrote on April 28 to the Massachusetts attorney general’s office. “They have a cluster of Covid cases among employees and have not been cooperative in giving us contact information or in following proper quarantine and isolation guidelines.”

Yok Yen Lee, a 69-year-old door greeter at the Quincy store, was so fearful of contracting the coronavirus that she used most of her accumulated paid time off in March and early April when case numbers in the US began to skyrocket, her daughter, Elaine Eklund, told BuzzFeed News. Shortly after Lee returned to work in mid-April, she began to feel sick but assumed she’d caught a cold from spending her eight-hour shift standing outside in near-freezing temperatures. On April 11, the Quincy Health Department contacted Walmart to inform the store that one of Lee’s coworkers had tested positive for the coronavirus. Although Walmart had waived its normal attendance policy in March, Lee continued to clock in, afraid of losing her job if she took more days off, Eklund said.
Walmart’s website says it began requiring employees to wear masks on April 17. But one current Quincy checkout employee, who asked to remain anonymous for fear of losing their job, said management told employees in April that masks weren’t necessary. Sometimes there would be 500 people in the store and no social distancing in the employee back rooms, according to the employee. “It was like corona was a myth,” they said. A Walmart spokesperson declined to comment on these specific allegations.
Lee had worked at the store for about 15 years, after emigrating from China in the 1980s and working a series of retail jobs. Colleagues described her as a joyous woman who doled out hugs and danced spontaneously but also showed a tough side when it came to dealing with rude customers.
Lee told at least one colleague, the checkout employee, that she had a slight cough. She had attempted to apply for extended leave, but found the process, which was managed by a third-party administrator, exceedingly complicated as she primarily spoke Cantonese, Eklund said. On April 19, Lee didn’t feel well at work and went home early. The next day, she had a fever and couldn’t get out of bed. Paramedics, with the help of a maintenance worker, cut the lock to her door and rushed her to a hospital, where she was intubated. Her request for extended leave from Walmart was approved on April 28, as she lay bedridden in the ICU, Eklund recalled.
She would have turned 70 last week. Instead, she died on May 3 — one of at least 22 Walmart employees killed by COVID-19 nationwide, according to United for Respect, a labor advocacy group. Lee left behind a daughter and two grandchildren, including one who was born in December.
“She never even got a real family picture with her grandson,” Eklund said. “We were starting to become a complete family. We weren’t prepared to lose her this suddenly.”
Only after Lee died did the Quincy Walmart close its doors. It soon emerged that 33 other employees there had contracted the virus.
The Worcester Walmart became one of the largest clusters in the state, with 82 employees ultimately diagnosed with COVID-19. It was also one of the largest outbreaks at any grocery retailer in the country.
By the time the store posted on Facebook about the daylong cleaning in late April, local officials were investigating the situation. Public health inspectors obtained an internal company list showing that nearly two dozen employees had tested positive for the coronavirus before the store closed, 20 within a one-week time period, Walter Bird Jr., a city spokesperson, told BuzzFeed News.
They also reviewed a photo of a sign instructing staffers to work their scheduled shifts during that April 30 cleaning: They were expected to help “clean, sanitize and stock” the store alongside a third-party cleaning service so it would be ready to open the next morning.

The city of Worcester issued a cease-and-desist order that day, “forcing the store to close immediately,” Bird said. It was the first time any US Walmart was closed by the government. The store didn’t reopen until May 5, after the company agreed to test all of the store’s nearly 400 employees.
The outbreaks in the Quincy and Worcester Walmarts were caused by “dangerous working conditions” present at other branches, as well, according to a complaint recently filed with the Occupational Safety and Health Administration by United for Respect, which surveyed stores nationwide. The complaint claimed that Walmart didn’t provide sufficient paid sick leave to its employees, “thereby pressuring people to go to work even if they have symptoms or have been exposed to the virus.”
The complaint also alleged that Walmart didn’t enforce social distancing and had failed to quickly close stores for cleaning and disinfecting after employees were exposed or diagnosed — as was the case in Worcester and Quincy — allowing the virus to spread further among employees and the public.
All these failures violated state and federal guidance for employers, the complaint alleged.
“Communities across the country have suffered from coronavirus cases, and with more than 1.5 million associates in the United States, and stores, clubs and other facilities located within 10 miles of 90 percent of the U.S. population, Walmart is not immune to the impact of COVID-19,” said Phillip Keene, a Walmart spokesperson. The corporation has worked “to find an appropriate balance between supporting our associates and serving our customers” during the pandemic, he said, by following deep cleaning, sanitizing, and social distancing protocols guided by the CDC. Associates are given health screenings and temperature checks prior to their shifts, for example, and employees who appear ill are asked to return home. Walmart has instructed managers since March to inform associates when one of their coworkers falls ill, Keene said.
There are no laws mandating that retailers report coronavirus cases, leaving it up to stores to decide how best to handle outbreaks. In May, a delegation of state lawmakers led by Sen. Elizabeth Warren sent a letter to Walmart CEO Doug McMillon, demanding more information about how the retail giant would make changes to prevent future outbreaks and protect workers.
In its response, Walmart deflected responsibility, saying it may be “impossible to track the source of anyone’s infection.”
“Walmart’s response is unacceptable,” Warren said in a statement to BuzzFeed News. “Nearly 100 Walmart workers in Massachusetts got sick with coronavirus and one died due to an outbreak at the store but the company refused to answer questions on what happened and what changes it is making to keep our residents safe at work.”
One recent afternoon in June, as protesters filled streets across the country, a line of masked shoppers stretched outside the Worcester Walmart as the store limited capacity to around 20% below its usual level. Shelves were stocked with pasta again, apples were piled into abundant mounds, and pork ribs lay beside long rows of fresh meat. Fruit farms, meatpacking plants, and grocery stores were open for business in every corner of America. The food supply chains kept on humming. ●

Salvador Hernandez contributed reporting to this story.










